Chapter: Biology of Disease: Cancer
Leukemias: Chronic myelogenous, Acute myeloid, Acute lymphoblastic leukemia
LEUKEMIAS
Leukemias are tumors of bone marrow cells that give rise to the blood cells and platelets . Leukemias were historically classified according to the speed of onset and progression, with those of sudden onset and rapid progression termed acute leukemias, while those that develop slowly over months and years are called chronic leukemias. The current classification is based on specific typing of the blood cells, although the terms acute and chronic are still used. The main types of leukemias encountered clinically are acute myeloblastic and chronic myelogenous leukemias and acute lymphoblastic and chronic lymphocytic leukemias. Another rarer leukemia is hairy cell leukemia named according to the microscopic ‘hair-like’ appearance of the plasma membrane.Most leukemias are characterized by symptoms such as excessive bleeding of the gums and nose, bruising, fatigue, breathless
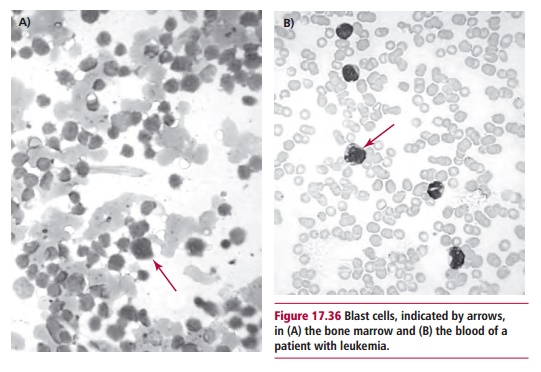
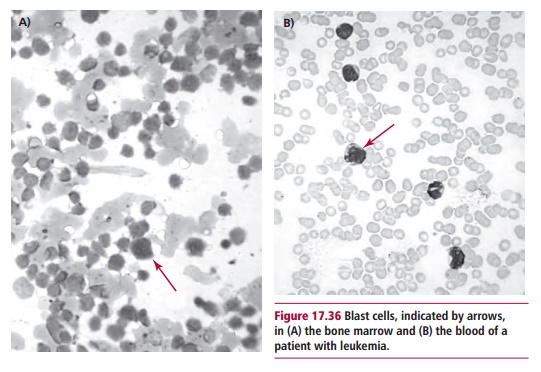
ness and increased susceptibility to infections. These are due to inadequate production of erythrocytes, platelets and lymphocytes owing to the abnormal proliferation of leukemic cells in the bone marrow. Blood and bone marrow films may show immature blast cells (Figures 17.36). Treatments for leukemia may involve chemotherapy, radiation therapy and stem cell transplantation .
Chronic myelogenous leukemia
Chronic myelogenous leukemia (CML) is a rare disorder that affects approximately 500 people annually in the UK and accounts for between 7 and 15% of all leukemias. Patients are usually adults between the ages of 40 and 60 years. The disease is caused by malignant transformation of a myeloid stem cell which would normally give rise to the polymorphonuclear leukocytes, monocytes, basophils, erythrocytes and megakaryocytes. The clonal proliferation of a myeloid stem cell results in the accumulation of
immature and mature myeloid cells within the bone marrow and spleen. Chronic myelogenous leukemia usually follows a clinical pattern in which there is a benign chronic phase, an accelerated phase and a blastic or blast crisis phase. During the chronic phase there are few signs and symptoms and many patients are asymptomatic. Patients may present with fatigue, anorexia and weight loss, and splenomegaly, with the condition being revealed by a routine blood count during the investigation of these symptoms. The blood count shows a leukocytosis, that is, an increased number of leukocytes, ranging from 10 q 109 to more than 500 q 109 cells dm–3. A blood smear also shows large numbers of neutrophils and immature myelocytes. The Philadelphia chromosome is present in 95% of cases. Splenomegaly may be present on examination. The presence of myeloblasts within a peripheral blood smear indicates a worsening of the disease and progression into the accelerated phase and the rapidly fatal blast crisis. This may take between three and five years from diagnosis.
Two major treatments are available for CML. The first is stem cell transplantation following radiation therapy to destroy the patient’s own bone marrow . The second is to use imanitib mesylate (Glivec) together with IFN- α. Imanitib mesylate is an inhibitor of tyrosine kinase that is administered orally. It is directed against the bcr-abl protein and is successful in inducing disease remission in approximately90% of patients. However, the remainder are resistant, while up to 25% of patients also develop resistance during treatment. Chemotherapy with hydroxyurea may also be used. This is a temporary measure that reduces the leukocyte count by suppressing the division of the malignant cells. The effectiveness of treatment can be monitored by detecting the proportion of cells with the Philadelphia translocation.
Acute myeloid (myeloblastic) leukemia
Acute myeloid leukemia (AML) is a rare disease that affects approximately 2000 adults, mostly over the age of 60 years, and 100 children annually in the UK. The disease is characterized by the presence of immature myeloid cells, or myeloblasts, in the blood, due to clonal proliferation of an aberrant cell in the bone marrow. The cause of AML is unknown, though it has been linked to exposure to industrial solvents. There is no genetic link and cases are sporadic.
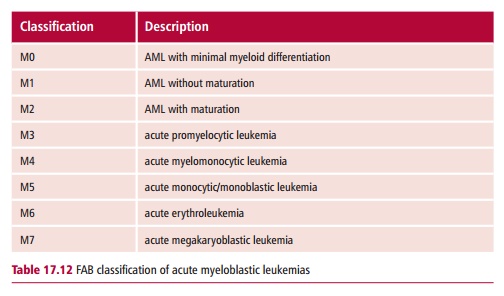
Acute myeloid leukemias are classified according to the type of cell which is involved, using the FAB (French–American–British) classification (Table17.12).
Patients present with anemia and bruising due to inadequate production of erythrocytes and platelets respectively. Poor platelet production is also associated with bleeding from the gums and nose. An inadequate production of appropriate leukocytes means that patients suffer repeated infections. Acute myeloid leukemia requires rapid diagnosis and immediate treatment. Chemotherapy is effective in bringing many patients into remission although high dose chemotherapy followed by a stem cell transplant may be required in some cases. Patients may require platelet transfusions before and during their treatment and erythropoietin may be given to treat the anemia. The use of the monoclonal antibody, gemtuzumab ozogamicin, directed at CD33 proteins present on the surfaces of the leukemic cells may be of some efficacy.
The prognosis for AML depends on the age at diagnosis. For adults under the age of 55 years, the five-year survival rate is between 40 and 60%, for those over 55 years it is unfortunately only 20%.
Chronic lymphocytic leukemia
Chronic lymphocytic leukemia (CLL) is the most common form of leukemia, affecting mostly those aged over 60 years. It is characterized by the clonal proliferation of lymphoid stem cells. However, the disease is slow growing and many patients are asymptomatic in the early stages. Signs and symptoms include frequent infections, anemia, bleeding and bruising. The spleen and the lymph nodes in the neck, axillae and groin may be swollen due to the accumulation of abnormal cells. The cause of CLL is unknown although in a minority of cases the disease may be familial. A diagnosis of CLL is by examination of blood and bone marrow. A lymph node biopsy may also be taken for histological examination. The disease is described as Stage A, B or C according to the degree of lymph node involvement. Stage C patients have enlarged lymph nodes in three or more areas and a low erythrocyte and/or platelet count. Patients with Stage A, with little or no lymph node enlargement may not need treatment. Patients with Stages B and C may be brought into remission with chemotherapy. Treatment is usually successful in maintaining remissions for several years.
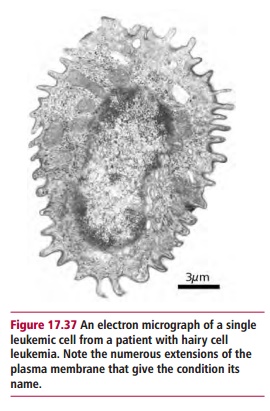
Hairy cell leukemia is a rare form of CLL which occurs in people between 40 and 60 years of age. It constitutes 2–5% of leukemias. The leukemic cell is a B lymphocyte and is characterized by cells with outgrowths or projections which give the disorder its name (Figure 17.37) although the cause of the pathology is not known. Patients present with symptoms of breathlessness, weakness, weight loss and infections. There may also be splenomegaly. Diagnosis is by examination of blood smears and demonstration of splenomegaly on examination. Histological examination of a bone marrow specimen is also undertaken.
Treatment of hairy cell leukemia is by chemotherapy, using cytotoxic drugs. Interferon α has also been used to treat this disorder. The prognosis for hairy cell leukemia is good. The leukemia is slow growing and chemotherapy may only be needed after regular monitoring of cell counts reveals the count of abnormal cells is rising and if the patient presents with symptoms.
Acute lymphoblastic leukemia
Acute lymphoblastic leukemia (ALL) is a rare disorder that occurs most frequently in children under the age of 15 years although it does affect around 600 adults annually in the UK, mostly between the ages of 15 and 25 and those over 75 years of age. The cause of ALL is unknown. The disease is characterized by a clonal proliferation of a lymphoid stem cell, leading to increased numbers of lymphoblasts in the blood. As with other leukemias, patients may present with unusual bleeding of the gums and nose, bruising, anemia, aching
joints and bones and a general feeling of malaise. Diagnosis is achieved by microscopic examination of bone marrow taken from the pelvis or sternum. A lumbar puncture may be used to obtain a sample of cerebrospinal fluid, to detect the presence of leukemic cells.
Acute lymphoblastic leukemia is classified into three types according to the FAB classification. These are L1ALL, in which the lymphoblasts resemble mature lymphocytes, with L2ALL and L3ALL showing increasingly immature forms of lymphoblasts. The disease may also be classified according to whether the leukemic cells are T cells or B cells, or pre-B cells, which are immature forms. A diagnosis of these forms involves histological examination and immunofluorescence testing of cell surface characteristics, with analysis by flow cytometry. A proportion of ALL patients also have the Philadelphia chromosome, which can be shown by karyotyping.
The treatment for ALL involves chemotherapy and this achieves remission in 80% of patients. Chemotherapy may also require intrathecal injection of chemotherapeutic agents to destroy leukemic cells in the cerebrospinal fluid. Steroids, such as dexamethasone, may be combined with cytotoxic drugs and imanitib may also be used. Radiation therapy to the brain and the testes in men may also be required to prevent recurrence. When patients are at high risk of relapse, a stem cell transplant may be required.
The survival rates for ALL depend on the age at which it is diagnosed. Children with ALL have a five-year survival rate of between 65 and 75%, while for adults it is only 20–35%.
Related Topics