Chapter: The Massage Connection ANATOMY AND PHYSIOLOGY : Skeletal System and Joints
The Vertebral Column - Axial Skeleton
THE VERTEBRAL COLUMN
The vertebral column (see Figures 3.18–3.20) consists of 26 bones—24 vertebrae, 1 sacrum, and 1 coccyx. Together, they protect the spinal cord, maintain an upright body position, and provide support to the head, neck, and trunk. They also transmit the weight of the body to the legs and provide a surface for at-tachment of muscles of the trunk.
Vertebral Regions and Spinal Curvatures
The vertebral column is subdivided into the cervical (7 vertebrae), thoracic (12 vertebrae), lumbar (5 ver-tebrae), sacral (1 vertebrae), and coccygeal (1 verte-bra)regions. Although the cervical, thoracic, and lumbar consist of individual vertebrae, the sacrum is formed by the fusion of 5 individual vertebrae and the coccyx is formed by the fusion of 3–5 vertebrae. For ease, the vertebrae are labeled according to the position in individual regions (e.g., the 7th cervical vertebra is labeled C7; 2nd thoracic vertebra as T2; and so on.
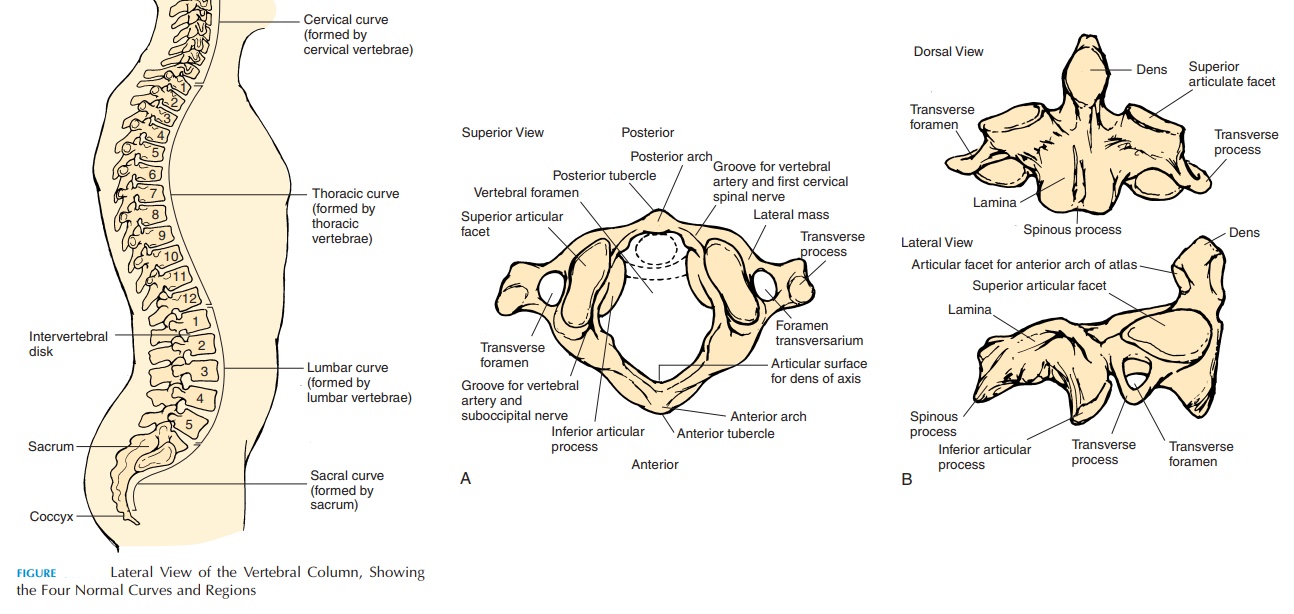
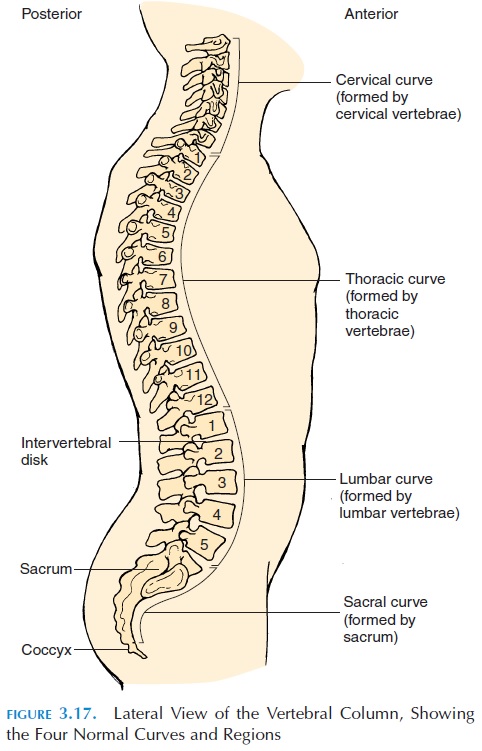
The individual vertebra of the vertebral column are aligned to form four spinal curves (see Figure 3.17)—the cervical, thoracic, lumbar, and sacralcurvature. The thoracic and sacral curvatures havethe concavity of the curve facing forward.
Each vertebra consists of three parts: the body,vertebral arch, and articular processes (see Figure3.18). The body is thick, disk-shaped, and located an-teriorly. The bodies are interconnected by ligaments. Interspersed between each vertebra are fibrocartilage pads called intervertebral disks . Two vertebral arches lead off posterolaterally from thebody. The two, short, thick processes leading off from the body are known as pedicles. The pedicles have depressions on the superior and inferior surfaces (vertebral notches). The pedicles join the laminae, the flat, posterior part of the arch. These arches meet posteriorly to enclose an opening called thevertebralforamen. Because the vertebrae lie on top of eachother, the successive vertebral foramen form a verte-bral canal. The spinal cord lies in the vertebral canal.Laterally, a small foramen is formed where the notches on the pedicles of successive vertebrae align. This is the intervertebral foramen. The spinal nerves exit from the vertebral canal through these foramen. Posteriorly, each vertebra has a projection called the spinous process. This forms the bumps that are seen in the middle of the back in a lean indi-vidual. The most prominent of these bumps at the base of the neck indicates the location of the C7 spin-ous process. C7 is, therefore, called thevertebraprominens (also see Fig. M 3).
A large elastic ligament, the ligamentum nuchae, is attached to the spinous process of C7. From here, it continues upward, attached to the spinous processes of the other cervical vertebrae before it reaches the prominent ridge on the occipital bone, the external oc-cipital crest. This ligament maintains the cervical cur-vature, even without the help of muscular contraction. If the head is bent forward, this elastic ligament helps bring the head to an upright position.
Transverse processes project laterally on bothsides. The processes are sites for muscle attachment. Each vertebrae has articular processes that project inferiorly (inferior articular process) and superi-orly (superior articular process). This is the area where adjacent vertebrae articulate. The superior ar-ticular processes of the lower vertebra articulate with the inferior articular processes of the vertebra lo-cated above. The articulating surface of the processes are known as facets.
Characteristics of Vertebraein Different Regions
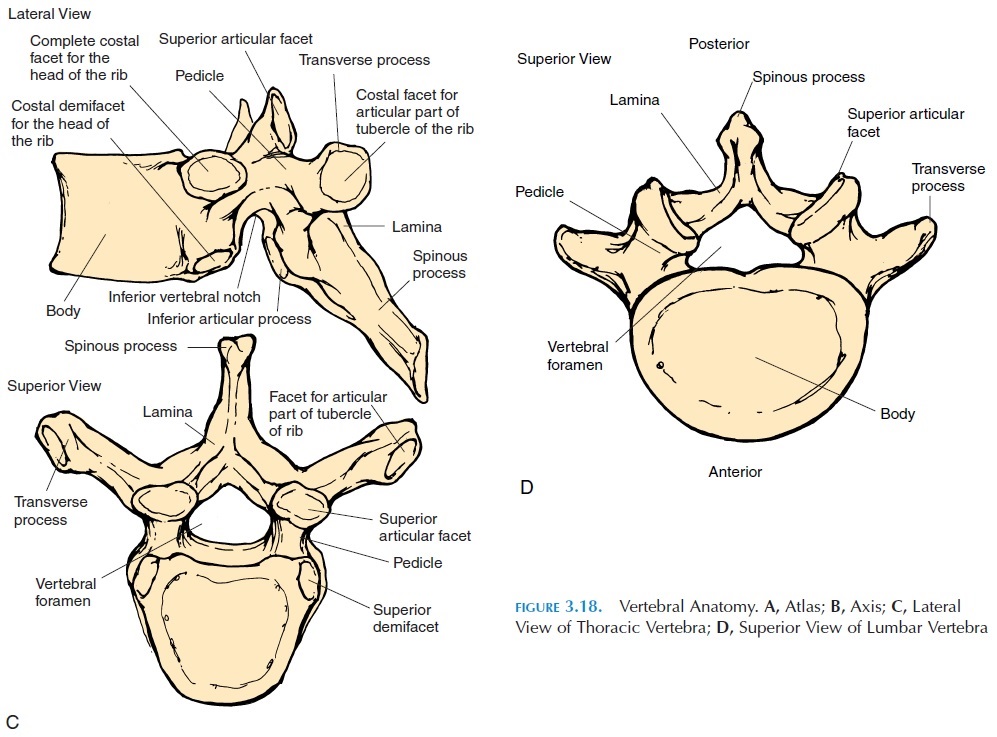
The characteristics of the vertebrae in different re-gions vary according to major function. For example, the cervical vertebrae have a large vertebral foramen because all the nerves ascending and descending from the brain form the spinal cord here. As the lower regions are approached, the vertebral foramen become smaller. This is because of the exit of spinal nerves according to the region they supply. As the spinal cord descends, more and more nerves leave; hence, the tapering appearance of the spinal cord. The cervical vertebrae are also smaller as they only must bear the weight of the head. The vertebrae in the other regions become sturdier, the lumbar being the largest (Figure 3.18D) because they have to bear more weight. The thoracic vertebrae have extra facets on the transverse processes and the body that articu-late with the ribs (Figure 3.18C). The transverse processes of the cervical vertebrae have a foramen (transverse foramen), through which the vertebral artery, vein, and nerve pass. The spinous processes of the cervical vertebrae C2–C6 are often bifid.
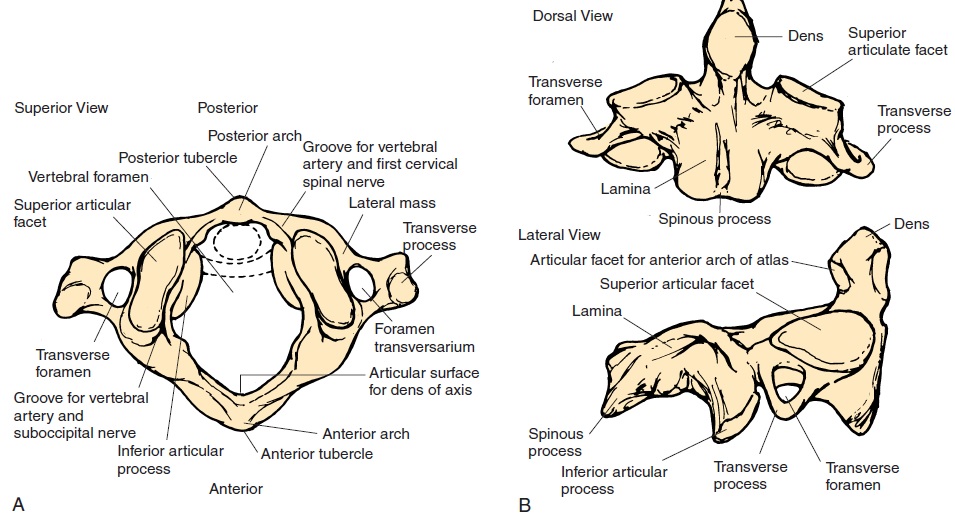
The first cervical vertebra is the atlas (Figure 3.18A) as it bears the weight of the head. It articulates with the occipital condyles of the skull. This joint—the atlanto-occipital joint—permits the nodding of the head. The atlas does not have a body and spinous process, instead it has anterior and posterior arches and a thick, lateral mass. The second vertebra is called the axis (Figure 3.18B). It has a projection (dens, or odontoid process) that projects superiorly from theregion of the body of the vertebra. This process is held in place against the inner surface of the atlas by a transverse ligament. This joint allows the head to ro-tate and pivot on the neck. The dens is actually the fu-sion of the body of the atlas with that of the axis.
Because the position of the head on the cervical vertebrae resembles a bowl being balanced on a small rod, contraction of small muscles attached to the base of the head can initiate marked changes in head posi-tion. However, these muscles, being weak, cannot fully support the head if it is jolted violently, as in a car crash. Such a jolt can result in dislocation of the cervical vertebrae and injury to the spinal cord, liga-ments, and muscles of the neck. The movement of the head in this situation resembles the lashing of a whip; hence, the name whiplash for this kind of injury.
The Sacrum
The sacral vertebrae (see Figure 3.19) begin to fuse with each other at puberty. They are completely fused between 25–30 years of age. The fused sacrum is tri-angular with the base located superiorly and the apex pointing downward. The lateral part of the sacrum has articulating surfaces for the pelvic girdle. Large mus-cles of the thigh are attached to its large surface. The sacrum also protects the lower end of the digestive tract and organs of reproduction and excretion. The upper end of the sacrum articulates with the last lum-bar vertebra. Internally, the sacral canal is a continu-ation of the vertebral canal. The nerves from the spinal cord, along with the membranes, continue along the length of the sacral canal and enter and leave the canal through the foramen in the sacrum.
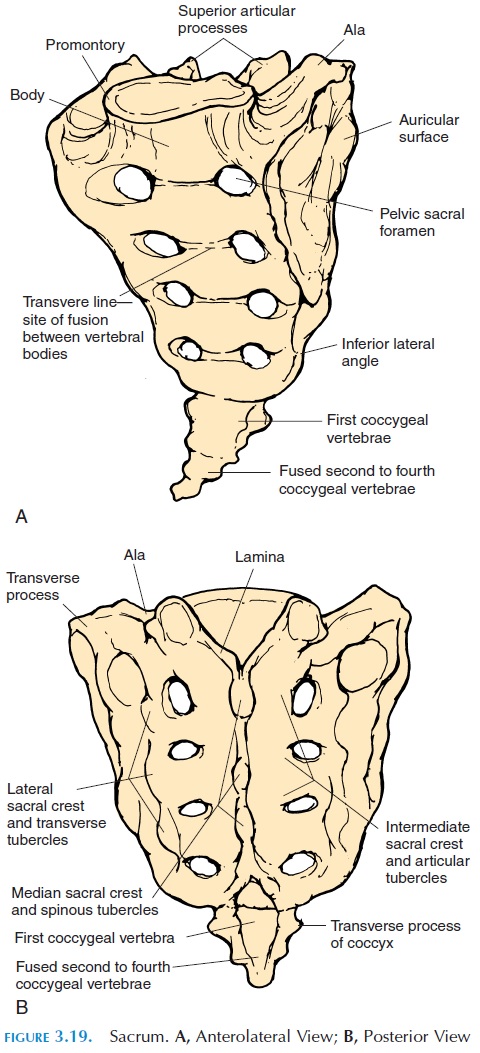
The coccyx also consists of vertebrae, which begin to fuse by about age 26. It provides attachment to lig-aments and anal muscles.
Intervertebral Disks
From the axis to the sacrum, the vertebral bodies are separated from each other by fibrocartilage called in-tervertebral disks. Each disk-shaped structure is made of a tough outer layer, the annulus fibrosus. The collagen fibers of this layer attach adjacent bod-ies of the vertebrae. The annulus fibrosus encloses a gelatinous, elastic and soft core called the nucleuspulposus. Seventy-five percent of this core is water,with scattered strands of elastic and reticular fibers. The disks serve as shock absorbers. They also allow the vertebrae to glide over each other slightly, with-out loosing alignment. Because the disks contribute to one-fourth of the length of the vertebral column, the height of the individual diminishes as the disks loose water and become narrower with age.
Disks can be compressed beyond normal limits. This can happen during a hard fall or whiplash injury or even when lifting heavy weights. If this happens, the nucleus pulposus distorts the annulus fibrosus and forces it into the vertebral canal or the intervertebral foramen. Sometimes it is the nucleus pulposus that protrudes into the canal or foramen in a condition called slipped disk, disk prolapse, or herniated disk.
The distorted disk can compress the spinal cord (in the canal) or the spinal nerves (in the foramen), leading to loss of function in areas supplied by the compressed nerves. It presents as severe backache or burning or tingling sensations in the region supplied by the nerves. Depending on the extent, control of skeletal muscle may also be lost. Some common regions where disks may prolapse are between C5–C6, L4–L5, and L5–S1.
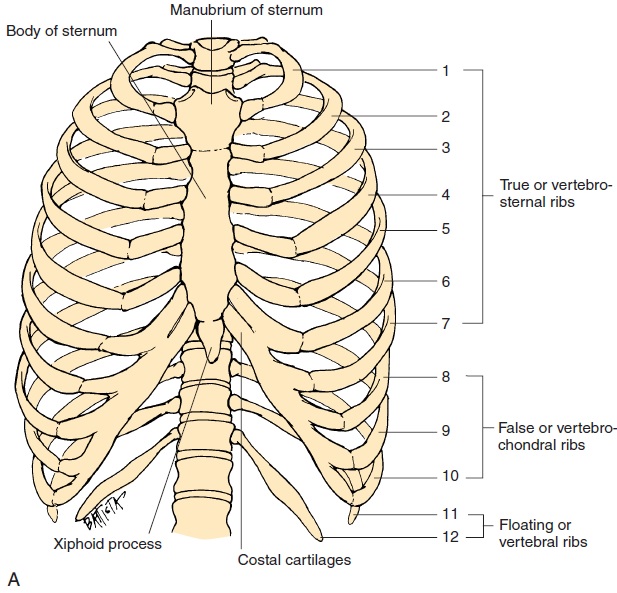
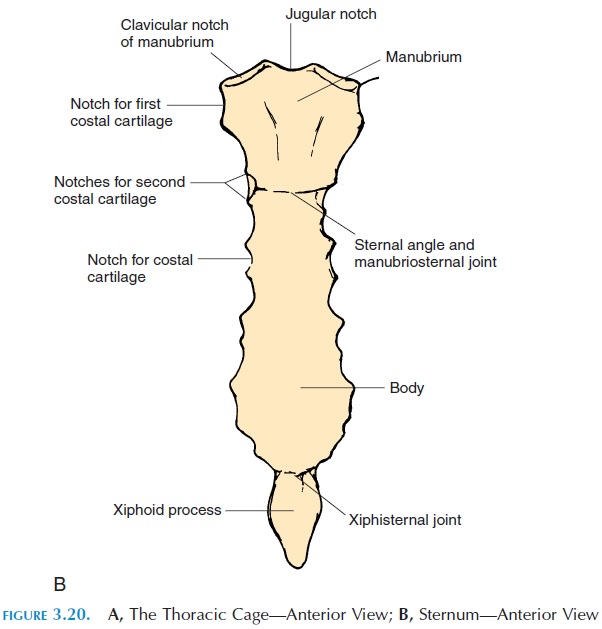
Related Topics