Chapter: The Massage Connection ANATOMY AND PHYSIOLOGY : Cardiovascular System
Blood Types
BLOOD TYPES
The cell membrane of red blood cells contains a variety of glycoproteins and glycolipids (antigens) that can provoke antibody formation. In the blood, these antigens are referred to as agglutinogens; the antibodies as agglutinins. Based on the presence of certain agglutinogens, blood is classified into different blood groups, such as ABO grouping and Rh group-ing. Humans have more than 24 blood groups; how-ever, ABO grouping and Rh grouping are the major groups. There may be many blood types in each group.
ABO Grouping
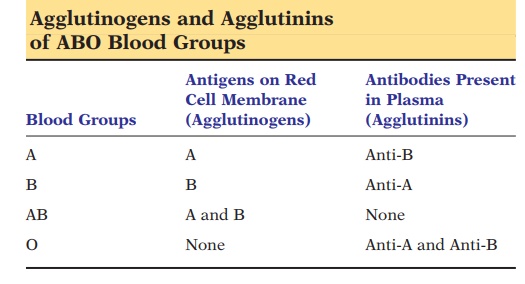
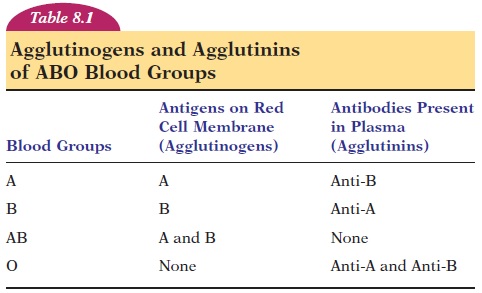
In the ABO group, there are two important antibody-provoking antigens—the A and B agglutinogens. Based on the presence or absence of these antigens, individuals are divided into 4 major blood types—A,B, AB, and O. Individuals with type A have the Aantigen on the red blood cell membrane; individuals with type B have B antigen; individuals with type AB have both antigens on the cell membrane; and indi-viduals with type O have neither antigen on the cell membrane. A and B antigens have been found in other tissue, such as salivary glands, saliva, pancreas, kidney, liver, lungs, testes, and semen.
In general, antibodies against antigens are inher-ited or developed upon exposure to the antigens. In the blood, the antibodies (agglutinins)against A and B antigens areinherited. Therefore, in-dividuals who are blood type A have antibodies against B antigen (anti-B antibodies) in their plasma; individuals with type B have antibodies against A antigen (anti-A antibodies); and individuals with type O have antibodies against both A and B antigens (anti-A and anti-B antibodies). Individuals with type AB do not have antibodies against A and B antigens because they possess both antigens (see Table 8.1).
Importance of Blood Grouping
Blood or blood components are often transferred from one person to another by a process known as blood transfusion. When a person is exposed to awrong blood type, the antigens and antibodies react with each other. This results in clumping of red blood cells—the red cells are closely drawn to each other. The clumping of blood cells resulting from an antigen-antibody reaction is called agglutination. These red cell clumps can block capillaries and re-duce blood flow to tissue, with serious consequences. In addition, all immune reactions are triggered with activation of the complement system, release of chemical mediators, and even anaphylaxis.
The clumps are also hemolyzed (broken down) to re-lease hemoglobin into the plasma. Free hemoglobin in the plasma can increase the viscosity of blood, block the glomeruli of the kidneys, and lead to kidney failure.
For example, agglutination of blood cells can hap-pen if A type blood is transfused into a person of B type. This is because the B type person has existing an-tibodies against A antigen in the plasma. What do you think will happen if a person of O blood type is given the blood of an A group, B group, or AB group individ-ual? Yes, there will be agglutination because the O group person already has antibodies against A and B antigen in their plasma. Now, identify what blood type can be given to a person belonging to AB blood group. Can blood type A be given? Yes, as the recipient plasma does not have antibodies against A antigen. Can blood group B be given? Yes—no antibodies against B anti-gen are present. What about O group? Yes—O group has no antigens. Because individuals with AB group can be given any type of blood, these persons are called universal recipients. However, because persons withgroup O cannot tolerate (or is incompatible with) any type of blood other than O (but can donate to individ-uals of any blood type), these persons are called uni-versal donors. This is the basis of blood transfusion.
Cross Matching
Before blood is transfused, tests are performed to see if any agglutination occurs when the plasma of the recipient and red cells of the donor (and vice versa) are mixed. This test, called cross matching, is done even when blood types are known. Because there are more than 500 billion blood group types, with many yet to be discovered, it is important to cross match blood before blood transfusion.
Some questions arise. What if the donor has anti-bodies against the red cells of the recipient? For ex-ample, what about the antibodies present in O group plasma if O group blood is given to a person of A group? Doesn’t the O group blood have antibodies against A and B antigen? Will this not clump red cells of the recipient?
Yes, it can. However, because blood from the donor (about 400 mL [422 qt]) is given to the recipi- ent slowly, the antibodies are diluted in the recipient’s plasma (plasma volume is approximately 3.5l [3.7 qt]) before they can produce any reaction.
Rh Grouping
Rh system is another important blood grouping sys-tem, other than the ABO system discussed above. TheRh factor (or Rhesus factor) was named after therhesus monkey, whose blood was first used to study this system, and it consists of many antigens (e.g., D, C, and E) on the red blood cell membrane. Of these, the D antigen is most important. When a person has the D antigen on the cell membrane she or he is said to be Rh-positive (Rh ). If no D antigen is present, the individual is said to be Rh-negative (Rh-). Unlike the ABO system in which antibodies are present against the antigens that are not present of the red cells, an Rh-negative individual does not have anti-bodies in the plasma against the Rh antigen. How-ever, if those individuals are exposed to the Rh anti-gen, antibodies are eventually developed.
Importance of Rh Grouping
The Rh system gains importance in an Rh-negative mother if the father happens to be Rh positive. When the mother is pregnant with an Rh-positive fetus, small amounts of Rh-positive blood from the fetus may leak into the maternal circulation. This tends to happen es-pecially at the time of delivery. If the mother is exposed to Rh-positive blood cells, she develops antibodies against the Rh antigen. Usually, the first fetus is not harmed by antigen-antibody reaction because the leak-age tends to occur at the time of delivery and not many antibodies are developed by the mother.
If the mother becomes pregnant again with an Rh-positive fetus, the antibodies that she has already de-veloped can enter the fetal circulation and cause ag-glutination and hemolysis of fetal blood cells. This is called hemolytic disease of the newborn or eryth-roblastosis fetalis. If the reaction is severe, the fetuscan die in the uterus; if less severe, the fetus can de-velop anemia, jaundice, or edema. Because the breakdown product of hemoglobin—bilirubin—can enter the fetal brain, neurologic problems can de-velop. (In an adult, barriers developed in the blood capillaries of the brain do not allow bilirubin to enter brain tissue).
Fortunately, injecting anti-Rh antibodies into the Rh-negative mother soon after delivery can prevent development of antibodies. These anti-Rh antibodies recognize Rh antigens if they enter the mother’s circulation and destroy them before they can stimulate the mother’s immune system.
One might wonder how this has any direct bearing on massage therapy. The basis of blood typing is an apt example of the basic concepts of immunity and how immunity is developed in an individual. The immune mechanisms involved in fighting off infection, recognizing foreign cells (as in transplantation), and benefits of immunization follow the same principles.
Related Topics