Chapter: Biology of Disease: Disorders of the Blood
Microcytic Anemias
MICROCYTIC ANEMIAS
The major causes of microcytic anemias are iron deficiency, thalassemias, sideroblastic anemia and the anemia of chronic disease. Iron is difficult to absorb because of problems connected with the low solubility of its salts, its oxidation state, and interaction with other components of the diet. Loss of iron also occurs in hemorrhage and menstruation.
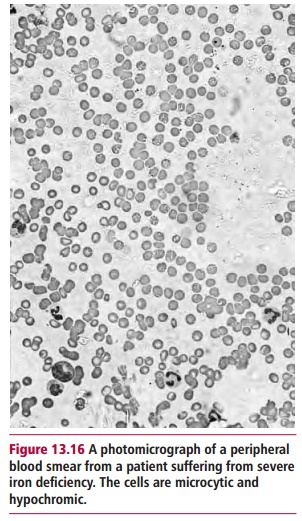
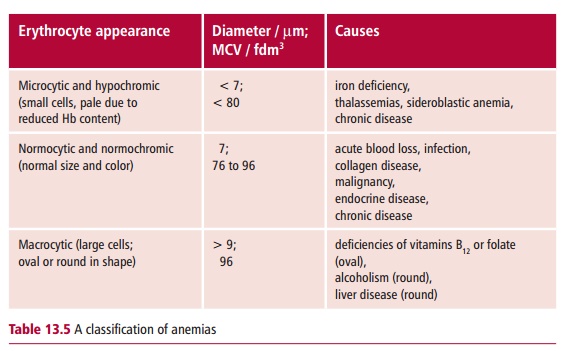
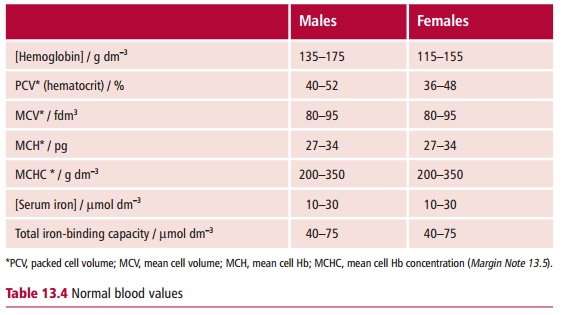
Iron deficiency anemia, the commonest cause of anemia worldwide, shows a number of characteristic features. The erythrocytes (Figure 13.16) are microcytic, with an MCV of less than 80 fdm3, and hypochromic, the MCH being less than 27 pg. There is variation in, cell sizes, anisocytosis and poikilocytosis, that is abnormal shapes, and a reduced reticulocyte count. There are also changes in the bone marrow, for example erythroid hypoplasia and decreased iron deposits. The serum iron decreases while the serum iron binding capacity increases compared with their normal concentration (Table 13.4). The transferrin saturation, that is the proportion of serum iron to its total iron binding capacity, falls below 19%, compared with a more usual 30% or so. The concentration of serum ferritin resulting from cellular degradation is regarded as the most reliable measurement of anemia. Patients may also show an impaired ability to maintain body temperature, depressed muscle function and abnormal thyroid hormone metabolism.
The underlying cause of the iron deficiency should be identified by the appropriate tests and taking a careful history of the patient. To counteract the deficiency, 600 mg of ferrous sulfate is given orally each day. If there are side effects, such as nausea, diarrhea or constipation, then ferrous gluconate may be substituted. Failure to respond to the treatment may be due to lack of patient compliance, continuing hemorrhage, severe malabsorption, or another cause for the anemia. It may be necessary to give iron parentally if absorption is defective, as for example in patients with ulcerative colitis or Crohn’s disease .
Related Topics