Chapter: The Massage Connection ANATOMY AND PHYSIOLOGY : Skeletal System and Joints
Intervertebral Articulation
INTERVERTEBRAL ARTICULATION
Articulating Surfaces and Type of Joint
Adjacent vertebrae articulate with each other via articular facets located inferiorly and superiorly. This joint is known as the zygapophyseal joints, interarticular, or facet joints (Figure 3.18). The bodies of the verte-brae also articulate with each other, with most verte-bral bodies, excluding the first and occiput, first and second cervical, and vertebrae of the sacrum and coc-cyx, being separated from each other by the interver-tebral disks.
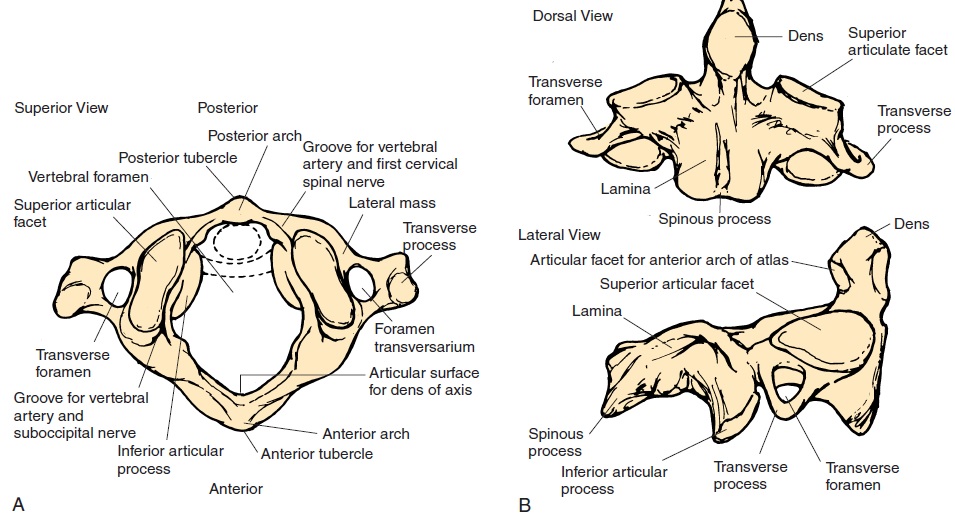
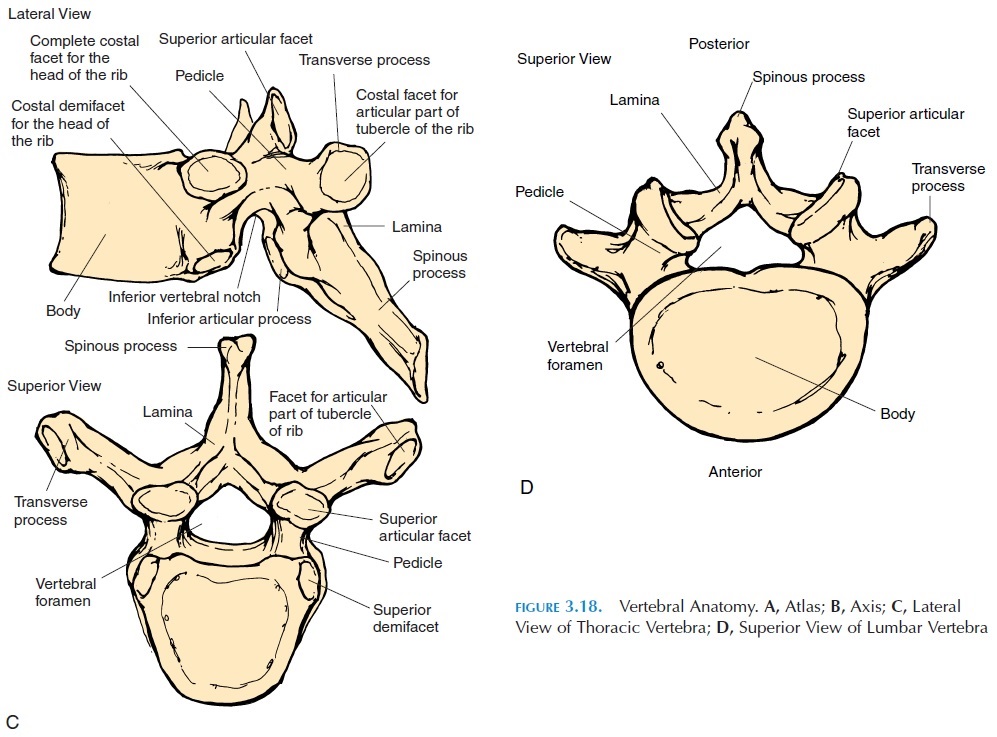
The articular surfaces of the vertebral processes are gliding joints, allowing some rotation and flexion. The articulation between the vertebral bodies is a symphyseal joint. The joint between the first cervical vertebra (atlas) and the second vertebra (axis) (at-lantoaxial joint) is a pivot joint.
The atlas has neither vertebral body nor interverte-bral disk. The axis that projects into the atlas in the re-gion where the vertebral body would be, if present, permits rotation of the ringlike atlas around it, form-ing a pivot joint. Hence, there are two atlantoaxial joints. The medial atlantoaxial joint is between the facet for dens on the atlas and the odontoid process of the axis. The lateral atlantoaxial joint is between the inferior facets of the lateral masses of the atlas and the superior facets of the axis. The superior facet of the lateral masses of the first cervical vertebra—atlas, articulates with the occipital condyles as the atlanto-occipital joint. The atlanto-occipital joint allows forflexion, extension, and lateral bending; the atlantoax-ial joints allow flexion, extension, and rotation.
Ligaments
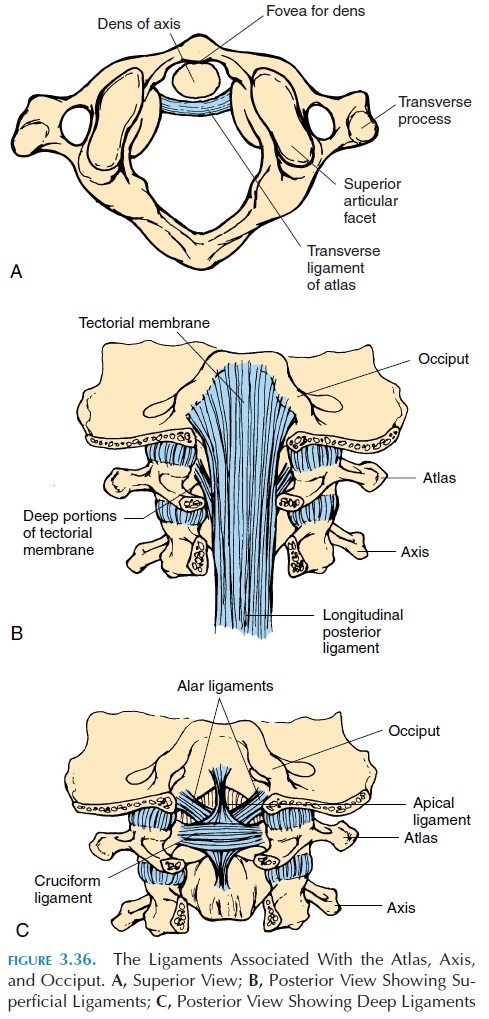
The bones are held in place by various ligaments. Fig-ure 3.36 shows the various superficial and deep liga-ments related to the atlas, axis, and occiput. The transverse ligament, alar ligament, cruciate, and api-cal ligaments stabilize the upper cervical spine and prevent damage to the brain stem by dislocation of the dens.
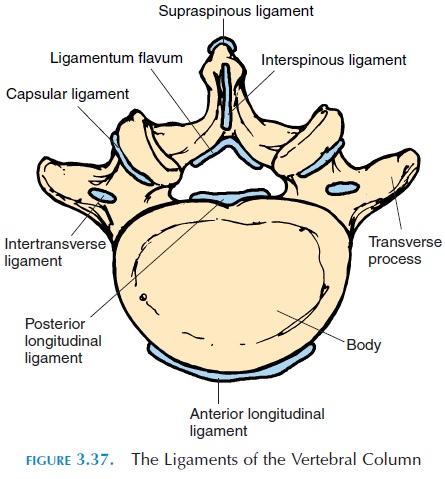
Certain ligaments (see Figure 3.37) run between the vertebral bodies and processes to help stabilize the vertebral column. The anterior longitudinal lig-ament connects the bodies of adjacent vertebra ante-riorly, while the posterior longitudinal ligament does the same posteriorly. The ligamentum flavum connects the lamina of adjacent vertebrae. Other lig-aments, known as the interspinous ligaments, con-nect adjacent spinous processes. The supraspinousligament connects the spinous processes from C7 tothe sacrum. The intertransverse ligament connects adjacent transverse processes.
Possible Movements
The vertebrae are capable of bending forward (flex-ion), bending backward (hyperextension), and side-ways (lateral flexion and rotation).
Range of Motion
Range of motion depends on the angle and size of the articulating surfaces and the resistance offered by the intervertebral disk. It also depends on the muscles and ligaments around the spine. For proper move-ment, remembered that, when one group of muscles (agonists) contract in a direction, the muscles that bring about the opposite movement (antagonists) have to relax. Similarly, the ligaments lying in the op-posite side of the movement have to stretch.
The greatest motion possible in the spine is in the lower lumbar region—between L5 and S1, where the joint surfaces are largest and disks the thickest. Con-versely, there is more chance of damage, inflamma-tion (arthritis), and herniation of disks in this region.
Cervical region
Flexion, 45° Extension, 55° Lateral bending, 40° Rotation, 70°
Lumbar region
Flexion, 75° Hyperextension, 30°
Lateral and medial bending, 35°
Muscles
The erector spinae muscles and the ab-dominal muscles help with the various spinal movements. The trapezius, scalenes, sterno-cleidomastoid, and other neck muscles help with movements in the cervical region.
The muscles of the cervical spine can be divided into four functional groups: superficial posterior, deep posterior, superficial anterior, and deep anterior. The trapezius is a major superficial posterior muscle. The levator scapulae, splenius capitis, and splenius cervicis are other large superficial muscle groups that extend the head and neck.
The multifidi and suboccipital muscles belong to the deep posterior muscle group. The multifidi, which have their origin on the transverse processes and insert into the spinous process above, extend the neck when contracted together and bend the neck to the same side when acting unilaterally.
The sternocleidomastoid is the largest and strongest anterior muscle that flexes the neck. Other neck flexors are the scalenus muscles. The deep anterior neck mus-cles are the longus coli and longus capitis.
Physical Assessment of the Spine—CervicalRegion
Inspection
The neck, the upper limb, and the upper body should be exposed to examine this region. The position of the head and movement should be noted.
Palpation
Bone and cartilage: The bone and cartilage that can be easily palpated are the hyoid bone (superior to the thyroid cartilage), the thyroid cartilage (in men, it forms the Adam’s apple), and the mastoid processes and the spinous processes of the cervical vertebrae. The C2 spinous process is the first one that can be palpated as you run your hand down from the oc-ciput.
Muscles: The sternocleidomastoid, extending from the sternoclavicular joint to the mastoid process that helps to turn the head from side to side and to flex it, is a common site of injury. Other muscles, such as the trapezius, can be palpated from origin to insertion. The superior nuchal ligament that extends from the occiput to the C7 spinous process can be easily pal-pated as well. Both active and passive range of move-ment of the neck should be tested.
Other structures: The cervical chain of lymph nodes may be palpable if enlarged. The parotid gland can also be felt as a boggy, soft swelling over the angle of the mandible if enlarged. The pulsation of the carotid arteries can be easily felt on either side of the trachea.
Because the nerves to the upper limb rise from the C5 to T1 spinal cord level, it is important to examine the functioning of the nerves. The function of the nerve can be tested by examining the sensations in the shoulder and the upper limb, as well as the strength of the muscles in the region.
Special tests (requiring specific training) test the ligaments of the upper cervical spine.
Physical Assessment of the Spine—LumbarRegion
Inspection
Watch for unnatural or awkward movement of the spine or signs of pain when the person exposes the spine when disrobing or walking
Look at the skin for swelling, redness, etc. in the region of the spine and identify abnormal curvatures of the spine.
Palpation
Bony prominences and ligaments: Posteriorly, feel the spinous processes, posterior superior iliac spine, sacrum, coccyx, iliac crests, ischial tuberosity, and greater trochanter, identifying painful areas.
Muscles: Palpate the muscles on either side of the spine and the abdominal muscles. Note tenderness, spasm, or differences in size between the right and left side.
Nerve: The sciatic nerve is an important nerve that may get compressed by spinal deformities. Palpate for tenderness in the midpoint between the ischial tuberosity and greater trochanter with the hip flexed.
Range of motion: Check flexion by asking the client to lean forward and try to touch the toes with-out bending the knee. Check extension by asking the client to bend backward with your hand on the pos-terior superior iliac spine. Check lateral bending by asking the client to lean to the right and the left as far as possible. Rotation is checked by turning the trunk to the right and left with the pelvis stabilized.
Related Topics