Chapter: Case Study in Obstetrics and Gynaecology: General Gynaecology
Case Study Reports: Pelvic Pain
PELVIC PAIN
History
A
24-year-old woman presents with pelvic pain
and painful sexual
intercourse for 2 years
and is worried that she may have an ovarian
cyst or other gynaecological problem.
The pain occurs at any time of the menstrual cycle
but is worse during menstruation. It can also be worse when
she passes urine
or opens her
bowels. There is no relation to exercise.
She
has been with her current
sexual partner for 6 months
and the pain occurs nearly every time she has
intercourse unless penetration is very gentle.
She has never
been diag- nosed with any sexually
transmitted infections. She has been pregnant once at the age of 19 years but this ended in a spontaneous complete
miscarriage.
She
opens her bowels
regularly and denies
any bloating, constipation, diarrhoea or mucus in the stool. She
had an episode
of cystitis a few years
ago which responded to antibiotics.
There is no other medical history of
note and she takes no regular medications.
Examination
The
abdomen is not distended and there is no organomegaly. No masses are palpable but there is suprapubic tenderness. Speculum examination shows a normal smooth grey/white coloured discharge and swabs
are taken. The uterus is anteverted but has limited
mobility and is tender
on movement. There
are no adnexal
masses but the
adnexae are tender.
Questions
·
What is the diagnosis?
·
How would you manage this patient?
·
What are the long-term
implications of this disease?
Answer:
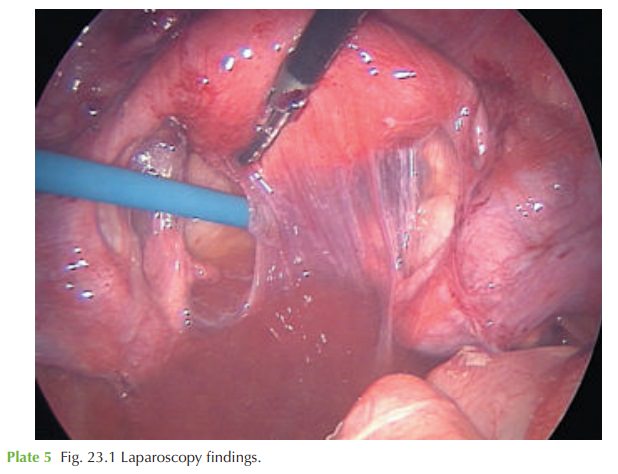
The
laparoscopy image shows
in Fig. 23.1 pelvic adhesions suggestive of previous
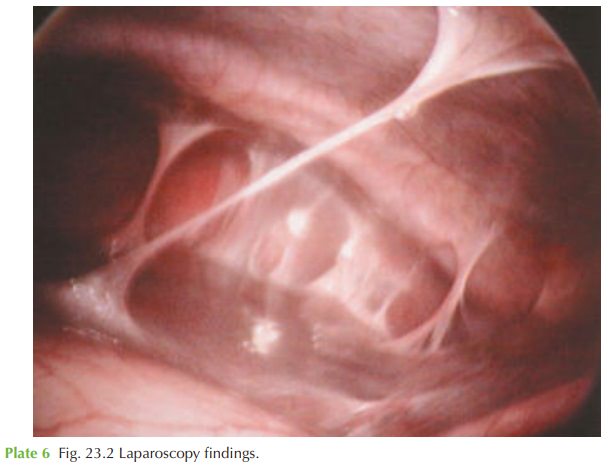
infec- tion. The ‘violin-string’ perihepatic adhesions in Fig. 23.2 are classical of Fitz-Hugh–Curtis
syndrome, generally seen with previous
chlamydial infection though
also described with gonorrhoea. These findings can
develop in the
absence of a clinically recognized infective episode.
The
woman therefore has chronic pain from pelvic
inflammatory disease. Negative
swabs would suggest that she may no longer
be infected with chlamydia.
Management
The pain may be helped with laparoscopic
adhesiolysis. The perihepatic adhesions should be ignored as they are not causing symptoms. Otherwise pain-management options
are analgesics or possible
uterosacral nerve ablation.
Even though there is no evidence of current active
infection, the tests
have limited sensi- tivity so it is worthwhile treating
the woman and her partner
with a course of antibiotics for pelvic inflammatory disease.

Related Topics