Chapter: Basic & Clinical Pharmacology : The Gonadal Hormones & Inhibitors
Physiologic Effects - The Estrogens
Physiologic Effects
A. Mechanism
Plasma estrogens in the blood and interstitial
fluid are bound to SHBG, from which they dissociate to enter the cell and bind
to their receptor. Two genes code for two estrogen receptor isoforms, α
and β,
which are members of the superfamily of steroid, sterol, retinoic acid, and
thyroid receptors. The estrogen receptors are found predominantly in the
nucleus bound to heat shock proteins that stabilize them (see Figure 39–4).
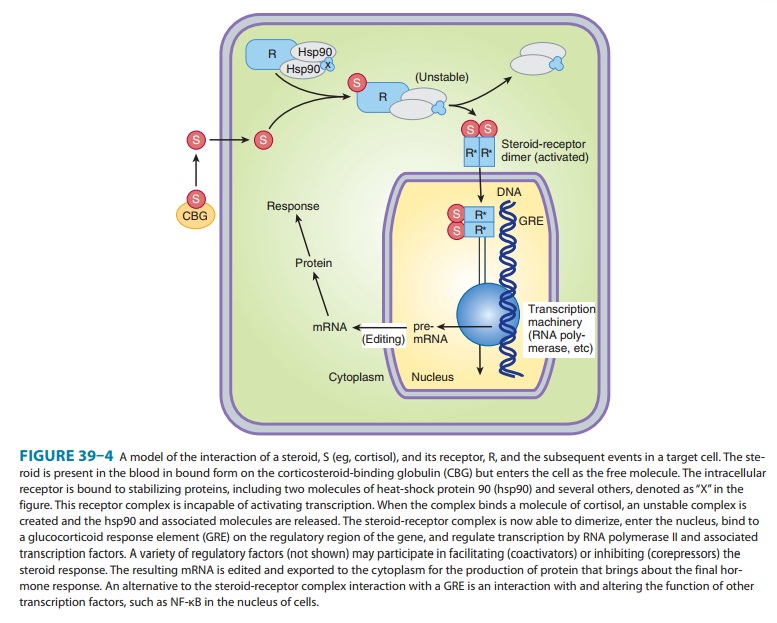
Binding of the hormone
to its receptor alters its conformation and releases it from the stabilizing
proteins (predominantly Hsp90). The receptor-hormone complex forms homodimers
that bind to a specific sequence of nucleotides called estrogen responseelements (EREs) in the promoters of various genes
and regulatetheir transcription. The ERE is composed of two half-sites arranged
as a palindrome separated by a small group of nucleotides called the spacer.
The interaction of a receptor dimer with the ERE alsoinvolves a number of
nuclear proteins, the coregulators, as well as components of the transcription
machinery. The receptor may also bind to other transcription factors to
influence the effects of these factors on their responsive genes.
The relative
concentrations and types of receptors, receptor coregulators, and transcription
factors confer the cell specificity of the hormone’s actions. The genomic
effects of estrogens are mainly due to proteins synthesized by translation of
RNA tran-scribed from a responsive gene. Some of the effects of estrogens are
indirect, mediated by the autocrine and paracrine actions of auta-coids such as
growth factors, lipids, glycolipids, and cytokinesproduced by the target cells
in response to estrogen.
Rapid
estrogen-induced effects such as granulosa cell Ca2+
uptake and increased uterine blood flow do not require gene acti-vation. These
appear to be mediated by nongenomic effects of the classic estrogen
receptor-estrogen complex, influencing several intracellular signaling
pathways.
Recently, all steroid
receptors except the mineralocorticoid receptors were shown to have
palmitoylation motifs that allow enzymatic addition of palmitate and increased
localization of the receptors in the vicinity of plasma membranes. Such
receptors are available for direct interactions with, and effects on, various
membrane-associated or cytoplasmic proteins without the need for entry into the
nucleus and induction of transcriptional actions.
B. Female Maturation
Estrogens
are required for the normal sexual maturation and growth of the female. They
stimulate the development of the vagina, uterus, and uterine tubes as well as
the secondary sex char-acteristics. They stimulate stromal development and
ductal growth in the breast and are responsible for the accelerated growth
phase and the closing of the epiphyses of the long bones that occur at puberty.
They contribute to the growth of axillary and pubic hair and alter the
distribution of body fat to produce typical female body contours. Larger
quantities also stimulate development of pigmentation in the skin, most
prominent in the region of the nipples and areolae and in the genital region.
C. Endometrial Effects
In
addition to its growth effects on uterine muscle, estrogen plays an important
role in the development of the endometrial lining. When estrogen production is
properly coordinated with the pro-duction of progesterone during the normal
human menstrual cycle, regular periodic bleeding and shedding of the
endometrial lining occur. Continuous exposure to estrogens for prolonged periods
leads to hyperplasia of the endometrium that is usually associated with
abnormal bleeding patterns.
D. Metabolic and Cardiovascular Effects
Estrogens have a
number of important metabolic and cardiovascu-lar effects. They seem to be
partially responsible for maintenance of the normal structure and function of
the skin and blood vessels in women. Estrogens also decrease the rate of
resorption of bone by promoting the apoptosis of osteoclasts and by
antagonizing the osteoclastogenic and pro-osteoclastic effects of parathyroid
hor-mone and interleukin-6. Estrogens also stimulate adipose tissue production
of leptin and are in part responsible for the higher levels of this hormone in
women than in men.
In addition to
stimulating the synthesis of enzymes and growth factors leading to uterine and
breast growth and differentiation, estrogens alter the production and activity
of many other proteins in the body. Metabolic alterations in the liver are
especially impor-tant, so that there is a higher circulating level of proteins
such as transcortin (corticosteroid-binding globulin, CBG), thyroxine-binding
globulin (TBG), SHBG, transferrin, renin substrate, and fibrinogen. This leads
to increased circulating levels of thyroxine, estrogen, testosterone, iron,
copper, and other substances.
Alterations in the
composition of the plasma lipids caused by estrogens are characterized by an
increase in the high-density lipo-proteins (HDL), a slight reduction in the
low-density lipoproteins (LDL), and a reduction in total plasma cholesterol
levels. Plasma triglyceride levels are increased. Estrogens decrease hepatic
oxida-tion of adipose tissue lipid to ketones and increase synthesis of
triglycerides.
E. Effects on Blood Coagulation
Estrogens
enhance the coagulability of blood. Many changes in factors influencing
coagulation have been reported, including increased circulating levels of
factors II, VII, IX, and X and decreased antithrombin III, partially as a
result of the hepatic effects mentioned above. Increased plasminogen levels and
decreased platelet adhesiveness have also been found (see Hormonal
Contraception, below).
F. Other Effects
Estrogens
induce the synthesis of progesterone receptors. They are responsible for
estrous behavior in animals and may influence behavior and libido in humans.
Administration of estrogens stimulates central components of the stress system,
including the production of corticotropin-releasing hormone and the activity of
the sympathetic system, and promotes a sense of well-being when given to women
who are estrogen-deficient. They also facilitate the loss of intravascular
fluid into the extracellular space, produc-ing edema. The resulting decrease in
plasma volume causes a compensatory retention of sodium and water by the
kidney. Estrogens also modulate sympathetic nervous system control of smooth
muscle function.
Related Topics