Chapter: The Massage Connection ANATOMY AND PHYSIOLOGY : Skeletal System and Joints
Structure and Formation of Bone
STRUCTURE AND FORMATION OF BONE
Bone is a special form of connective tissue. Similar to other connective tissue, it has ground substance with collagen fibers and cells . However, the ground substance in bone has a large deposition of calcium and phosphorus that makes the tissue hard and rigid. The minerals are in the form of hydroxya-patite crystals (calcium carbonate and calciumphosphate mineral salts). Minerals account for 60% to 70% of the dry weight of bone; water accounts for 5% to 8%; and organic matter, the remaining weight. The collagen fibers are arranged in various direc-tions, with the arrangement being altered according to lines of stress and tension created by the weight and activity of the body. The presence of collagen fiber gives bone its flexibility and resilience. Collagen fibers and minerals combined make the bone flexible, compressible, and able to withstand considerable shear forces. The gel-like ground substance that sur-rounds the collagen fibers is made up of large, com-plex molecules called proteoglycans. Proteoglycans are mucopolysaccharides bound to protein chains.
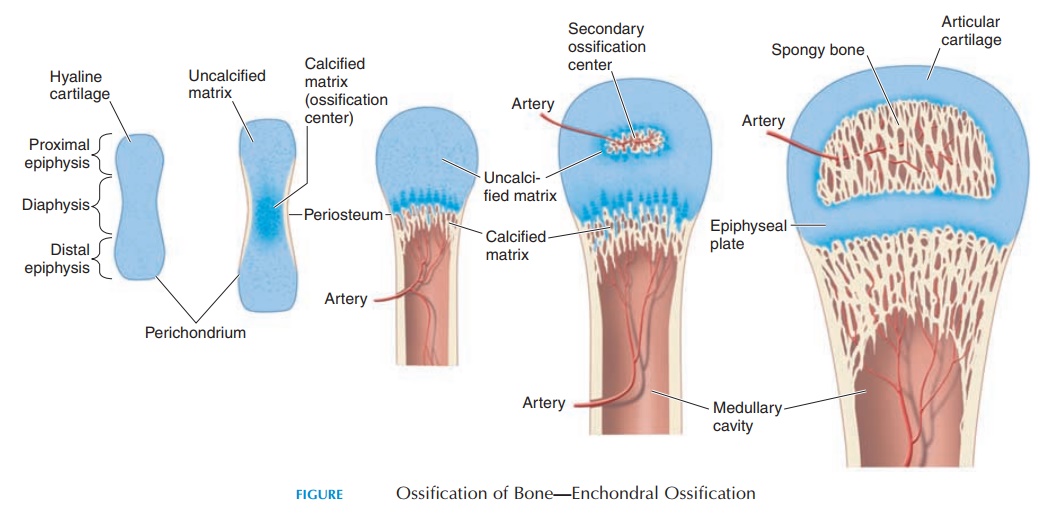
Like all tissue, bone requires its own supply of blood and nerves. Unlike other softer tissue, bone is solid and must grow around blood vessels and nerves in a more complex process. To better understand this complex process, bone formation in the fetus must be examined. The process of bone formation is known as ossification, osteogenesis, or calcification (see Figure 3.1). Ossification may occur in two ways. In intramembranous ossification, bone is formedwithin or on fibrous connective tissue membranes. Flat bones of the skull and mandible are formed by intramembranous ossification. In endochondral os-sification, the more common type of ossification,bone is formed within hyaline cartilage.
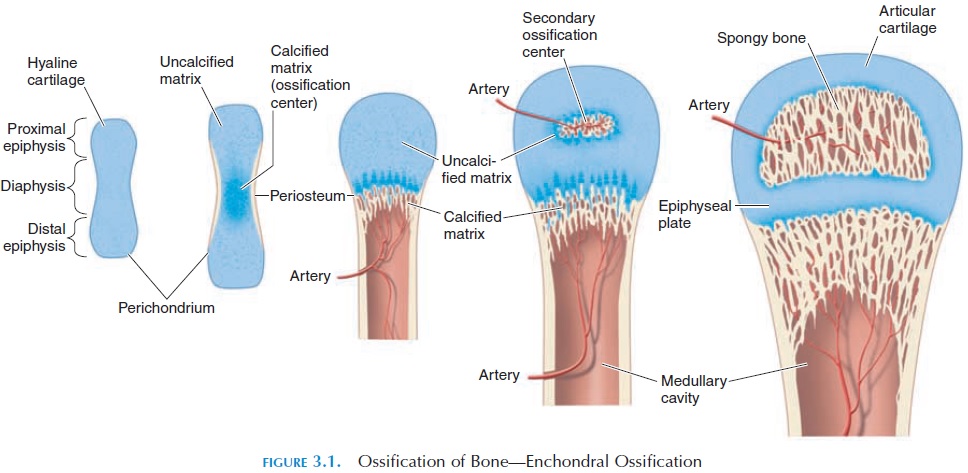
In the fetus, special cells known as chondroblasts appear in areas where bone must be present. Chon-droblast secretions result in the formation of carti-lage, which eventually takes the precise shape of bone in that area. In this way, cartilage forms a mold in which minerals can be deposited to form bone. The connective tissue around the cartilage forms a highly vascular membrane around the mold. Nerves are also incorporated in the membrane. The mem-brane has many chondroblasts, which help cartilagi-nous growth on the surface of the model. This mem-brane is known as the perichondrium.
At a later stage, chondroblasts undergo transfor-mation and begin to secrete the chemicals that pre-cipitate deposition of minerals around them. The transformed cells are osteoblasts.
The chondroblasts in the membrane are also trans-formed and bone begins to form both inside and on the surface of the cartilage model.
The beginning and rate of ossification varies from bone to bone. In each bone, ossification may begin at different sites known asossification centers. Ossifi-cation continues until the cartilage model has been replaced by bone. The bone has the potential to grow in length as long as adjacent ossification centers have not fused together. Once fused, the bone can only be-come thicker.
A typical bone has a hard outer shell, with a blood and nerve supply known as the periosteum, which is actually ossified perichondrium. Because the blood and nerve supply are located here, the periosteum is an important component of bone. It also houses the osteogenic cells (cells that divide to form os-teoblasts) and osteoblasts that are required for new bone formation on the surface, according to stresses and strains placed on the bone. The fusion of bones that occur in some regions of the body is also a result of the presence of periosteum. In addition, ligaments that cross joints are fused with the periosteum of ad-jacent bones, adding to joint stability. Tendons of muscles also blend with the collagen fibers of the periosteum at the point of attachment.
Related Topics