Chapter: Ophthalmology: Retina
Retinal Vasculitis - Retinal Inflammatory Disease
Retinal Inflammatory Disease
Retinal Vasculitis
Definition
Retinal vasculitis is an inflammation of the
retinal vasculature. Typical findings include cells in the vitreous body.
Epidemiology:
Retinal vasculitis is one of the more frequent clinical
syn-dromes.
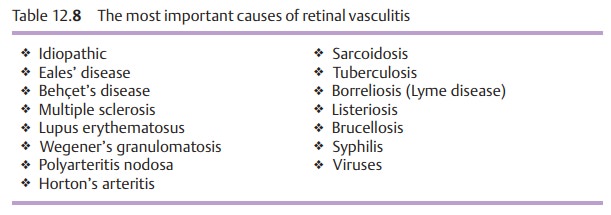
Etiology:
The cause of retinal vasculitis often remains obscure. It can becaused by a pathogen or occur in association with immunologic processes (Table 12.8).
Symptoms:
Patients report loss of visual acuity or black dots in their visualfield. These are due to the presence of cells in the vitreous body.
Diagnostic considerations:
The ophthalmologic diagnostic work-upincludes clinical
examination, ophthalmoscopy, and slit-lamp examination. The slit-lamp
examination will reveal cells in the
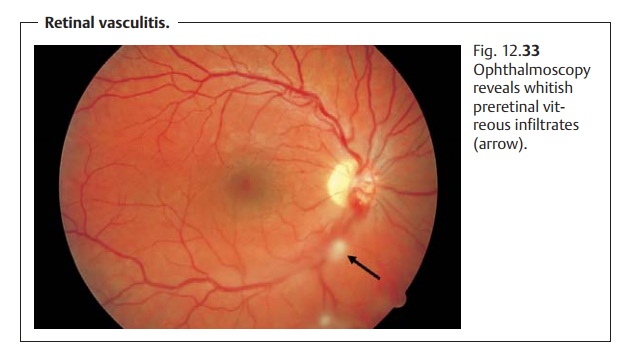
vitreous body. Ophthalmo-scopic findings will include whitish preretinal
infiltrates (Fig. 12.33), vascular
constriction (usually involving the veins), vascular occlusion, intraretinal bleeding,
and retinal edema. Fluorescein angiography may be used to eval-uate the
presence and activity of neovascularization. Underlying systemic disease,
immunologic processes, and infections (see Table 12.8) must be excluded.

Differential diagnosis:
Other vascular diseases of the retina such as veinocclusion should be excluded. These vascular diseases may be distinguished from vascular retinitis by the absence of cells in the vitreous body.
Treatment:
The causes of known underlying disorders should be
treated.Symptoms are treated with topical steroids and systemic steroids in the
absence of contraindications. Neovascularization is treated with laser
ther-apy.
Prophylaxis:
No prophylaxis is possible except for possible treatment of
anunderlying disorder.
Clinical course and prognosis:
Vascular occlusion can result in neovasculari-zation that may
lead to vitreous hemorrhage. Tractional retinal detachment is another possible
complication.
Related Topics