Chapter: Microbiology
Adaptive Imuunity
ADAPTIVE IMMUNITY
Introduction
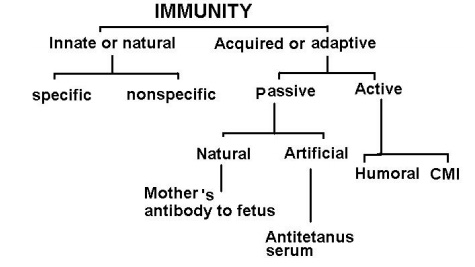
Immunity is the resistance shown by the host towards injury caused by microorganisms and their products. Immunity can be classi-fied into two types. They are innate or natural immunity and acquired or adaptive immunity
Innate immunity is the resistance to infections which individuals possess due to their genetic make up. Innate immunity is again divided into two types. They are specific and non specific.
Acquired or adaptive immunity which occurs after exposure to an infectious agent is specific and is mediated by either antibodies or lymphoid cells. It can be passive or active.
Passive immunity
Passive immunity is transmitted by antibodies preformed in another host. It is of two types. They are natural passive and artificial passive immunity. In natural passive immunity the antibodies which are formed in mother are transferred to foetus. They give protection to the new born babies for three months. In artificial passive immunity the preformed antibodies are administered to the persons. For example anti tetanus serum is used as passive immunization against tetanus. It provides immediate and temporary protection.
Active immunity
It is produced directly by the immune system of the host. Also it is induced by contact with antigen and give long lasting protection. The immune response is of two types. They are humoral immunity and cell mediated immunity.
Adaptive or acquired immunity forms the host’s second line of defense. When microorganisms overcome or circumvent the innate, nonspecific defense mechanism or deliberately administered as vaccines, they en-counter the adaptive immunity
DEFINITION
Adaptive (acquired) immunity, refers to antigen-specific defense mechanisms that take several days to become protec-tive and are designed to remove a specific antigen.
This is the immunity one develops throughout life. Six major characteristics of acquired immunity are:
1. Specificity : It shows exquisite specificity for distinct moleculesagainst which it is induced and does not recognize other molecules
2. Self-non self discrimination or tolerance: It can discriminate selfantigens belonging to the individual’s own body and are made tol-erant to these self antigens. Under very rare circumstances they react to the self antigens body and are made tolerant to these self antigens.
3. Inducible
Adaptive immune response can be induced artificially.
4. Diversity
Different types of microbes induce responses in different ways so that diverse responses are generated
5. Memory
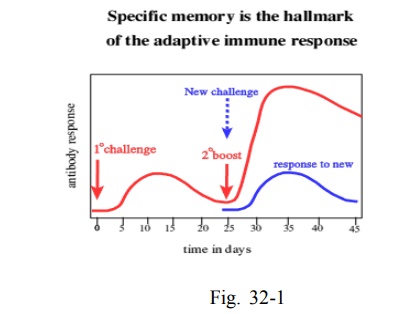
Adaptive immune response has the ability to remember and respond more vigorously to repeated exposure to the same microbe.
6. Self-limiting
Adaptive immunity usually improves upon repeated exposure to a given infection.
Adaptive immunity involves the following:
(1) antigen-presenting cells (APCs) such as macrophages and den-dritic cells; (2)the activation and proliferation of antigen-specific B-lymphocytes; (3) the activation and proliferation of antigen-specific T-lymphocytes; (4) and the production of antibody molecules, cytotoxic T-lymphocytes (CTLs), activated macrophages and NK cells, and cytokines. There are two major branches of the adaptive immune re-sponses: humoral immunity and cell-mediated immunity.
Humoral immunity: Humoral immunity involves the production of an-tibody molecules in response to an antigen and is mediated by B-lymphocytes.
Cell-mediated immunity: Cell-mediated immunity involves the pro-duction of cytotoxic T-lymphocytes, activated macrophages, activated NK cells, and cytokines in response to an antigen.
The humoral immune system
B cells develop in bone marrow. These B cells have membrane bound antibody as a receptor for antigen. Each B cell makes one kind of antibody. B cells differentiate into plasma cells, which produce large amounts of soluble antibody.
The cellular immune system
Helper T cells mature in the thymus and contain a single T cell receptor for antigen. Helper T cell activation requires recognition of antigen and a co-stimulatory signal from the innate immune system. Helper T cells contain a surface protein called CD4 and must be acti-vated by the antigen presenting dendritic cells of the innate immune system.
Fate of Antigens
Antigens are of two types namely complete antigens and incom-plete antigens. Complete antigens are substances when introduced into the body induce an immune response. Incomplete antigens do not in-duce immune response but they react with preformed antibodies and are called haptens
The mechanisms by which the complete antigens are destroyed depend on factors such as: 1)Physical nature of antigens 2) chemical nature of antigen 3) Dose of antigen 4) Route of entry 5) and antigen presentation.
Physical nature of antigen
Particulate antigens are removed from the circulation by two phases, one by a non immune phase and another by immune phase. In the non immune phase antigen is removed by phagocytic cells and in the immune phase antigen-antibody complexes are formed.
With soluble antigens three phases are seen. In the phase of equi-librium, the antigen is diffused into extravascular spaces. In the meta-bolic phase the antigen level falls down due to catabolic decay and during immune elimination the antigen is eliminated by antigen antibody reactions
Chemical nature of antigen
Protein antigens are eliminated with in weeks. Polysaccharide antigens are eliminated slowly. It takes several months to destroy them.
Dose of antigen
Macrophages modulate the dose of antigens so that they are not too low or too high.
Route of entry
Antigens introduced intravenously are localized in spleen, liver bone marrow, kidneys and lungs and are killed by reticuloendothelial cells mainly tissue macrophages.
Antigens introduced subcutaneously are localized in lymph nodes
Presentation of antigen
Presentation of antigens to the immunocompetent cells is carried out by macrophages and dendritic cells.
Adjuvants
Adjuvants are substances which enhance the immune responses. Immunocompetent B lymphocytes recognize antigens and produce antibodies. For this recognition it requires T cell help. Once B cell contacts its specific antigen, it undergoes clonal proliferation and is converted into plasma cells and secretes antibody.

Related Topics