Chapter: Medical Surgical Nursing: Assessment and Management of Patients With Hepatic Disorders
Assessment of Patients With Hepatic Disorders
Assessment
HEALTH HISTORY
If
liver function test results are abnormal, the patient may need to be evaluated
for liver disease. In such cases, the health history will focus on exposure of
the patient to hepatotoxic substances or in-fectious agents. The patient’s
occupational, recreational, and travel history may assist in identifying
exposure to hepatotoxins (eg, in-dustrial chemicals, other toxins) responsible
for illness. The pa-tient’s history of alcohol and drug use, including but not
limited to the use of injectable drugs, provides additional information about
exposure to toxins and infectious agents. Many medications (including
acetaminophen, ketoconazole, and valproic acid) are responsible for hepatic
dysfunction and disease. A careful med-ication history to assess hepatic
dysfunction should address all pre-scribed and over-the counter medications,
herbal remedies, and dietary supplements used by the patient currently and in
the past.
Lifestyle
behaviors that increase the risk for exposure to infec-tious agents are
identified. Injectable drug use, sexual practices, and a history of foreign
travel are all potential risk factors for liver disease. The amount and type of
alcohol consumption are iden-tified using screening tools (questionnaires) that
have been de-veloped for this purpose.
The
history also includes an evaluation of the patient’s past medical history to
identify risk factors for the development of liver disease. Current and past
medical conditions, including those of a psychological or psychiatric nature,
are identified. The family history includes questions about familial liver
disorders that may have their etiology in alcohol abuse or gallstone disease,
as well as other familial or genetic diseases, such as hemochro-matosis,
Wilson’s disease, or alpha-1 antitrypsin disease.
The
history also includes reviewing symptoms that suggest liver disease. Symptoms
that may have their etiology in liver disease but are not specific to hepatic
dysfunction include jaundice, malaise, weakness, fatigue, pruritus, abdominal
pain, fever, anorexia,weight gain, edema, increasing abdominal girth,
hematemesis, melena, hematochezia (passage of bloody stools), easy bruising,
decreased libido in men and secondary amenorrhea in women, changes in mental
acuity, personality changes, and sleep distur-bances.
PHYSICAL EXAMINATION
The
nurse assesses the patient for physical signs that may occur with liver
dysfunction, including pallor of chronic illness and jaundice. The skin,
mucosa, and sclerae are inspected for jaun-dice, and the extremities are
assessed for muscle atrophy, edema, and skin excoriation secondary to
scratching. The nurse observes the skin for petechiae or ecchymotic areas
(bruises), spider an-giomas, and palmar erythema. The male patient is assessed
for unilateral or bilateral gynecomastia and testicular atrophy due to
endocrine changes. The patient’s cognitive status (recall, mem-ory, abstract
thinking) and neurologic status are assessed. The nurse observes for general tremor,
asterixis, weakness, and slurred speech. These symptoms are discussed later.
The
nurse assesses the abdomen for dilated abdominal wall veins, ascites, and a
fluid wave (discussed later). The abdomen is palpated to assess liver size and
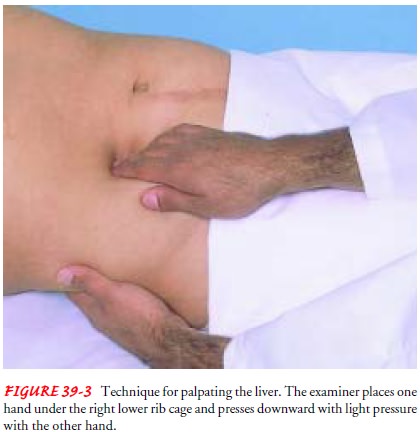
to detect any tenderness over the liver. The liver may be palpable in the right
upper quadrant. A palpable liver presents as a firm, sharp ridge with a smooth
sur-face (Fig. 39-3). The nurse estimates liver size by percussing its upper
and lower borders. When the liver is not palpable but ten-derness is suspected,
tapping the lower right thorax briskly may elicit tenderness. For comparison,
the nurse then performs a sim-ilar maneuver on the left lower thorax.
If the
liver is palpable, the examiner notes and records its size and consistency,
whether it is tender, and whether its outline is regular or irregular. If the
liver is enlarged, the degree to which it descends below the right costal
margin is recorded to provide some indication of its size. The examiner determines
whether the liver’s edge is sharp and smooth or blunt, and whether the
en-larged liver is nodular or smooth. The liver of a patient with cirrhosis is
small and hard, whereas the liver of a patient with acute hepatitis is soft,
and the hand easily moves the edge.
Tenderness
of the liver implies recent acute enlargement with consequent stretching of the
liver capsule. The absence of ten-derness may imply that the enlargement is of
long-standing du-ration. The liver of a patient with viral hepatitis is tender,
whereas that of a patient with alcoholic hepatitis is not. Enlargement of the
liver is an abnormal finding requiring evaluation.
Related Topics