Chapter: Medical Surgical Nursing: Assessment and Management of Patients With Eye and Vision Disorders
Macular Degeneration - Retinal Disorders
MACULAR DEGENERATION
Macular
degeneration is the most common cause of visual loss in people older than age
60 (Margolis et al., 2002). Commonly called age-related macular degeneration
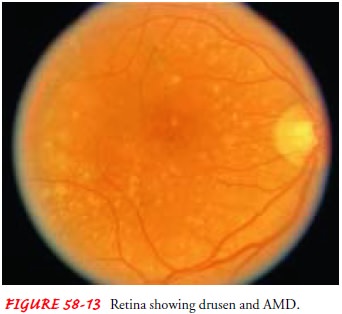
(AMD), it is character-ized by tiny, yellowish spots called drusen (Fig. 58-13)
beneath the retina. Most people older than 60 years of age have at least a few
small drusen. There is a wide range of visual loss in patients with macular
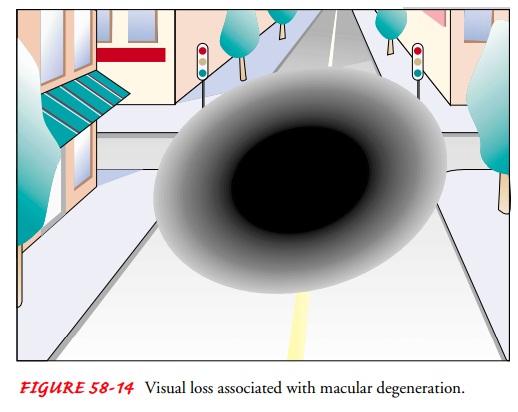
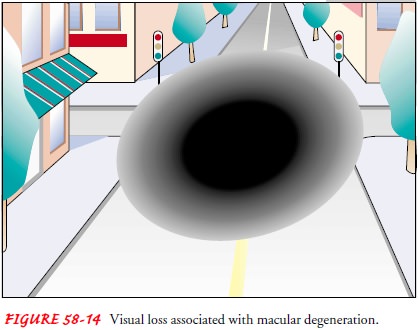
degeneration, but most patients do not experience total blindness. Central
vision is generally the most affected, with most patients retaining peripheral
vision (Fig. 58-14). There are two types of AMD, commonly known as the dry type
and wet type.
Between
85% and 90% of people with AMD have the dry or nonexudative type in which the
outer layers of the retina slowly break down (Fig. 58-15). With this breakdown
comes the ap-pearance of drusen. When the drusen occur outside of the mac-ular
area, patients generally have no symptoms. When the drusen occur within the
macula, there is a gradual blurring of vision that patients may notice when
they try to read. There is no known treatment that can slow or cure this type
of AMD.
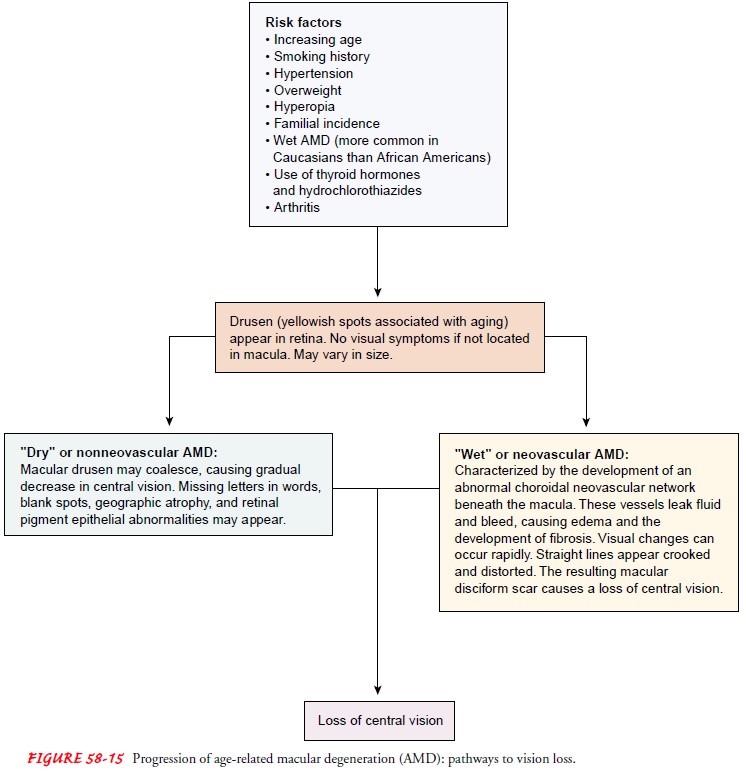
The second type of AMD, the wet or exudative type, may have an abrupt onset. Patients complain that straight lines appear crooked and distorted or that letters in words appear broken up. This effect results from proliferation of abnormal blood vessels growing under the retina, within the choroid layer of the eye, a condition known as choroidal neovascularization (CNV). The affected vessels can leak fluid and blood, elevating the retina. Some patients can be treated with the laser to stop the leakage from these vessels. This treatment is not ideal because vision may be affected by the laser treatment and abnormal vessels often grow back after treatment.
Medical Management
PHOTODYNAMIC THERAPY
Visual
loss from CNV lesions in AMD is a growing problem. With the growth of these new
vessels from the choriocapillar layer, fibrous tissue develops that can, over
months, destroy cen-tral vision. Laser treatment has been used to close these
abnor-mal vessels, but the very process of photocoagulation carries with it
some level of retinal destruction, albeit less than the natural scarring that
would occur in the untreated eye. Photodynamic therapy (PDT) has been developed
in an attempt to ameliorate the CNV while causing minimal damage to the retina.
The Treatment of Age-Related Macular Degeneration With Photo-dynamic Therapy
(TAP) study group (1999) has shown that PDT can reduce the risk of visual loss
for certain groups of pa-tients who have classic subfoveal choroidal
neovascularization due to macular degeneration.
PDT
is a two-step process (Fig. 58-16). Verteporfin, a photo-sensitive dye, is
infused intravenously over 10 minutes. Fifteen minutes after the start of the
infusion, a diode laser is used to treat the abnormal network of vessels. The
dye within the vessels takes up the energy of the diode laser, but the
surrounding retina does not, avoiding damage to adjacent areas. Retreatment may
be nec-essary over time.
Nursing Management
Nursing management is primarily educational. Verteporfin is a light-activated dye, and patient education is important preoperatively. The patient should be instructed to bring dark sunglasses, gloves, a wide-brimmed hat, long-sleeved shirt, and slacks to the PDT setting. The patient must be cautioned to avoid exposure to direct sunlight or bright light for 5 days after treatment. The dye within the blood vessels near the surface of the skin could become activated with exposure to strong light. This would include bright sunlight, tanning booths, halogen lights, and the bright lights used in dental offices and operating rooms. Ordinary indoor light is not a problem. If a patient must go outdoors within the first 5 days after treatment, he or she should be counseled to wear long-sleeved shirts and slacks made of tightly woven fabrics.
Gloves, shoes, socks,
sunglasses, and a wide-brimmed hat should also be worn if the patient has to go
outdoors during daylight hours during this period. Inadvertent sunlight
exposure can lead to severe blistering of the skin and sunburn that may require
plas-tic surgery.
Macular Translocation
Wet
macular degeneration is characterized by the development of an abnormal CNV
membrane to the detriment of central vi-sion. One approach to this problem is
the surgical procedure known as macular translocation, in which a 360-degree
retinal detachment is surgically created and the retina is gently lifted and
resettled, placing the macular area a slight distance away from thearea of CNV.
Laser treatment can then be applied to the abnor-mal neovascular network with
minimal damage occurring to the macula. Pilot studies are evaluating whether
this surgical ap-proach is an effective alternative to laser treatments of CNV
due to AMD.
Angiogenesis
An important component of the effort against neovascular AMD is the investigation into the causes of the development and pro-gression of angiogenesis (ie, abnormal blood vessel formation). Investigations continue in the laboratory to search for agents that can inhibit angiogenesis. This has implications for ocular neovascularization and treatment of other disorders such as solid tumors.
Management
Most
patients benefit from the use of bright lighting and magni-fication devices and
from referral to a low-vision center. Some low-vision centers send
representatives into the patient’s home or place of employment to evaluate the
living and working condi-tions and make recommendations to improve lighting,
thereby improving vision and promoting safety. The home care nurse can make the
same assessment and recommendations.
Amsler
grids are given to patients to use in their home to mon-itor for a sudden onset
or distortion of vision. These may provide the earliest sign that macular
degeneration is getting worse. Patients should be encouraged to use these grids
and to look at them, one eye at a time, several times each week with glasses
on. If there is a change in the grid (eg, if the lines or squares ap-pear
distorted or faded), the patient should be instructed to no-tify the
ophthalmologist immediately and to arrange to be seen promptly.
The
Age-Related Eye Disease Study Group (2001), a multi-center clinical trial, has
provided promising information about the prevention and treatment of AMD. The
study was designed to determine whether large doses of macronutrients are
effective in preventing or slowing the course of AMD. The study revealedthat
use of antioxidants (ie, vitamin C, vitamin E, and beta-carotene) and minerals
(ie, zinc oxide) can slow the progression of AMD and vision loss for people at
high risk for developing advanced AMD.
Related Topics