Chapter: Ophthalmology: Cornea
Corneal Surgery
Corneal Surgery
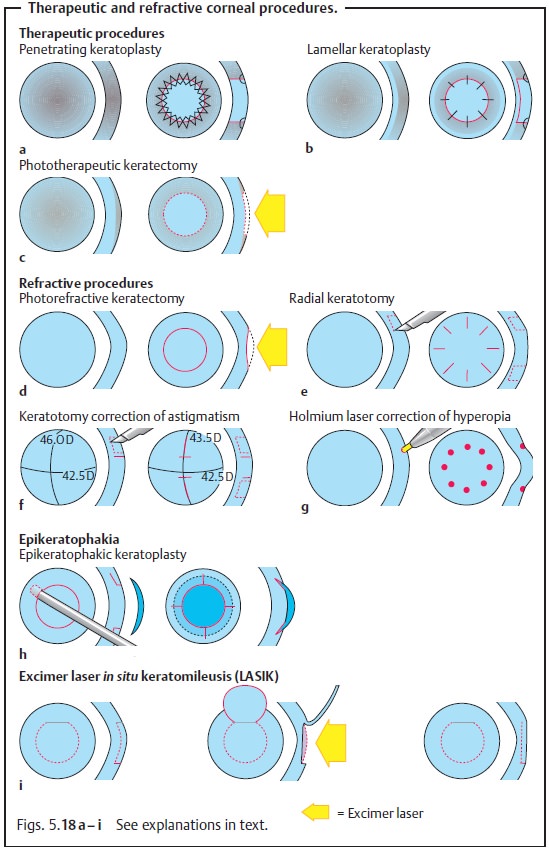
Corneal surgery includes curative or therapeutic procedures and refractive procedures (Fig. 5.18).
❖ Curative corneal procedures are intended to improve vision by eliminatingcorneal opacification.
❖ Refractive corneal procedures change the refractive power of aclearcornea.
Curative Corneal Procedures
Penetrating Keratoplasty (Fig. 5.18a)
Principle: This involves replacement of diseased corneal tissue with a
full-thickness donor graft of corneal tissue of varying diameter. A clear, regularly
refracting button of donor cornea is placed in an opacified or irregularly
refracting cornea. The corneal button is sutured with a continuous single or
double suture (Fig. 5.19) or with
interrupted sutures. (For special considera-tions in corneal transplants, see
also Morphology and healing.)
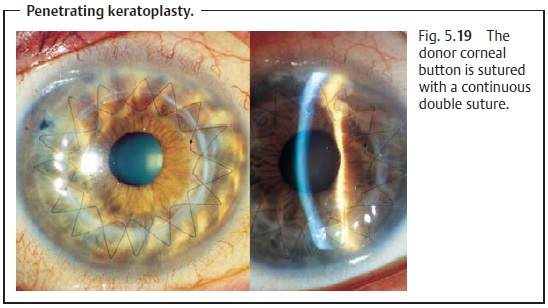
Penetrating keratoplasty can be performed as
an elective procedure to improve visual acuity or as an emergency procedure (emergency kerato-plasty). Emergency keratoplasty is indicated to treat a perforated or
nonheal-ing corneal ulcer to remove the perforation site and save the eye (tectonic ker-atoplasty).
Indications: Corneal diseases that affect the full thickness of the
cornealstroma (corneal scars, dystrophy, or degeneration) or protrusion
anomalies such as keratoconus or keratoglobus with or without central corneal
opacification.

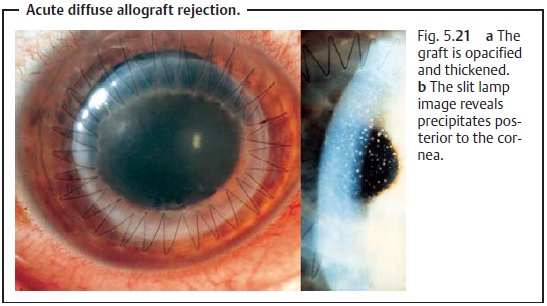
Allograft Rejection (Complications): The body’s immune system canrespond with a chronic focal allograft rejection (Fig. 5.20) or a diffuse allograft rejection (Fig. 5.21). The graft will be become opacified.
Lamellar Keratoplasty (Fig. 5.18b)
Principle: This involves replacement of a superficial stromal
opacificationwith a partial-thickness donor graft of clear corneal tissue.
This surgery requires the corneal epithelium, Descemet’s membrane, and the deeper layers of the cornea to be intact and healthy as it is only suitable for removing superficial opacifications down to about the middle of the cornea. The donor corneal button is then sutured with one or two continuous sutures or with interrupted sutures.
Indications: Corneal opacifications and scars affecting the superficial
cornealstroma (post-traumatic, degenerative, dystrophic, or postinflammatory
opacifications). This method is not suitable for treating corneal ulcers.
Allograft Rejection (Complications): Allograft rejection is less frequent thanin
the case of penetrating keratoplasty. There is also less danger of infection as
lamellar keratoplasty does not involve opening the globe.
Phototherapeutic Keratectomy (Fig. 5.18c)
Principle: Superficial corneal scars can be ablated with an excimer
laser(wavelength of 193 nm). The lesion is excised parallel to the surface of
the cor-nea to avoid refractive effects. The edges of the ablated area are
merged smoothly with the rest of the corneal surface, eliminating any
irregularities.
Indications: Indications are identical to those for lamellar
keratoplasty.However, this method is only suitable for ablation of relatively
superficial cor-neal opacifications, i.e., in the upper 20% of the corneal
stroma.
Disadvantage: Despite attempting ablation parallel to the surface of the
cor-nea, phototherapeutic keratectomy often creates a hyperopic effect.
Refractive Corneal Procedures
Photorefractive Keratectomy (Fig. 5.18d)
Principle: Tissue is ablatedto change the corneal curvature and to achieve arefractive
correction. Flattening the corneal
curvature corrects myopia, whereas steepening the curvature corrects hyperopia. The amount of
tissue removed at different sites can be varied with layer-by-layer excimer
laser ablation and the use of apertures. This makes it possible to correct for
myopia, by removing more tissue from the center of the cornea, or for
hyperopia, by removing more tissue from the periphery.
Indications: Best results are achieved in correcting myopia of less than
6diopters. At present stable correction can be achieved in 85 – 95% of all
cases of myopia up to !6 diopters, with deviation of !1 diopter from the target within one year. Correction of
hyperopia has also been attempted.
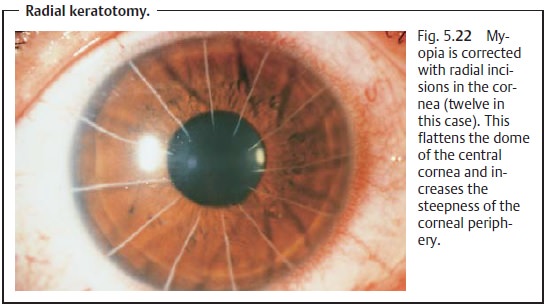
Radial Keratotomy (Fig. 5.18e)
Principle: Correction of myopia byflattening
the central dome of the corneawith four to sixteen radial incisions
extending through as much as 90% of the thickness of the cornea. This increases
the steepness of the corneal periphery and lowers the center of the cornea,
reducing its refractive power. This method does not influence the optical
center of the cornea (Fig. 5.22).
Indications and prognosis: The method is suitable for moderate myopia(less than 6 diopters). The effect achieved is influenced by the initial refrac-tion, intraocular pressure, corneal thickness, and the patient’s age and sex. A disadvantage is refractive fluctuations of up to 1.5 diopters during the course of the day. In one-fifth of all cases refraction becomes unstable within a year.
Photorefractive Keratectomy Correction of Astigmatism
Principle: Surgicalreduction of
severe regular astigmatismby flattening thesteep meridian in the center of
the cornea by increasing the steepness of the corneal periphery. Irregular astigmatism cannot be
corrected.
Indication: Severeregularastigmatism.
Holmium Laser Correction of Hyperopia
Principle: The laser is focused on the corneal stroma to create
shrinkageeffects. Placing these areas symmetrically steepens the central
cornea, which can correct severe hyperopia.
Indication: Hyperopia correction up to 8 diopters.
Epikeratophakic Keratoplasty (Epikeratophakia)
Principle: Severe myopia and hyperopia are corrected by suturing
speciallyprepared hyperopic or myopic partial-thickness corneal grafts on to
the recipient’s cornea. This involves special trephination and preparation of
the recipient’s cornea. The donor graft is then fitted into the prepared cornea
and sutured in place. The donor corneal button is prepared as a frozen section and
shaped to the required refractive power; these implants can be ordered from eye
banks.
Indications: Any severity of hyperopia or myopia can be corrected.
Excimer Laser in situ Keratomileusis (LASIK)
Principle: Myopia is corrected with preservation of Bowman’s layer. A
super-ficial corneal flap (approx. 160 µm) is created with
a microkeratome. The ker-atome is withdrawn, the flap is reflected, and the
exposed underlying corneal stroma is ablated with an excimer laser to correct
the myopia. Then the flap is repositioned on the corneal bed and fixed in place
by force of its own adhe-sion.
Indication: Even severe myopia (up to 10 – 12 diopters) can be corrected withthis method.
Related Topics