Chapter: Case Study in Obstetrics and Gynaecology: General Obstetrics
Case Study Reports: Antenatal Screening
ANTENATAL SCREENING
History
A
woman aged 23 years is referred by her general
practitioner to the antenatal clinic at
14 weeks in her first pregnancy. She has booked late having only just discovered she is
pregnant. Although the
pregnancy was unplanned she is now
happy about it.
She sepa- rated from
her partner of 2 years
a few weeks ago but
is supported by her family
and friends. She has
no significant medical
history and is one of four siblings. On direct ques- tioning her mother apparently had a stillbirth attributed to some
form of congenital abnormality 28 years ago.
Otherwise the pregnancy is assessed to be low
risk.
As
she is too late for a nuchal
translucency test she is offered
serum screening for Down’s
syndrome, which she agrees to. This is performed at 17 weeks.
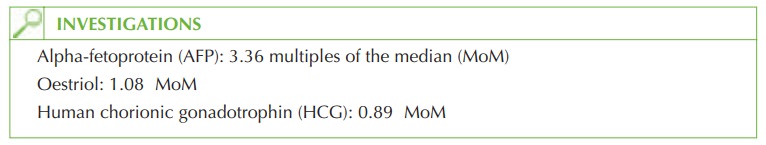
Questions
·
How
should she be counselled and what further
options are available?
·
If
the pregnancy is not affected with a fetal
abnormality, how else
could this test
result be explained?
Answers:
AFP, oestriol and
β-HCG are used
in combination in the ‘triple
test’, one of the serum- screening tests available to detect Down’s
syndrome. The results
are expressed as mul-
tiples of the median (MoM)
and in this case the AFP is significantly raised.
Down’s syndrome is associated with decreased AFP, increased oestriol and increased
β-HCG.
Increased AFP is associated with an increased
risk of fetal abnormality, the commonest
being:
·
neural tube defects
·
anterior abdominal wall defects
·
Patau’s syndrome (trisomy 13).
The
woman should be counselled that the risk of Down’s
syndrome is low but that the
blood test suggests a possible increased risk of the other
abnormalities described.
She
should be referred
to a specialist fetal medicine centre for a detailed ultrasound scan to
exclude any significant neural tube or abdominal
wall defects. Depending on the ultrasound
result, she may wish to terminate the pregnancy
if a serious abnormality is detected,
or to continue but with appropriate geneticist and paediatric input antenatally to prepare
for the delivery.
One
of the problems with serum screening is that other
pregnancy complications may
lead to a higher level of AFP. These include:
·
multiple pregnancy
·
fetal intrauterine growth restriction
·
oligohydramnios.
AFP
is also affected
by ethnic background, maternal diabetes and maternal liver
disease. Finally the normal range is dependent on gestation, and unless the gestational age has
been confirmed, the
AFP may be high because
the pregnancy is more advanced than presumed.
Related Topics
