Chapter: Case Study in Obstetrics and Gynaecology: Peripartum Care and Obstetric Emergencies
Case Study Reports: Absent Fetal Movements
ABSENT FETAL MOVEMENTS
History
A
34-year-old woman at 32 weeks
and 4 days’ gestation in her first
pregnancy complains of reduced
fetal movements. She normally feels
the baby move more than 10 times each day
but yesterday there were only two movements
and today there have been none. She has no significant medical, obstetric
or gynaecological history. In this pregnancy she booked at 10 weeks’ gestation
and all her booking blood tests were normal except that
she was discovered not to be immune
to rubella and
postnatal vaccination was
planned. Her 11–14-week scan, nuchal translucency test and anomaly
scan were all normal.
Examination
The
blood pressure is 137/73 mmHg and pulse
93/min. She is apyrexial. The symphysio-
fundal height of the uterus
is 31 cm and the fetus
is breech on examination. The fetal heart is
auscultated with hand-held Doppler and no heartbeat is heard. An ultrasound scan
is therefore arranged immediately, which confirms the
diagnosis of intrauterine fetal death.
Questions
·
How should this case be managed?
·
Are
there any factors
in the history
or examination to indicate the
cause of fetal
death and what investigations should be performed to establish a possible cause?
Answer:
Immediate management
The
baby needs delivery
to avoid the possibility of sepsis or disseminated intravascular coagulopathy developing. This is normally
achieved by induction of labour with mifepris-
tone (an antiprogestogen) followed 48 h later
by misoprostol (a prostaglandin analogue) to induce contractions. The woman can go home temporarily after the mifepristone to avoid the added stress from being on an antenatal
or postnatal ward.
In
labour, adequate analgesia is essential and
patient-controlled analgesia (PCA)
is useful.
Rarely there are contraindications to vaginal delivery, such as previous
Caesarean sec- tions, in which case operative delivery
may be necessary.
The
couple should be seen as soon as possible by a bereavement midwife to discuss
the loss, funeral or cremation plans.
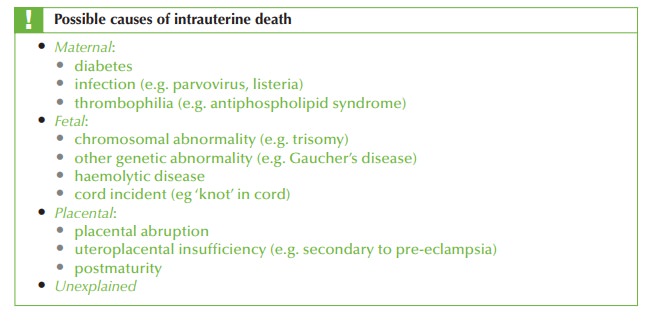
Cause of intrauterine death
In
this history the
only potentially significant factor is the
lack of rubella
immunity. This is unlikely to be significant, but rubella immunoglobulin (IgG) should be checked to exclude recent infection.
The
examination is normal except for the tachycardia, which may relate to anxiety
and should be rechecked.
Investigations
·
Maternal:
·
full blood count and coagulation
screen (to exclude disseminated intravascular
coagulopathy/thrombocytopenia secondary to fetal death)
·
random blood glucose and haemoglobin (Hb)A1c
·
Kleihauer test (for fetal cells in the maternal
circulation, implying significant fetomaternal haemorrhage)
·
anticardiolipin and lupus anticoagulant (for antiphospholipid syndrome)
·
Fetal:
·
swabs for microscopy, culture
and sensitivity from the fetus
and placenta
·
skin biopsy for karyotype
·
post mortem (if agreed by parents)

Related Topics