Chapter: Clinical Dermatology: Infections
Candidiasis - Fungal infections
Candidiasis
Cause
Candida
albicans is a classic opportunistic pathogen.Even in transient and
trivial local infections in the apparently fit, one or more predisposing
factors such as obesity, moisture and maceration, diabetes, pregnancy, the use
of broad-spectrum antibiotics, or perhaps the use of the contraceptive pill,
will often be found to be playing some part. Opportunism is even more obvious
in the overwhelming systemic infec-tions of the immunocompromised (Fig. 14.45).
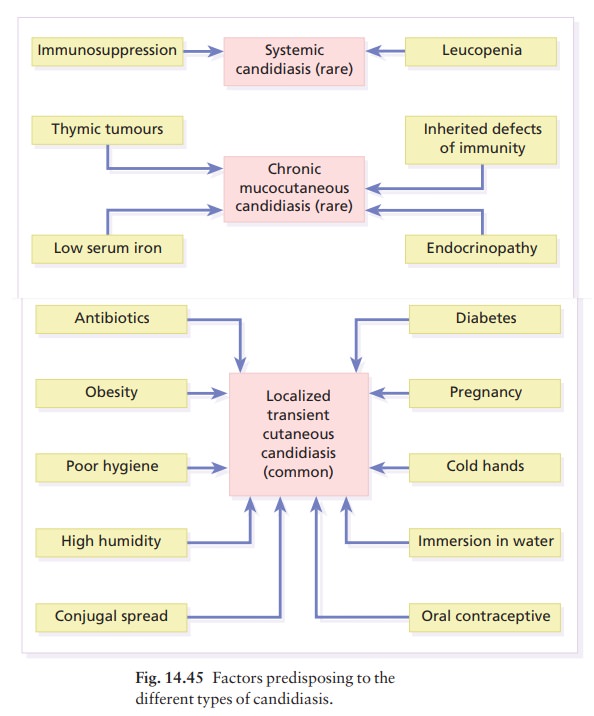
Presentation
This
varies with the site (Fig. 14.46).
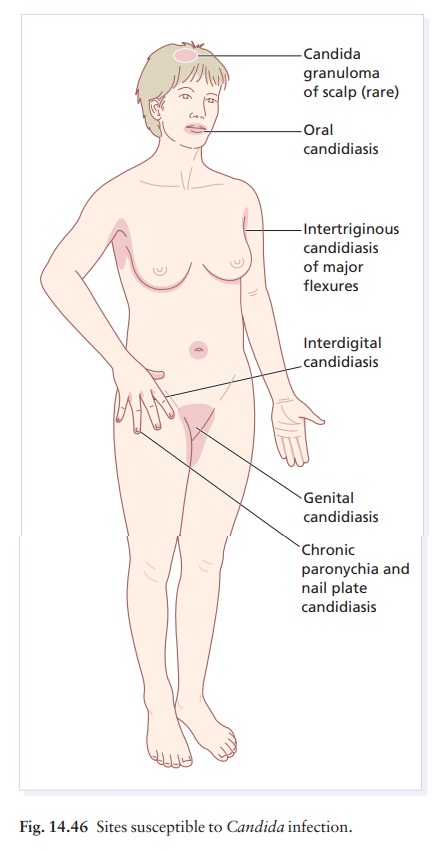
Oral candidiasis
One
or more whitish adherent plaques (like bread sauce) appear on the mucous
membranes. If wiped off they leave an erythematous base. Under dentures,
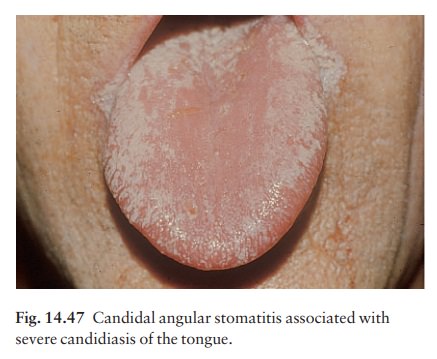
candidiasis will produce sore red areas. Angular stomatitis, usually in denture
wearers (Fig. 14.47), may be candidal.
Candida intertrigo
A moist glazed area of erythema and macera-tion appears in a body fold; the edge shows soggy scaling, and outlying satellite papulopustules. These changes are most common under the breasts, and in the armpits and groin, but can also occur be-tween the fingers of those whose hands are often in water.
Genital candidiasis
Most
commonly presents as a sore itchy vulvovagin-itis, with white curdy plaques
adherent to the inflamed mucous membranes, and a whitish discharge. The
eruption may extend to the groin folds. Conjugal spread is common; in males
similar changes occur under the foreskin (Fig. 14.48) and in the groin.
Diabetes,
pregnancy and antibiotic therapy are common predisposing factors.
Paronychia
Acute
paronychia is usually bacterial, but in chronic paronychia Candida
may be the sole pathogen, or be found with other opportunists such as Proteus
or Pseudomonas.
The proximal and sometimes the lateralnail folds of one or more fingers become
bolstered and red (see Fig. 13.28). The cuticles are lost and small amounts
of pus can be expressed. The adjacent nail plate becomes ridged and
discoloured. Predisposing factors include wet work, poor peripheral circulation
and vulval candidiasis.
Chronic mucocutaneous candidiasis
Persistent candidiasis, affecting most or all of the areas described above, can start in infancy. Some-times the nail plates as well as the nail folds are involved. Candida granulomas may appear on the scalp. Several different forms have been described including those with autosomal recessive and domin-ant inheritance patterns. In the Candida endocrino-pathy syndrome, chronic candidiasis occurs with one or more endocrine defects, the most common of which are hypoparathyroidism, and Addison’s dis-ease. A few late-onset cases have underlying thymic tumours.
Systemic candidiasis
This
is seen against a background of severe illness, leucopenia and immunosuppression.
The skin lesions are firm red nodules, which can be shown by biopsy to contain
yeasts and pseudohyphae.
Investigations
Swabs from suspected areas should be sent for cul-ture. The urine should always be tested for sugar. In chronic mucocutaneous candidiasis, a detailed immunological work-up will be needed, focusing on cell-mediated immunity.
Treatment
Predisposing
factors should be sought and eliminated; e.g. denture hygiene may be important.
Infected skin folds should be separated and kept dry. Those with chronic
paronychia should keep their hands warm and dry.
Amphotericin,
nystatin and the imidazole group of compounds are all effective topically. For
the mouth, these are available as oral suspensions, lozenges and oral gels
(Formulary 1). False teeth should be removed at night, washed and steeped in a
nysta-tin solution. For other areas of candidiasis, creams, ointment and
pessaries are available (Formulary 1). Magenta paint is also a useful but messy
rem-edy for the skin flexures. In chronic paronychia, the nail folds can be
packed with an imidazole cream or drenched in an imidazole solution several
times a day. Genital candidiasis responds well to a single day’s treatment with
either itraconazole and fluconazole (Formulary 2). Both are also valuable for
recurrent oral candidiasis of the immunocomprom-ised, and for the various types
of chronic mucocutan-eous candidiasis.
Related Topics