Chapter: Ophthalmology: Cornea
Mycotic Keratitis
Mycotic Keratitis
Epidemiology:
Mycotic keratitis was once very rare, occurring almost
exclu-sively in farm laborers (see Etiology for contact with possible causative
agents). However, this clinical syndrome has become far more prevalent today as
a result of the increased and often unwarranted use of antibiotics and
steroids.
Etiology:
The most frequently encountered pathogens areAspergillusandCandida albicans. The most frequent causative mechanism is an
injury withfungus-infested organic materials such as a tree branch.
Symptoms:
Patients usually have only slight symptoms.
Diagnostic considerations:
The red eye is apparent uponinspection(nor-mally
the disorder is unilateral), as is a corneal ulcer with an undermined
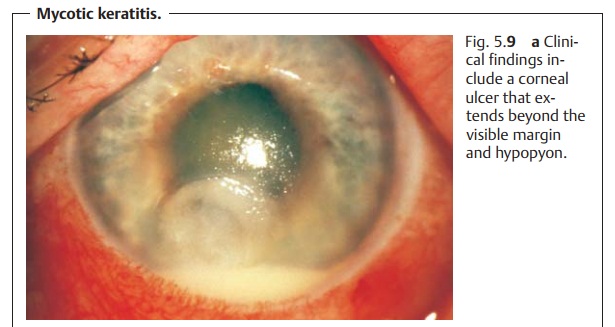
margin (Fig. 5.9). The ulcer will continue to expand beneath
the visible mar-gins (serpiginous corneal ulcer). Hypopyon may also be present
(as shown in Fig. 5.9a). Slit lamp examination will reveal typical whitish stromal infil-trates,
especially with mycotic keratitis due to Candida
albicans. The infil-trates and ulcer spread very slowly. Satellite lesions, several adjacent
smaller infiltrates grouped around a larger center, are characteristic but will
not nec-essarily be present.
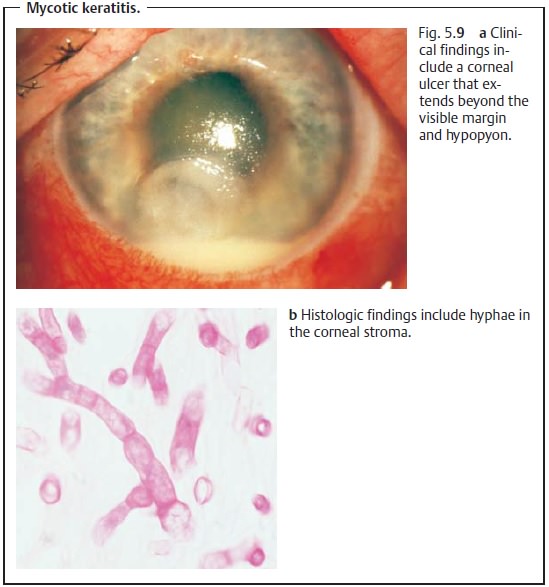
Identification of the pathogen.Microbiologicalidentification of fungi is diffi-cult and can be time consuming (for histologic identification, see Fig. 5.9b). It is important to obtain samples from beyond the visible margin of the ulcer. Fun-gal cultures should always be obtained where bacterial cultures are negative.
Treatment:
Conservative treatment.Hospitalizationis recommended when beginningtreatment as the
disorder requires protracted therapy. Systemic therapy is only indicated in the
case of an intraocular involvement. Other cases will respond well to topical
treatment with antimycotic agents such as natamycin, nystatin, and amphotericin
B. In general, the topical antimycotic agents will have to be specially
prepared by the pharmacist.
Surgical treatment.Emergency keratoplasty is indicated whenthe disorder fails to
respond or responds too slowly to conservative treatment and findings worsen
under treatment.
Related Topics