Chapter: Medical Surgical Nursing: Assessment and Management of Patients With Eye and Vision Disorders
Orbital Trauma
Orbital and Ocular Trauma
Whether
affecting the eye or the orbit, trauma to the eye and surrounding structures
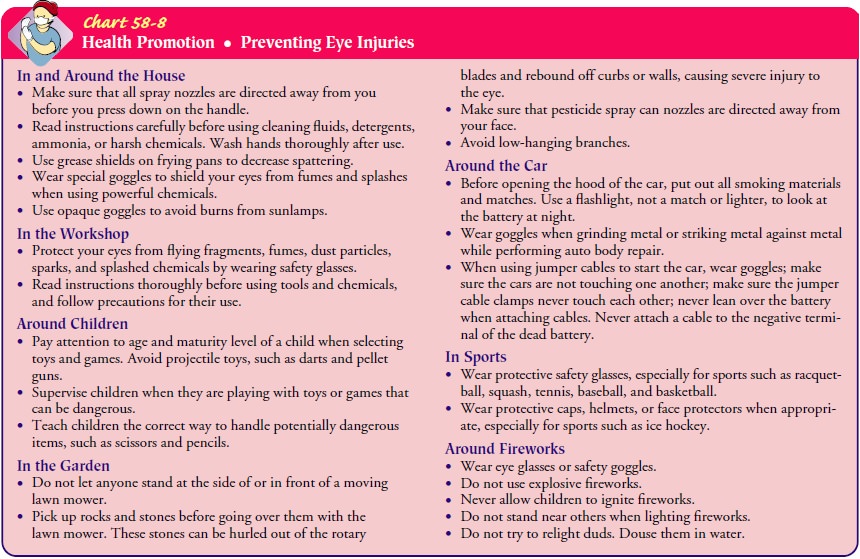
may have devastating consequences for vision.It is preferable to prevent injury
rather than treat it. Chart 58-8details safety measures to prevent orbital and
ocular trauma
ORBITAL TRAUMA
Injury
to the orbit is usually associated with a head injury; hence,the patient’s
general medical condition must first be stabilized before conducting an ocular
examination. Only then is the globeassessed for soft tissue injury. During
inspection, the face ismeticulously assessed for underlying fractures, which
should always be suspected in cases of blunt trauma. To establish the extent of
ocular injury, visual acuity is assessed as soon as possible, even if it is
only a rough estimate. Soft tissue orbital injuries often result in damage to
the optic nerve. Major ocular injuries indicated by a soft globe, prolapsing
tissue, ruptured globe, hemorrhage, and loss of red reflex require immediate
surgical attention.
Soft Tissue Injury and Hemorrhage
The signs and symptoms of soft tissue injury from
blunt or pene-trating trauma include tenderness, ecchymosis, lid swelling, prop-tosis (ie, downward displacement
of the eyeball), and hemorrhage.Closed injuries lead to contusions with
subconjunctival hemor-rhage, commonly known as a black eye. Blood accumulates in the tissues of the conjunctiva.
Hemorrhage may be caused by a soft tissue injury to the eyelid or by an
underlying fracture.
Management
of soft tissue hemorrhage that does not threaten vision is usually conservative
and consists of thorough inspection, cleansing, and repair of wounds. Cold
compresses are used in the early phase, followed by warm compresses. Hematomas
that ap-pear as swollen, fluctuating areas may be surgically drained or
as-pirated; if they are causing significant orbital pressure, they may be
surgically evacuated.
Penetrating
injuries or severe blow to the head can result in se-vere optic nerve damage.
Visual loss can be sudden or delayed and progressive. Immediate loss of vision
after an ocular injury is usu-ally irreversible. Delayed visual loss has a
better prognosis. Cortico-steroid therapy is indicated to reduce optic nerve
swelling. Surgery, such as optic nerve decompression, may be performed.
Orbital Fractures
Orbital fractures are detected by facial x-rays. Depending on the orbital structures involved, orbital fractures can be classified as blow-out, zygomatic or tripod, maxillary, midfacial, orbital apex, and orbital roof fractures. Blow-out fractures result from com-pression of soft tissue and sudden increase in orbital pressure when the force is transmitted to the orbital floor, the area of least resistance.
The
inferior rectus and inferior oblique muscles, with their fat and fascial
attachments, or the nerve that courses along the infe-rior oblique muscle may
become entrapped, and the globe may be displaced inward (ie, enophthalmos).
Computed tomography (CT) can firmly identify the muscle and its auxiliary
structures that are entrapped. These fractures are usually caused by blunt
small objects, such as a fist, knee, elbow, or tennis or golf balls.
Orbital
roof fractures are dangerous because of potential com-plications to the brain.
Surgical management of these fractures requires a neurosurgeon and an
ophthalmologist. The most com-mon indications for surgical intervention are
displacement of bone fragments disfiguring the normal facial contours,
interfer-ence with normal binocular vision caused by extraocular muscle
entrapment, interference with mastication in zygomatic fracture, and
obstruction of the nasolacrimal duct. Surgery is usually non-emergent, and a
period of 10 to 14 days gives the ophthalmolo-gist time to assess ocular
function, especially the extraocular muscles and the nasolacrimal duct.
Emergency surgical repair is usually not performed unless the globe is
displaced to the maxil-lary sinus. Operative repair is primarily directed at
freeing the en-trapped ocular structures and restoring the integrity of the
orbital floor. Cosmetic surgery for deformities of the globe and enoph-thalmos
may follow after 4 to 6 months, but successful repair is usually difficult.
Foreign Bodies
Foreign
bodies that enter the orbit are usually tolerated, except for copper, iron, and
vegetable materials such as those from plants or trees, which may cause
purulent infection. X-rays andCT scans are used to identify the foreign body.
Careful history taking is important, especially if the foreign body has been in
the orbit for a period of time and the incident forgotten. It is im-portant to
identify metallic foreign bodies because they prohibit the use of magnetic
resonance imaging (MRI) as a diagnostic tool.
After
the extent of the orbital damage is assessed, the decision is made between
conservative treatment and surgical removal. In general, orbital foreign bodies
are usually removed if they are su-perficial and anterior in location, have
sharp edges that may af-fect adjacent orbital structures, or are composed of
copper, iron, or vegetable material. The surgical intervention is directed at
pre-vention of further ocular injury and maintaining the integrity of the
affected areas. Cultures are usually obtained, and the patient is placed on
prophylactic intravenous antibiotics that are later changed to oral
antibiotics.
Related Topics