Chapter: Ophthalmology: Retina
AIDS-Related Retinal Disorders - Retinal Inflammatory Disease
AIDS-Related Retinal Disorders
Definition
Retinal disorders in AIDS involve either
AIDS-associated microangiopathy or infection.
Epidemiology:
Up to 80% of all AIDS patients have retinal disorders as aresult
of the disease. Other ocular involvement is rare.
Pathogenesis:
The pathogenesis of microangiopathy is still unclear.
Oppor-tunistic infections are frequently caused by viruses.
Symptoms:
Microangiopathy is usually asymptomatic. Patients with
infec-tious retinal disorders report loss of visual acuity and visual field
defects.
Diagnostic considerations:
Ophthalmoscopic findings inAIDS-associatedmicroangiopathy include hemorrhages, microaneurysms, telangiectasia,and cotton-wool spots. Direct involvement of vascular endothelial cells in HIV infection or immune-complex-mediated damage to endothelial cells and vascular structures is thought to play a role.
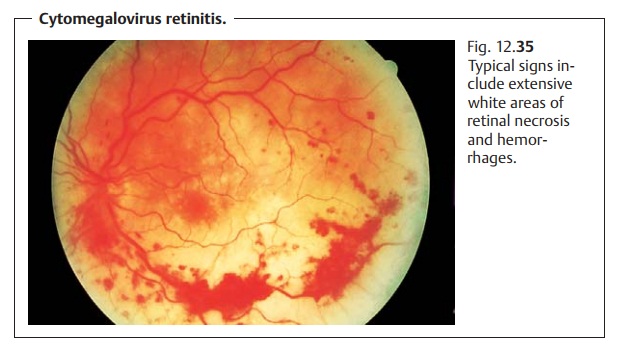
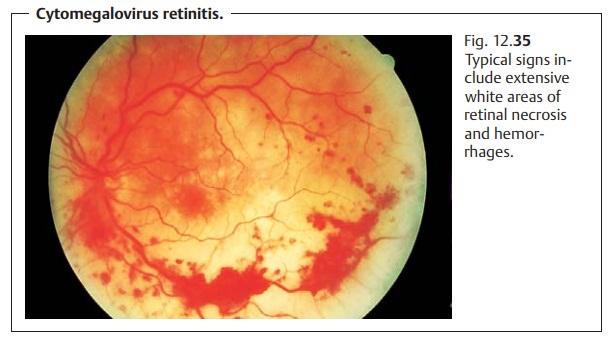
Cytomegalovirus retinitis occurs in 20 – 40% of older patients. Peripheralretinal necrosis
and intraretinal bleeding (Fig. 12.35)
are frequently observed. Vascular occlusion is rare. Secondary rhegmatogenous
retinal detachment may develop. These lesions heal to produce fine granular
pigment epithelial scars.
Less frequently, AIDS may involve retinal infection caused by herpes sim-plex and varicella-zoster
viruses, Toxoplasma gondii, or Pneumocystis carinii. The diagnosis of
a viral retinal infection in AIDS is confirmed byattempting to obtain positive
serum cultures and by resistance testing.
Differential diagnosis:
Inflammatory retinal changes due to other causesshould be
excluded by serologic studies.
Treatment:
Microangiopathy does not require treatment. Viral retinitis
istreated with ganciclovir or foscarnet. Herpes simplex and varicella-zoster
viruses are treated with acyclovir.
Prophylaxis:
Ophthalmologic screening examinations are indicated in
thepresence of known viral infection.
Clinical course and prognosis:
The prognosis for microangiopathy is verygood. Infectious
retinitis will lead to blindness if left untreated. Visual acuity can often be
preserved if a prompt diagnosis is made.
Related Topics