Chapter: Biology of Disease: Cancer
Prostate Cancer: Treatment, Signs, symptoms and staging
PROSTATE CANCER
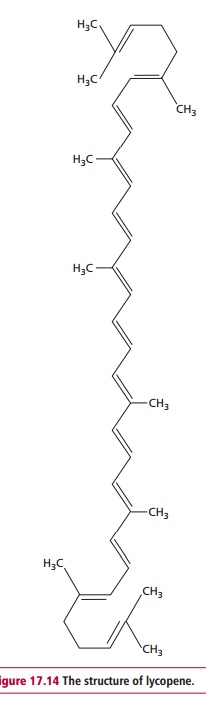
The prostate is a small gland, surrounding part of the urethra, which produces semen that mixes with the sperm produced by the testes as described. Prostate cancer is a disease that principallyaffects men over the age of 50 years. Many prostate cancers go undiagnosed because the tumor remains latent for long periods of time. The annual incidence of prostate cancer in the UK is about 30 000 men and around one in 12 men will develop the condition. In the USA the incidence is half that of the UK. Its incidence has increased in recent years, although this may reflect the increasing age of the population. While most prostate cancers are slow growing, a small proportion of tumors grow and metastasize more quickly. The risk of a man contracting prostate cancer are increased if close relatives have had the disease, or if female family members have had breast cancer, especially if they were diagnosed at an early age. Men of Afro-Caribbean and African–American origin are at greater risk of getting the disease while Asian men have the lowest risk. A diet high in animal fat and dairy products and low in fresh fruit and vegetables increases the risk. Consumption of the carotenoid, lycopene (Figure 17.14), which is abundant in tomatoes and tomato products, reduces the risk of contracting prostate cancer. Lycopene has been shown to lower the amount insulin-like growth factor 1, which may otherwise stimulate the growth of cancer cells.
Signs, symptoms, diagnosis and staging of prostate cancer
The symptoms of prostate cancer are not usually present when the tumor is small. However, as the tumor grows there is difficulty and pain on passing urine, coupled with a more frequent need to urinate, particularly at night. There may also be blood in the urine. If cancer cells have spread to the bone there may be pain in the back and pelvis.
A patient presenting with symptoms of prostate cancer will be given a digital rectal examination (DRE; Figure 17.33 (B)). During this examination a gloved finger is inserted into the rectum, from where the prostate can be felt. An enlarged prostate that feels round and smooth is most likely a benign prostate hyperplasia. In contrast, a prostate tumor will make the gland feel hard and lumpy. Blood samples are also taken for a PSA test. The PSA test measures the level of prostate specific antigen. The normal level of PSA is approximately 2.8 ng cm–3 in men of 50 and 5.3 ng cm–3 in men of 70 years of age. Men with levels of 10 ng cm–3 or above require referral for further
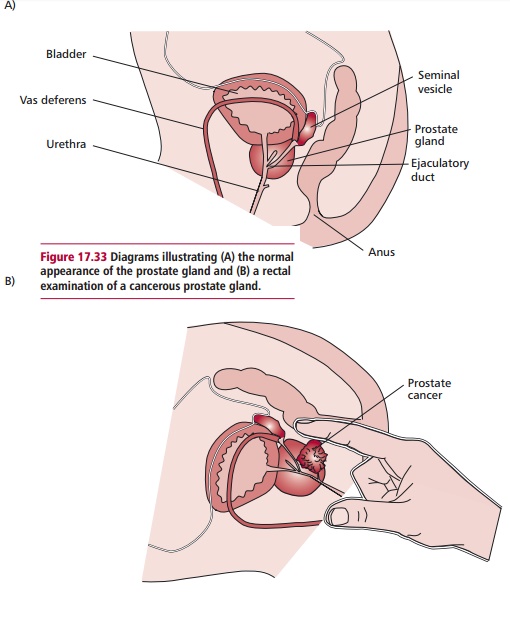
tests because above normal levels of PSA are found in conditions other than cancer, for example in urinary infections. Following referral, additional tests undertaken to determine the extent of the problem include an isotopic scan of bones and an MRI or CT scan. Biopsies of the prostate are obtained by passing a needle through the rectum into the prostate, aided by an ultrasound scan.
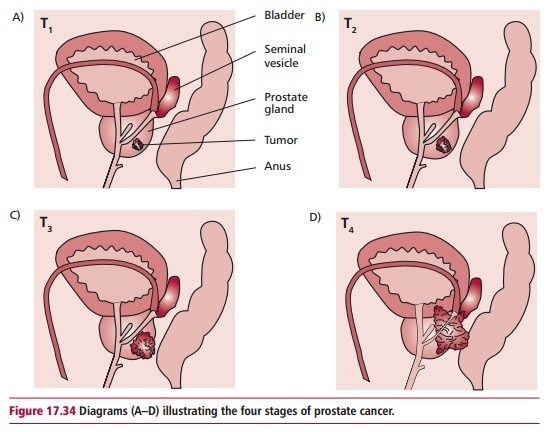
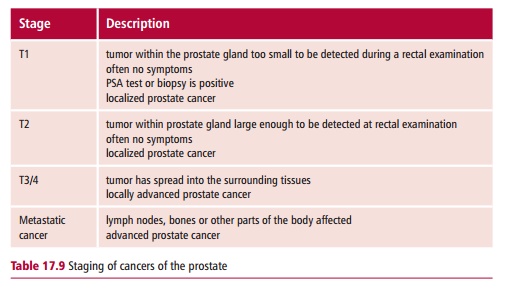
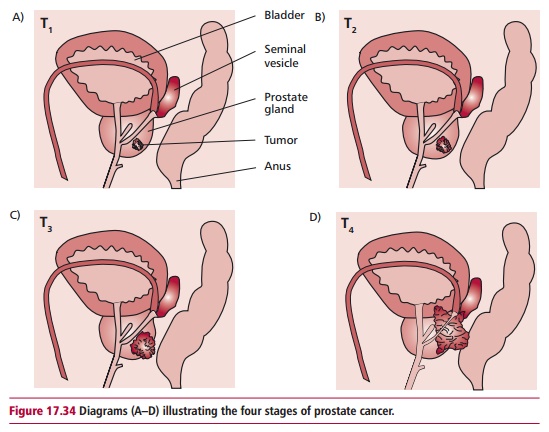
Prostate cancers are commonly graded using the Gleason system which scores the cancer according to the growth pattern and the arrangement of the cancer cells within the prostate. The higher the score, the more likely the tumor is to spread. The tumors are staged as shown in Table 17.9 and Figure 17.34.
Treatment for prostate cancer
The treatment for prostate cancer is determined by the grade and stage of the tumor, including metastasis, the age and health of the patient and the concentration of PSA in the blood. The range of treatments for early prostate cancer includes surgical removal of the prostate gland or prostatectomy, radiation therapy, hormonal therapy, or combinations of any or all of these. Chemotherapy is rarely used to treat prostate cancer. Depending on the age of the patient, an early stage cancer may not require treatment, but may be actively monitored until treatment is needed. Prostate cancers often grow slowly and the treatments, which have considerable side effects, should be restricted to the more aggressive forms of the disease. Prostatectomy is the removal of the whole prostate gland and may result in impotence and incontinence.
External radiation therapy may be given following surgery to ensure that any remaining cancer cells are destroyed. Radiation therapy is also used as a first line of treatment and is an equally effective alternative to surgery. Therapeutic approaches include external beam and brachytherapy. A form of external radiotherapy, known as conformational radiotherapy (CRT), allows the radiation beams to be shaped to match the shape of the prostate itself, which lowers the side effects caused by irradiation of the surrounding healthy tissue. Brachytherapy is delivered by the implantation of radioactive iodine ‘seeds’ or iridium wires in the prostate itself. If the cancer has spread to bone, radiation therapy using 89Strontium, which is preferentially taken up by bone tissue, is given by intravenous injection.
Prostate cancer cells have receptors for the active form of testosterone and their growth requires a supply of testosterone from the testes. The aim of hormone therapy is to lower testosterone levels. Some of the drugs used are analogs of gonadotrophin releasing hormone (GnRH), examples being goserelin, leuprorelin and triptorelin. Goserelin is administered as a subcutaneous pellet while the others are injected subcutaneously or intramuscularly in liquid form. Other drugs used are antiandrogens, which block the interactions of hormone and receptor. The side effects of hormonal therapy include sexual impotence, flushes and sweating which may be reduced by intermittently stopping and starting the therapy.
The prognosis for men with prostate cancer is generally good, since this type of cancer usually occurs in older men and grows slowly.
Related Topics