Chapter: Essentials of Anatomy and Physiology: Nervous System
Spinal Cord and Spinal Cord Reflexes
SPINAL CORD
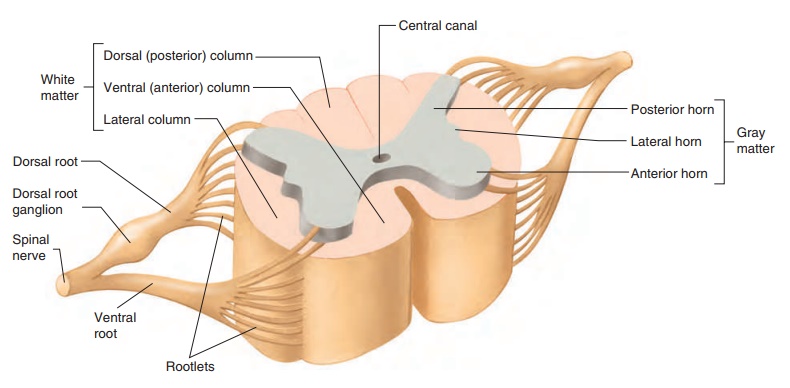
The spinal cord extends from the foramen magnum at the base of the skull to the second lumbar vertebra (figure 8.15). Spinal nerves communicate between the spinal cord and the body. The inferior end of the spinal cord and the spinal nerves exiting there resemble a horse’s tail and are collectively called the caudaequina (kaw′dă, tail;ē-kwı̄′nă, horse).
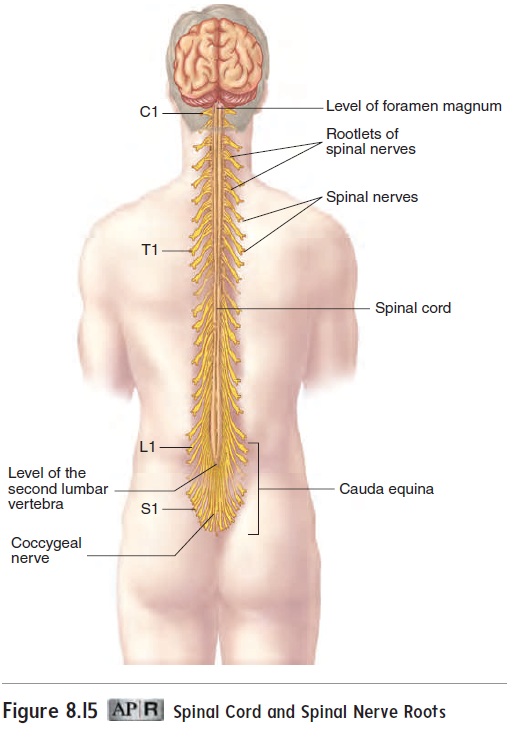
A cross section reveals that the spinal cord consists of a superficial white matter portion and a deep gray matter portion (figure 8.16a). The white matter consists of myelinated axons, and the gray matter is mainly a collection of neuron cell bodies. The white matter in each half of the spinal cord is organized into three columns, called the dorsal (posterior), ventral (anterior), and lateral columns. Each column of the spinal cord contains ascending and descending tracts, or pathways. Ascending tracts consist of axons that conduct action potentials toward the brain, and descending tracts consist of axons that conduct action poten-tials away from the brain. Ascending tracts and descending tracts are discussed more fully in “Sensory Functions” and “Motor Functions” later.
The gray matter of the spinal cord is shaped like the letter H, with posterior horns and anterior horns. Small lateral horns exist in levels of the cord associated with the autonomic nervous system. Thecentral canal is a fluid-filled space in the center of the cord.
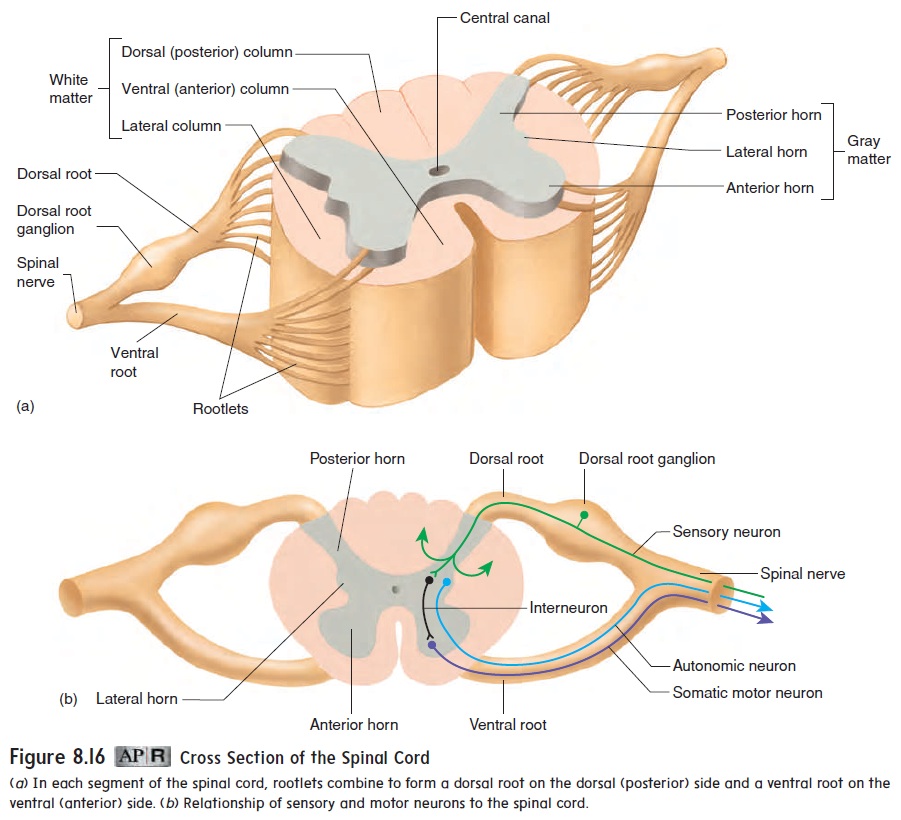
Spinal nerves arise from numerous rootlets along the dorsal and ventral surfaces of the spinal cord (figure 8.16a). The ventral rootlets combine to form a ventral root on the ventral (anterior) side of the spinal cord, and the dorsal rootlets combine to form a dorsal root on the dorsal (posterior) side of the cord at each seg-ment. The ventral and dorsal roots unite just lateral to the spinal cord to form a spinal nerve. The dorsal root contains a ganglion, called the dorsal root ganglion (gang′ glē-on; a swelling or knot).
The cell bodies of pseudo-unipolar sensory neurons are in the dorsal root ganglia (figure 8.16b). The axons of these neurons originate in the periphery of the body. They pass through spinal nerves and the dorsal roots to the posterior horn of the spinal cord gray matter. In the posterior horn, the axons either synapse with interneurons or pass into the white matter and ascend or descend in the spinal cord.
The cell bodies of motor neurons, which regulate the activi-ties of muscles and glands, are located in the anterior and lateral horns of the spinal cord gray matter. Somatic motor neurons are in the anterior horn, and autonomic neurons are in the lateral horn.
Axons from the motor neurons form the ventral roots and pass into the spinal nerves. Thus, the dorsal root contains sensory axons, and the ventral root contains motor axons. Each spinal nerve therefore has both sensory and motor axons.
An example of a converging pathway involves a motor neuron in the spinal cord that stimulates muscle contraction (figure 8.17a). Sensory fibers from pain receptors carry action potentials to the spinal cord and synapse with interneurons, which in turn synapse with a motor neuron. Neurons in the cerebral cortex, controlling conscious movement, also synapse with the same motor neuron by way of axons in descending tracts. Both the interneurons and the neurons in the cerebral cortex have axons that converge on the motor neuron, which can therefore be stimulated either through the reflex arc or by conscious thought.
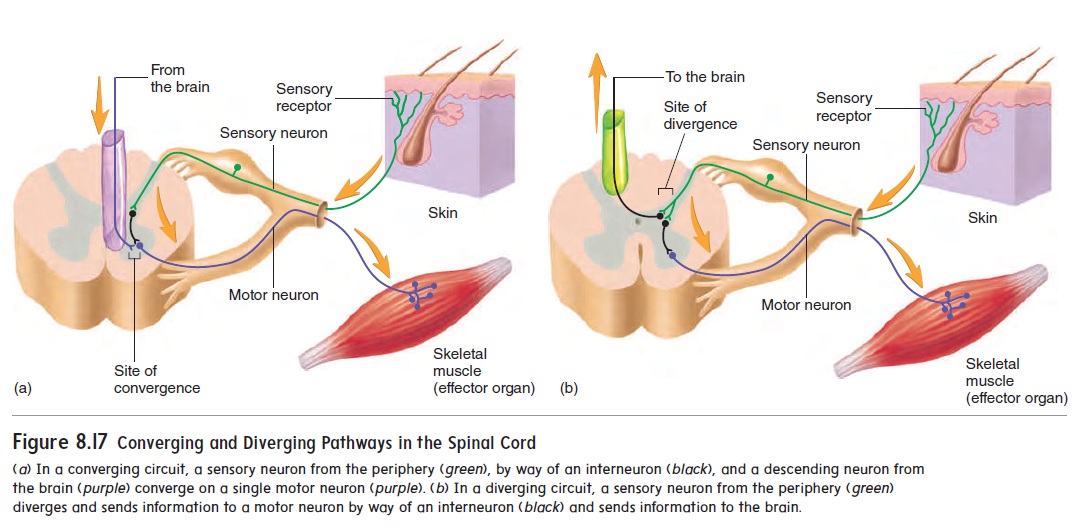
An example of a diverging pathway involves sensory neurons within the spinal cord (figure 8.17b). The axon of a sensory neu- ron carrying action potentials from pain receptors branches within the spinal cord. One branch produces a reflex response by synaps-ing with an interneuron. The interneuron, in turn, synapses with a motor neuron, which stimulates a muscle to withdraw the injured region of the body from the source of the pain. The other branch synapses with an ascending neuron that carries action potentials through a nerve tract to the brain, where the stimulation is inter-preted as pain.
Spinal Cord Reflexes
Knee-Jerk Reflex
The simplest reflex is the stretch reflex, in which muscles contract in response to a stretching force applied to them. The knee-jerkreflex, orpatellar reflex(figure 8.18), is a classic example of thestretch reflex. When the patellar ligament is tapped, the quadriceps femoris muscle tendon and the muscles themselves are stretched. Sensory receptors within these muscles are also stretched, and the stretch reflex is activated. Consequently, contraction of the muscles extends the leg, producing the characteristic knee-jerk response.
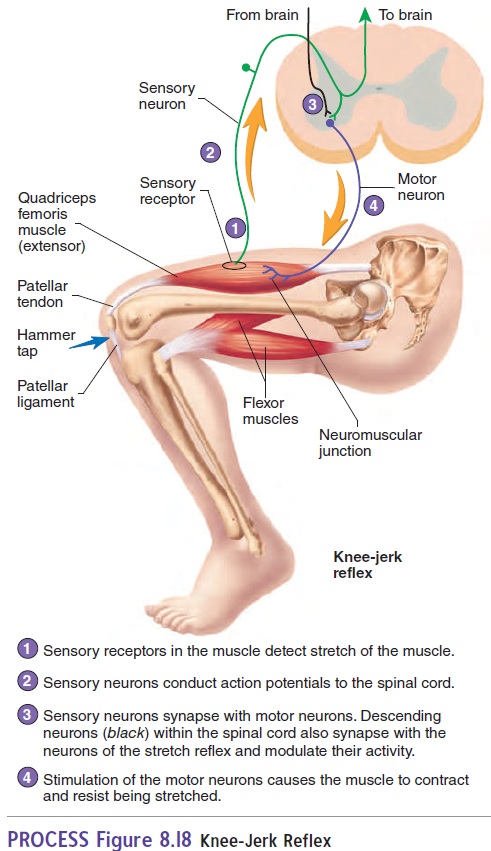
Clinicians use the knee-jerk reflex to determine if the higher CNS centers that normally influence this reflex are functional. Descending neurons within the spinal cord synapse with the neu-rons of the stretch reflex and modulate their activity. This activity is important in maintaining posture and in coordinating muscular activity. Following a severe spinal cord injury, all spinal reflexes are lost below the level of injury. By about 2 weeks after the injury, the knee-jerk reflex returns, but it is often exaggerated. When the stretch reflex is absent or greatly exaggerated, it indicates that the neurons within the brain or spinal cord that modify this reflex have been damaged.
Withdrawal Reflex
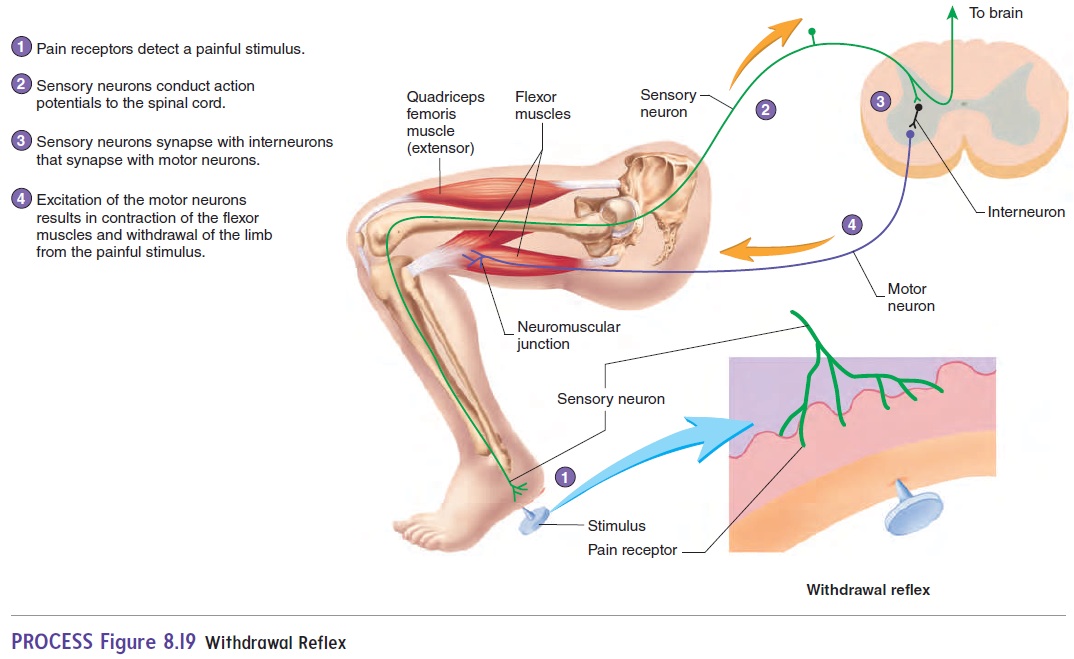
The function of the withdrawal reflex, or flexor reflex, is to remove a limb or another body part from a painful stimulus. The sensory receptors are pain receptors . Following painful stimuli, sensory neurons conduct action potentials through the dorsal root to the spinal cord, where the sensory neurons synapse with interneurons, which in turn synapse with motor neurons (figure 8.19). These neurons stimulate muscles, usually flexor mus-cles, that remove the limb from the source of the painful stimulus.
Related Topics