Chapter: Clinical Anesthesiology: Regional Anesthesia & Pain Management: Chronic Pain Management
Differential Neural Blockade
Differential
Neural Blockade
Pharmacological or anatomic differential
neural blockade has been advocated as a method of dis-tinguishing somatic,
sympathetic, and psychogenic pain mechanisms. The procedure is controversial
owing to the challenges of interpreting the data and the inability to define
exactly which nerve fibers or pathways are blocked. Theoretically, the
pharmaco-logical approach relies on the differential sensitivity of nerve
fibers to local anesthetics. Preganglionic sympathetic (B) fibers are reported
to be most sen-sitive, closely followed by pain (Aδ) fibers, somato-sensory (Aβ) fibers, motor fibers (Aα), and finally C fibers. By using different concentrations of local
anesthetic, it may be possible to selectively block certain types of fibers
while preserving the func-tion of others. The challenge is that the critical
con-centration needed to block sympathetic fibers can vary considerably between
patients, and conduction block by local anesthetics is dependent not only on
fiber size but also on the duration of contact and fre-quency of impulses
conducted. Many clinicians have therefore abandoned the use of pharmacological
dif-ferential neural blocks in favor of anatomic differen-tial blockade.
Stellate ganglion blocks can be used to
selec-tively block sympathetic fibers to the head, neck, and arm. Celiac
plexus, hypogastric plexus, and lumbar paravertebral sympathetic blocks can be
used for sympathetic blocks of the abdomen, pelvis, and leg, respectively.
Selective nerve root, intercostal, cervi-cal plexus, brachial plexus, or
lumbosacral plexus blocks may be used for somatic nerve blockade.
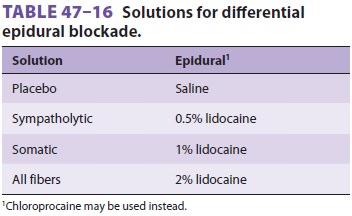
Differential epidural blocks may be used for thoracic pain when the
techniques for sympathetic blockade carry a significant risk of pneumothorax (Table
47–16). After each epidural injection, the patient is evaluated for pain
relief, signs of sym-pathetic blockade (a decrease in blood pressure),
sensation to pinprick and light touch, and motor function. If the pain
disappears after the saline injection, the patient either has psychogenic pain
(usually a profound long-lasting effect) or is dis-playing a placebo effect
(usually short lasting). If pain relief coincides with isolated signs of
sympa-thetic blockade, it is likely mediated by sympathetic fibers. If pain
relief only follows somatosensory blockade, it is likely mediated by somatic
fibers. Lastly, if the pain persists even after signs of motor blockade, the
pain is either central (supraspinal) or psychogenic.
The differential epidural block carries the risk of any neuraxial block,
and the possibility of hypo-tension and blocking cardiac accelerator fibers at
T1–T4. The level should not extend above the T5 dermatome due to these risks.
Following catheter insertion, injections should be administered with the
patient in a monitored setting for the rest of this procedure.
Although differential epidural blockade has limitations, it may be
helpful to identify primarily centralized pain when a patient continues to have
a significant level of pain despite multilevel dermato-mal blockade over the
painful region. It is unlikely that a subsequent nerve block would help to
treat the painful condition.
When it is thought that a
patient may have abdominal pain from the anterior abdominal
wall, a transversus abdominis plane (TAP) block may be performed using
ultrasound guidance. This may offer potential short- or long-term relief and
can be considered as an alternative to differential epidural blockade. If no
relief is obtained, the pain may have a visceral origin or a central cause.
Visceral pain may best respond to a celiac or splanchnic nerve block and possibly
to subsequent splanchnic RFA. Patients with pain that is primarily of a central
origin may respond to multidisciplinary therapy, including counseling and
biofeedback training.
Related Topics