Chapter: Clinical Anesthesiology: Anesthetic Management: Anesthesia for Patients with Cardiovascular Disease
Calculating Aortic Valve Area & Transvalvular Gradient
CALCULATING AORTIC VALVE AREA & TRANSVALVULAR GRADIENT
As with mitral stenosis, the pressure
gradient across the aortic valve can be determined noninvasively using
continuous wave Doppler echocardiography:
∆P =4V2
where ∆P is the peak pressure gradient (mm Hg)
and V is peak blood flow velocity
(m/s) distal to the obstruction. Peak velocities greater than 4.5 m/sec are
usually indicative of severe stenosis. Moreover, if the area proximal to the
stenosis (LVOT) can be measured, the continuity equation can then be applied to
estimate valve area. Either TVIs or maxi-mum velocities can be used:
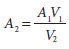
where A2 is valve area, A1 is the cross-sectional area of the
LVOT, V1
is maximum blood flow velocity in LVOT, and V2 is maximum flow velocity through the aortic valve.
Treatment
Once symptoms develop, most patients,
with-out surgical treatment, will die within 2–5 years. Percutaneous balloon
valvuloplasty is generally used in younger patients with congenital aortic
stenosis; it can also be used in elderly patients with calcific aor-tic
stenosis who are poor candidates for aortic valve replacement. Its efficacy for
the latter group is short-lived, however, and restenosis usually occurs within
6–12 months. Catheter-delivered aortic valves are increasingly being perfected
and deployed in the treatment of aortic valve disease. Surgical replace-ment of
the stenotic aortic valve remains the main-stay of therapy.
Anesthetic Management
A. Objectives
Maintenance of normal sinus rhythm,
heart rate, vascular resistance, and intravascularvolume is critical in
patients with aortic stenosis. Loss of a normally timed atrial systole often
leads to rapid deterioration, particularly when associated with tachycardia.
The combination of the two (AF with rapid ventricular response) seriously
impairs ventricular filling and necessitates immediate car-dioversion. The
reduced ventricular compliance also makes the patient very sensitive to abrupt
changes in intravascular volume. Many patients behave as though they have a
fixed SV in spite of adequate hydration; under these conditions, car-diac
output becomes very rate dependent. Extreme bradycardia (<50 beats/min) is therefore poorly tolerated. Heart
rates between 60 and 90 beats/min are optimal in most patients.
B. Monitoring
Close monitoring of the ECG and blood
pressure is crucial. Monitoring for ischemia is complicated by baseline
ST-segment and T-wave abnormali-ties. Intraarterial pressure monitoring is
desir-able in patients with severe aortic stenosis, as many of these patients
do not tolerate even brief episodes of hypotension. Pulmonary artery
cath-eterization data should be interpreted carefully; a higher than normal
pulmonary capillary wedge pressure is often required to maintain adequate left
ventricular end-diastolic volume and car-diac output. Prominent a waves are often visible on the
pulmonary artery wedge pressure wave-form. Vasodilators should generally be
used cau-tiously because patients are often very sensitive to these agents. TEE
can be useful in these patients for monitoring ischemia, ventricular preload,
contractility, valvular function, and the effects of therapeutic interventions.
C. Choice of Agents
Patients with mild to moderate aortic
stenosis (gen-erally asymptomatic) may tolerate spinal or epidural anesthesia.
These techniques should be employed very cautiously, however, because
hypotension readily occurs as a result of reductions in preload, afterload, or
both. Epidural anesthesia may be pref-erable to single-shot spinal anesthesia
in many situ-ations because of its slower onset of hypotension, which allows
more timely correction. Continuous spinal catheters can similarly be used to gradually
increase the level of regional anesthesia and limit the possibility of blood
pressure collapse. Spinal and epidural anesthesia are relatively
contraindicated in patients with severe aortic stenosis.
In the patient with severe aortic
stenosis the choice of general anesthetic agents is less impor-tant than
managing their hemodynamic effects. Most general anesthetics can produce both
vaso-dilation and hypotension, which require treatment post induction. If a
volatile agent is used, the con-centration should be controlled to avoid
excessive vasodilatation, myocardial depression, or loss of normal atrial
systole. Significant tachycardia and severe hypertension, which can precipitate
isch-emia, should be treated immediately by increasing anesthetic depth or
administration of a β-adrenergic blocking agent. Most patients with
aortic stenosis tolerate moderate hypertension and are sensitive to
vasodilators. Moreover, because of an already precarious myocardial oxygen
demand–supply bal-ance, they tolerate even mild degrees of hypotension poorly.
Hypotension should generally be promptly treated with escalating doses (25–100
mcg) of phen-ylephrine. Intraoperative supraventricular tachy-cardias with
hemodynamic compromise should be treated with immediate synchronized
cardioversion. Frequent ventricular ectopy (which often reflects ischemia) is
usually poorly tolerated hemodynami-cally and should be treated. Amiodarone is
generally effective for both supraventricular and ventricular arrhythmias.
Related Topics