Chapter: Medical Surgical Nursing: Management of Patients With Dermatologic Problems
Viral Skin Infections
Viral Skin Infections
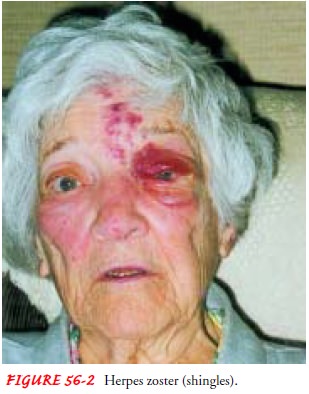
HERPES ZOSTER
Herpes zoster, also called shingles, is an
infection caused by the varicella-zoster virus, a member of a group of DNA
viruses. The viruses causing chickenpox and herpes zoster are
indistinguish-able, hence the name varicella-zoster virus. The disease is
charac-terized by a painful vesicular eruption along the area of distribution
of the sensory nerves from one or more posterior ganglia. It is as-sumed that
herpes zoster represents a reactivation of latent vari-cella virus infection
and reflects lowered immunity. After a case of chickenpox runs its course, it
is thought that the varicella-zoster viruses responsible for the outbreak lie
dormant inside nerve cells near the brain and spinal cord. Later, when these
la-tent viruses are reactivated, they travel by way of the peripheral nerves to
the skin, where the viruses multiply and create a red rash of small,
fluid-filled blisters. About 10% of adults get shingles during their lifetimes,
usually after age 50 years. There is an in-creased frequency of herpes zoster
infections among patients with weakened immune systems and cancers, especially
leukemias and lymphomas (Odom et al., 2000).
Clinical Manifestations
The eruption is usually accompanied or preceded by
pain, which may radiate over the entire region supplied by the affected nerves.
The pain may be burning, lancinating (ie, tearing or sharply cut-ting),
stabbing, or aching. Some patients have no pain, but itch-ing and tenderness
may occur over the area. Sometimes, malaise and gastrointestinal disturbances
precede the eruption. Thepatches of grouped vesicles appear on the red and
swollen skin. The early vesicles, which contain serum, later may become puru-lent,
rupture, and form crusts. The inflammation is usually uni-lateral, involving
the thoracic, cervical, or cranial nerves in a bandlike configuration. The
blisters are usually confined to a nar-row region of the face or trunk (Fig.
56-2). The clinical course varies from 1 to 3 weeks. If an ophthalmic nerve is
involved, the patient may have eye pain. Inflammation and a rash on the trunk
may cause pain with the slightest touch. The healing time varies from 7 to 26
days.
Herpes
zoster in healthy adults is usually localized and benign. However, in
immunosuppressed patients, the disease may be se-vere and the clinical course
acutely disabling.
Medical Management
The
goals of herpes zoster management are to relieve the pain and to reduce or
avoid complications, which include infection, scar-ring, and postherpetic
neuralgia and eye complications. Pain is controlled with analgesics, because
adequate pain control during the acute phase helps prevent persistent pain
patterns. Systemic corticosteroids may be prescribed for patients older than
age 50 years to reduce the incidence and duration of postherpetic neuralgia
(ie, persistent pain of the affected nerve after healing). Healing usually
occurs sooner in those who have been treated with corticosteroids. Triamcinolone
(Aristocort, Kenacort, Kenalog) injected subcutaneously under painful areas is
effective as an anti-inflammatory agent.
There
is evidence that infection is arrested if oral antiviral agents such as
acyclovir (Zovirax), valacyclovir (Valtrex), or fam-ciclovir (Famvir) are
administered within 24 hours of the initial eruption. Intravenous acyclovir, if
started early, is effective in sig-nificantly reducing the pain and halting the
progression of the disease. In older patients, the pain from herpes zoster may
persist as postherpetic neuralgia for months after the skin lesions dis-appear
(Hall, 2000).
Ophthalmic herpes zoster occurs when an eye is involved. This is considered an ophthalmic emergency, and the patient should be referred to an ophthalmologist immediately to prevent the possi-ble sequelae of keratitis, uveitis, ulceration, and blindness.
People
who have been exposed to varicella (ie, chicken pox) by primary infection or by
vaccination are not at risk for infec-tion after exposure to patients with
herpes zoster.
Nursing Management
The nurse assesses the patient’s discomfort and
response to med-ication and collaborates with the physician to make necessary
ad-justments to the treatment regimen. The patient is taught how to apply wet
dressings or medication to the lesions and to follow proper hand hygiene
techniques to avoid spreading the virus.
Diversionary
activities and relaxation techniques are encour-aged to ensure restful sleep
and to alleviate discomfort. A care-giver may be required to assist with
dressings, particularly if the patient is elderly and unable to apply them.
Relatives, neighbors, or a home care nurse may need to help with dressing
changes and food preparation for patients who cannot care for themselves or
prepare nourishing meals.
HERPES SIMPLEX
Herpes
simplex is a common skin infection. There are two types of the causative virus,
which are identified by viral typing. Generally, herpes simplex type 1 occurs
on the mouth and type 2 in the genital area, but both viral types can be found
in both locations. About 85% of adults worldwide are seropositive for herpes
type 1. The prevalence of type 2 is lower; type 2 usually appears at the onset
of sexual activity. Serologic testing shows that many more people are infected
than have a history of clinical disease.
Herpes
simplex is classified as a true primary infection, a non-primary initial
episode, or a recurrent episode. True primary in-fection is the initial
exposure to the virus. A nonprimary initial episode is the initial episode of
type 1 or type 2 in a person pre-viously infected with the other type.
Recurrent episodes are sub-sequent episodes of the same viral type.
OROLABIAL HERPES
Orolabial herpes, also called fever blisters or
cold sores, consists of erythematous-based clusters of grouped vesicles on the
lips. A prodrome of tingling or burning with pain may precede the ap-pearance
of the vesicles by up to 24 hours. Certain triggers, such as sunlight exposure
or increased stress, may cause recurrent episodes. Fewer than 1% of people with
primary orolabial herpes infections develop herpetic gingivostomatitis. This
complication occurs more in children and young adults. The onset is often
ac-companied by high fever, regional lymphadenopathy, and gener-alized malaise.
Another complication of orolabial herpes is the development of erythema
multiforme, an acute inflammation of the skin and mucous membranes with
characteristic lesions that have the appearance of targets.
GENITAL HERPES
Genital herpes, or type 2 herpes simplex, manifests
with a broad spectrum of clinical signs. Minor infections may produce no
symptoms at all; severe primary infections with type 1 can cause systemic
flulike illness. Lesions appear as grouped vesicles on an erythematous base
initially involving the vagina, rectum, or penis. New lesions can continue to
appear for 7 to 14 days. Lesions are symmetric and usually cause regional
lymphadenopathy. Fever and flulike symptoms are common. Typical recurrences
begin with a prodrome of burning, tingling, or itching about 24 hours before
the vesicles appear. As the vesicles rupture, erosions and ulcerations begin to
appear. Severe infections can cause extensive erosions of the vaginal or anal
canal.
Assessment and Diagnostic Findings
Herpes simplex infections are confirmed in several
ways. Gener-ally, the appearance of the skin eruption is strongly suggestive.
Viral cultures and rapid assays are available, and the type of test used
depends on lesion morphology. Acute vesicular lesions are more likely to react
positively to the rapid assay, whereas older, crusted patches are better
diagnosed with viral culture. In all cases, it is imperative to obtain enough
viral cells for testing, and careful collection methods are therefore
important. All crusts should be gently removed or vesicles gently unroofed. A
sterile cotton swab premoistened in viral culture preservative is used to swab
the base of the vesicle to obtain a specimen for analysis.
Complications
Eczema
herpeticum is a condition in which patients with eczema contract herpes that
spreads throughout the eczematous areas. The same type of spread of herpes can
occur in severe seborrhea, scabies, and other chronic skin conditions.
Herpes
Whitlow is an infection of the pulp of a fingertip with herpes type 1 or 2.
There is tenderness and erythema of the lateral fold of the cuticle.
Deep-seated vesicles appear within 24 hours.
Most
cases of neonatal infection with herpes occur during de-livery by contact of
the infant with the mother’s active ulcera-tions. Rarely, in mothers who have
primary infections during pregnancy, intrauterine neonatal infections occur.
Fetal anom-alies include skin lesions, microcephaly, encephalitis, and
intra-cerebral calcifications.
Medical Management
In many patients, recurrent orolabial herpes
represents more of a nuisance than a disease. Because sun exposure is a common
trig-ger, those with recurrent orolabial herpes should use a sunscreen
liberally on the lips and face. Topical treatment with drying agents may
accelerate healing. In more severe outbreaks or in pa-tients who have
identified a trigger, intermittent treatment with 200 mg of acyclovir
administered five times each day for 5 days is often started as soon as the
earliest symptoms occur.
Treatment
of genital herpes depends on the severity, the fre-quency, and the
psychological impact of recurrences and on the infectious status of the sexual
partner. For people who have mild or rare outbreaks, no treatment may be
required. For those who have more severe outbreaks, but for whom outbreaks are
still in-frequent, intermittent treatment as described for oral lesions can be
used. Because intermittent treatment reduces the duration of the infection by
only 24 to 36 hours, it should be initiated as early as possible.
Patients
who have more than six recurrences per year may benefit from suppressive
therapy. Use of acyclovir, valacyclovir, or famciclovir suppresses 85% of
recurrences, and 20% of pa-tients are free of recurrences during suppressive
therapy. Sup-pressive therapy also reduces viral shedding by almost 95%, making
the person less contagious. Treatment with suppressive doses of oral antiviral
medications prevents recurrent erythema multiforme.
Eczema
herpeticum is managed with oral or intravenous acyclovir.
Management
of genital herpes in pregnancy is controversial. Routine prenatal cultures do
not predict shedding at the time of delivery. The use of scalp electrodes
during delivery should be avoided because they increase the risk for infection
in the new-born. Because the risk for neonatal herpes is greater in women with
their initial episode during pregnancy, suppression therapy should be started
in these women to reduce outbreaks during the third trimester. All women with
active lesions at the time of de-livery undergo cesarean section.
In
immunocompromised patients, suppression therapy should be considered. In severe
infections of the hospitalized pa-tient, intravenous acyclovir is prescribed.
Related Topics