Chapter: Biology of Disease: Disorders of the Endocrine System
Diagnosis and treatment of diabetes mellitus
Diagnosis and treatment of diabetes mellitus
Investigation of diabetes is made on the basis of clinical features and laboratory investigations. A preliminary screening test may identify the presence of urinary glucose, although this is not diagnostic of diabetes mellitus. A patient presenting with symptoms of diabetes mellitus must have a venous blood specimen taken and its glucose concentration determined. A patient is diagnosed as diabetic if the fasting plasma glucose concentration is equal to or greater than 7.0 or the random concentration is greater than 11.1 mmol dm–3. Diabetes mellitus is excluded if the fasting or random plasma glucose concentrations are less than 6.1 or 7.8 mmol dm–3 respectively. If the individual under investigation lacks the typical symptoms of diabetes then diagnosis cannot be confirmed by a single glucose determination but reconfirmed by at least one additional positive test on another day or investigated using the oral glucose tolerance test (OGTT). During the OGTT, the patient is kept on a normal diet for three days prior to the test and then fasts overnight prior to the test. A basal (fasting) venous blood sample is taken for glucose determination before the patient drinks 75 g of anhydrous glucose dissolved in a small volume of water. Blood specimens are collected after one and two hours and plasma glucose determined. Plasma glucose values greater than or equal to 7.0 mmol dm–3 for the basal sample or 11.1 mmol dm–3 for the 2 h samples are diagnostic of diabetes mellitus. Individuals with plasma glucose concentrations less than 7.0 for the basal sample or between 7.8 and 11.1 mmol dm–3 for the 2h samples are categorized as having impaired glucose tolerance (IGT). This group has an increased risk of developing cardiovascular disease . Patients with plasma glucose concentrations of 6.1 to 7.0 mmol dm–3 for the basal samples or less than 7.8 mmol dm–3 for the 2 h samples are categorized as having impaired fasting glucose (IFG) and are at risk of developing diabetes. The values given relate to venous plasma samples and are different from those for whole blood samples.
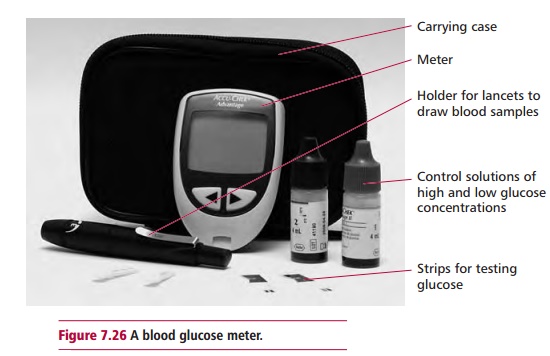
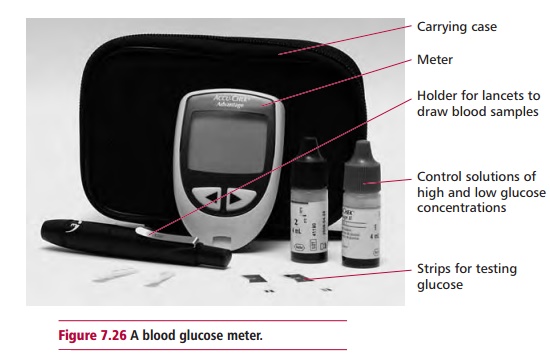
The management of diabetes mellitus aims to provide relief from symptoms and reduce the chances of developing acute and chronic complications. This includes educating the patient that diabetes is a life-long disease and affected individuals must be responsible for their own treatment. Regular clinical and laboratory assessment of the patient is required to ensure that treatment is effective, to detect early signs of treatable complications so as to reduce their progression and ensure compliance with treatment. Management involves the dietary restriction of simple sugars and of saturated fats and cholesterol and the use of complex carbohydrate and fibers. Dietary control is often accompanied by use of injected insulin or oral hypoglycemic drugs, such as sulfonylureas, in patients with type 1 and type 2 diabetes respectively. Occasionally, it may be necessary to use insulin in patients with type 2 diabetes to control blood glucose effectively. Hypoglycemic drugs act by increasing the sensitivity of A cells to glucose therefore stimulating insulin release or by increasing sensitivity of target cells to insulin. Both effects will reduce blood glucose levels. Some hypoglycemic drugs act to reduce the absorption of glucose by the GIT or reduce glycogenolysis in the liver. Diabetic patients on treatment are monitored regularly to ensure that blood glucose is kept in control. Most patients measure their own blood glucose at home regularly using kit methods based on reagent strips and a portable glucose meter (Figure 7.26) and adjust insulin dosage according to needs, perhaps following a change in diet, during illness or after exercise. The amount of glycated hemoglobin (Figure 1.14) in a patient is determined regularly to assess therapy compliance because its presence is an indicator of average glycemia over the previous 6–8 weeks. The amount of glycated hemoglobin tends to be less than 6% in nondiabetics but may exceed 10% in uncontrolled diabetes. Diabetic patients with high values have poor blood glucose control and their treatment or compliance must be reviewed.
Related Topics