Chapter: Medical Surgical Nursing: Assessment and Management of Patients With Hematologic Disorders
Non-HodgkinŌĆÖs Lymphomas
NON-HODGKINŌĆÖS
LYMPHOMAS (NHLs)
The NHLs are a heterogeneous group of cancers that originate from the neoplastic growth of lymphoid tissue. As in CLL, the neo-plastic cells are thought to arise from a single clone of lymphocytes; however, in NHL, the cells may vary morphologically. Most NHLs involve malignant B lymphocytes; only 5% involve T lymphocytes. In contrast to HodgkinŌĆÖs disease, the lymphoid tissues involved are largely infiltrated with malignant cells.
The spread of these malignant
lymphoid cells occurs unpredictably, and true localized disease is uncommon.
Lymph nodes from multiple sites may be infiltrated, as may sites outside the
lymphoid system (extranodal tissue).
The
incidence of NHL has increased dramatically over the past decade; it is now the
fourth most common type of cancer diag-nosed in the United States and the fifth
most common cause of cancer death (Greenlee, Hill-Horton, Murray, & Thun,
2001; Zelenetz et al., 2000). The incidence increases with each decade of life;
the average age at diagnosis is 50 to 60 years. Although no com-mon etiologic
factor has been identified, there is an increased inci-dence of NHL in people
with immunodeficiencies or autoimmune disorders, viral infections (including
Epstein-Barr virus and HIV), or exposure to pesticides, solvents, or dyes.
Prognosis varies greatly among the various types of NHL. Long-term survival
(more than 10 years) is commonly achieved in low-grade, localized lym-phomas.
Even with aggressive disease forms, cure is possible in at least one third of
patients who receive aggressive treatment.
Clinical Manifestations
Symptoms
are highly variable, reflecting the diverse nature of these diseases. With
early-stage disease, or with the types that are con-sidered more indolent,
symptoms may be virtually absent or very minor, and the illness typically is
not diagnosed until it progresses to a later stage, when the patient is more
symptomatic. At these stages (III or IV), lymphadenopathy is noticeable. One
third of pa-tients have ŌĆ£B symptomsŌĆØ (recurrent fever, drenching night sweats,
and unintentional weight loss of 10% or more).
Assessment and Diagnostic Findings
The
actual diagnosis of NHL is categorized into a highly complex classification
system based on histopathology, immunophenotyp-ing, and cytogenetic analyses of
the malignant cells. The specific histopathologic type of the disease has
important prognostic im-plications. Treatment also varies and is based on these
features. In-dolent (less aggressive) types tend to have small cells and are
distributed in a follicular pattern. Aggressive types tend to have large or
immature cells distributed through the nodes in a diffuse pattern. Staging,
also an important factor, is typically based on data obtained from CT scans,
bone marrow biopsies, and occasionally cerebrospinal fluid analysis. The stage
is based on the site of dis-ease and its spread to other sites. For example, in
stage I disease, only one area of involvement is detected; thus, stage I
disease is highly localized and may respond well to localized therapy (eg,
ra-diation therapy). In contrast, stage IV disease is detected in at least one
extranodal site. Although low-grade lymphomas may not re-quire treatment until
the disease progresses to a later stage, histor-ically they have also been
relatively unresponsive to treatment in that most therapeutic modalities did
not improve overall survival. More aggressive types of NHL (eg, lymphoblastic
lymphoma, BurkittŌĆÖs lymphoma) require prompt initiation of chemotherapy;
however, these types tend to be more responsive to treatment.
Medical Management
Treatment
is based on the actual classification of disease, the stage of disease, prior
treatment (if any), and the patientŌĆÖs ability to tol-erate therapy. If the
disease is not an aggressive form and is truly localized, radiation alone may
be the treatment of choice. With aggressive types of NHL, aggressive
combinations of chemother-apeutic agents are given even in early stages. More
intermediate forms are commonly treated with combination chemotherapy and
radiation therapy for stage I and II disease. The biologic agent interferon has
been approved for the treatment of follicular low-grade lymphomas, and an
antibody to CD20, rituximab (Rit-uxan), has been effective in achieving partial
responses in patients with recurrent low-grade lymphoma. Studies of this agent
in com-bination with conventional chemotherapy have demonstrated an improvement
in survival as well (Coiffier, 2002; Emmanouilides et al., 2000; Petryk &
Grossbard, 2000). Central nervous system involvement is also common with some
aggressive forms of NHL; in this situation, cranial radiation or intrathecal
chemotherapy is used in addition to systemic chemotherapy. Treatment after re-lapse
is controversial. BMT or PBSCT may be considered for pa-tients younger than 60
years of age.
Nursing Management
Most
of the care for patients with HodgkinŌĆÖs disease or NHL is performed in the
outpatient setting, unless complications occur (eg, infection, respiratory
compromise due to mediastinal mass). For patients who require treatment,
chemotherapy and radiation therapy are most commonly used. Chemotherapy causes
systemic side effects (eg, myelosuppression, nausea, hair loss, risk for
infec-tion), whereas the side effects from radiation therapy are specific to
the area being irradiated. For example, patients receiving ab-dominal radiation
therapy may experience nausea and diarrhea but not hair loss. Regardless of the
type of treatment, all patients may experience fatigue.
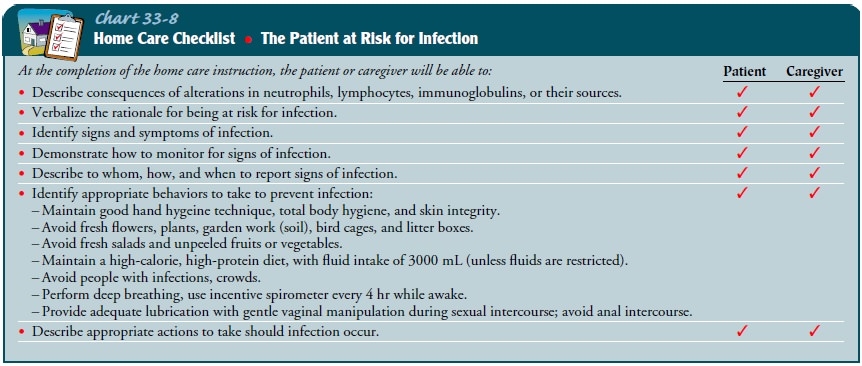
The
risk of infection is significant for these patients, not only from
treatment-related myelosuppression but also from the defec-tive immune response
that results from the disease itself. Patients need to be taught to minimize the
risks for infection, to recognize signs of possible infection, and to contact
the health care profes-sional should such signs develop (see Chart 33-8).
Many
lymphomas can be cured with current treatments. However, as survival rates
increase, the incidence of second ma-lignancies, particularly AML or MDS, also
increases. Therefore, survivors should be screened regularly for the
development of sec-ond malignancies.
Lymphoma
is a highly complex constellation of diseases. When caring for the patient with
lymphoma, it is extremely important to know the specific disease type, stage of
disease, treatment his-tory, and current treatment plan.
Related Topics