Chapter: Essentials of Anatomy and Physiology: Respiratory System
Lungs - Anatomy of the Respiratory System
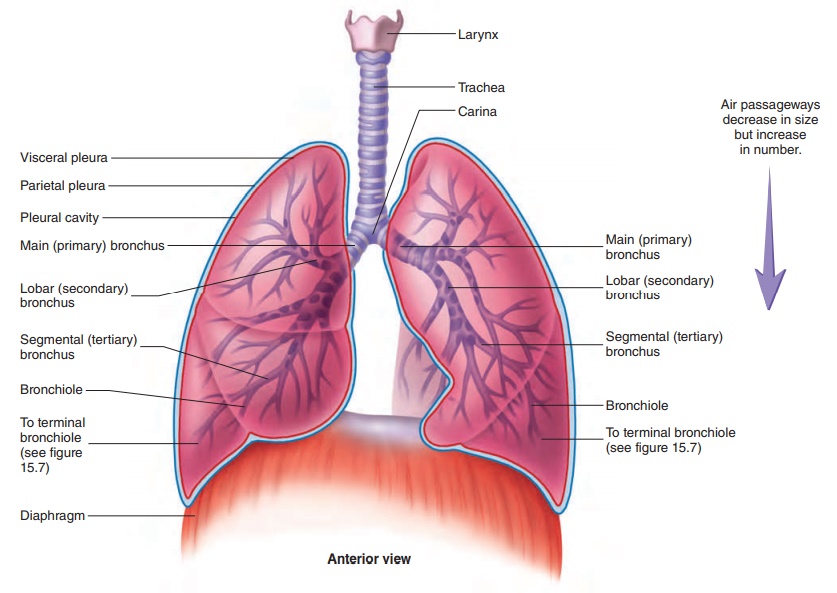
Lungs
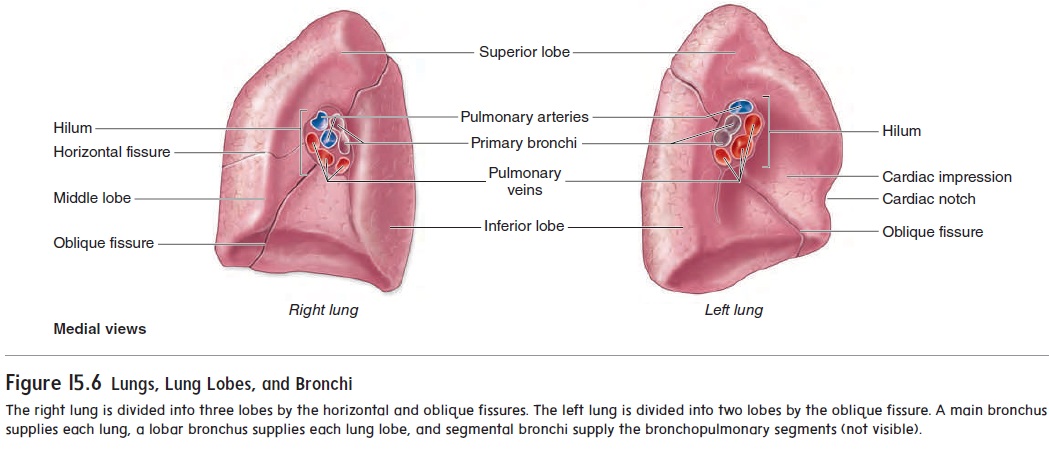
The lungs are the principal organs of respiration. Each lung is cone-shaped, with its base resting on the diaphragm and its apex extending superiorly to a point about 2.5 cm above the clavicle (figure 15.5). The right lung has three lobes, called the superior, middle, and inferior lobes. The left lung has two lobes, called the superior and inferior lobes (figure 15.6). The lobes of the lungs are separated by deep, prominent fissures on the lung surface. Each lobe is divided into bronchopulmonary segments separated from one another by connective tissue septa, but these separations are not visible as surface fissures. Individual diseased bronchopulmo-nary segments can be surgically removed, leaving the rest of the lung relatively intact, because major blood vessels and bronchi do not cross the septa. There are nine bronchopulmonary segments in the left lung and ten in the right lung.
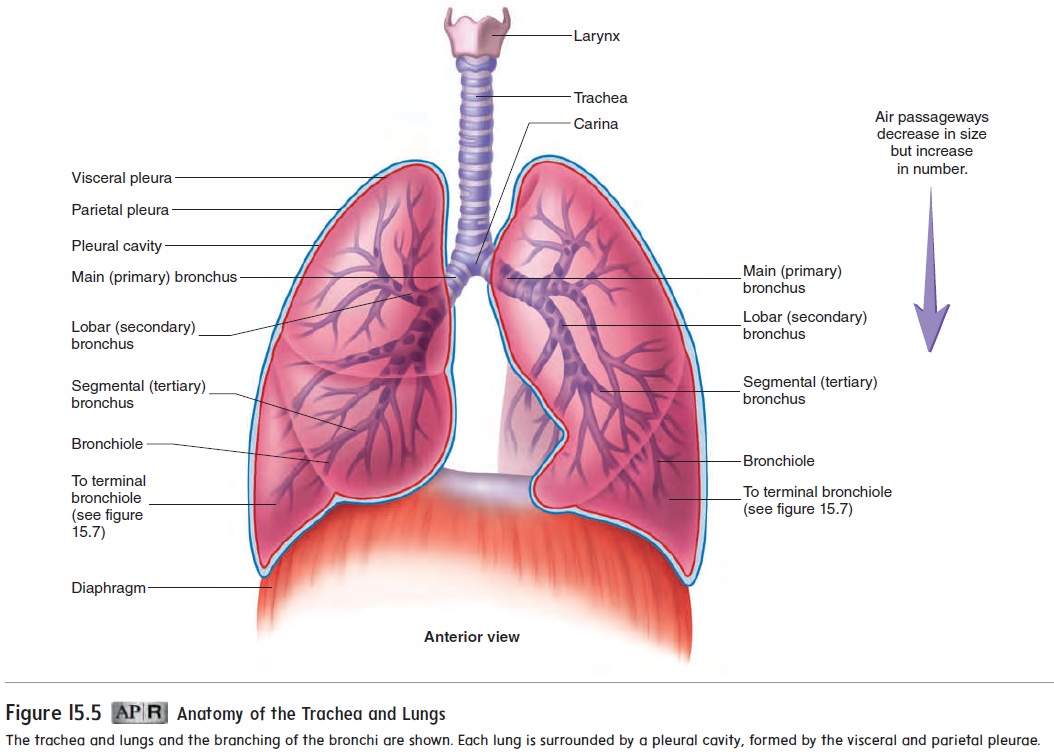
The main bronchi branch many times to form the tracheo-bronchial tree (see figure 15.5). Each main bronchus divides intolobar bronchi as they enter their respective lungs (figure 15.6). The lobar bronchi (orsecondary bronchi), two in the left lung andthree in the right lung, conduct air to each lobe. The lobar bronchi in turn give rise to segmental bronchi (or tertiary bronchi), which extend to the bronchopulmonary segments of the lungs. The bronchi continue to branch many times, finally giving rise to bronchioles.
The bronchioles also subdivide numerous times to give rise to terminal bronchioles, which then subdivide into respiratory bronchioles (figure 15.7). Each respiratory bronchiolesubdivides to form alveolar (al-vē′ ō-lăr) ducts, which are like long, branching hallways with many open doorways. The doorways open into alveoli (al-vē′ ō-lı̄; hollow sacs), which are small air sacs. The alveoli become so numerous that the alveolar duct wall is little more than a succession of alveoli. The alveolar ducts end as two or three alveolar sacs, which are chambers connected to two or more alveoli. There are about 300 million alveoli in the lungs.
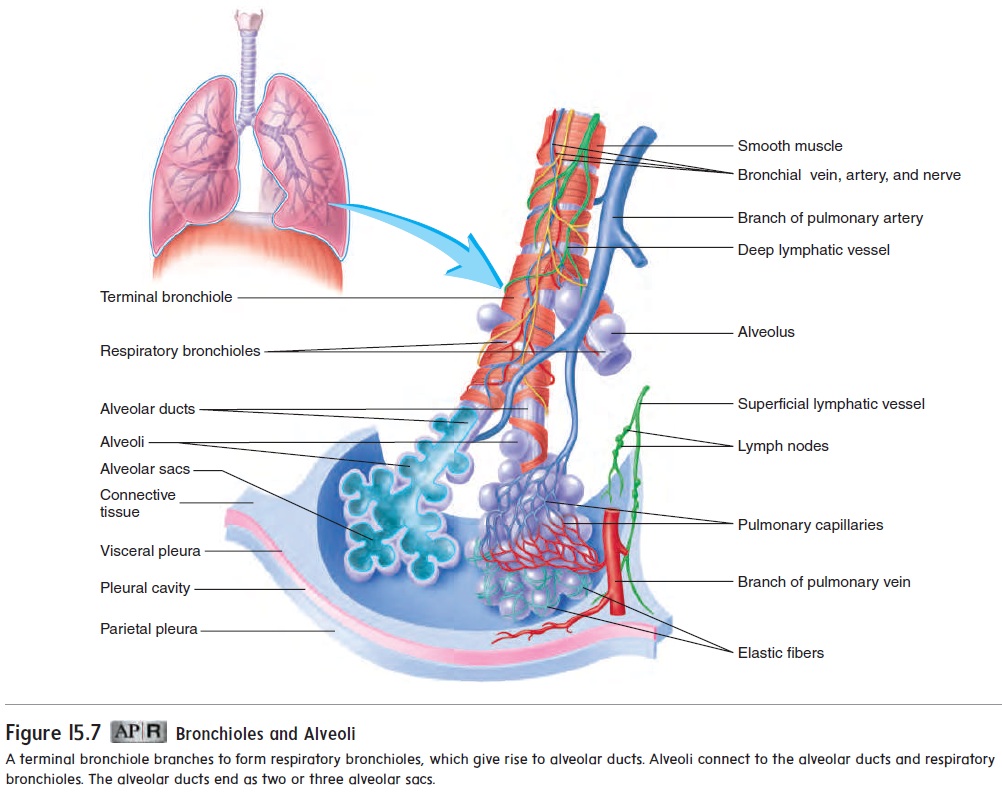
As the air passageways of the lungs become smaller, the structure of their walls changes. The amount of cartilage decreases and the amount of smooth muscle increases until, at the terminal bronchioles, the walls have a prominent smooth muscle layer but no cartilage. Relaxation and contraction of the smooth muscle within the bronchi and bronchioles can change the diameter of the air pas-sageways. For example, during exercise the diameter can increase, thus increasing the volume of air moved. During an asthma attack, however, contraction of the smooth muscle in the terminal bronchi-oles can result in greatly reduced airflow (see Systems Pathology). In severe cases, air movement can be so restricted that death results. Fortunately, medications, such as albuterol (al-bū′ ter-ol), help counteract the effects of an asthma attack bypromoting smooth muscle relaxation in the walls of terminal bron-chioles, so that air can flow more freely.
As the air passageways of the lungs become smaller, the lining of their walls also changes. The trachea and bronchi have pseu-dostratified ciliated columnar epithelium, the bronchioles have cili-ated simple columnar epithelium, and the terminal bronchioles have ciliated simple cuboidal epithelium. The ciliated epithelium of the air passageways functions as a mucus-cilia escalator, which traps debris from the inhaled air and removes it from the respiratory system.
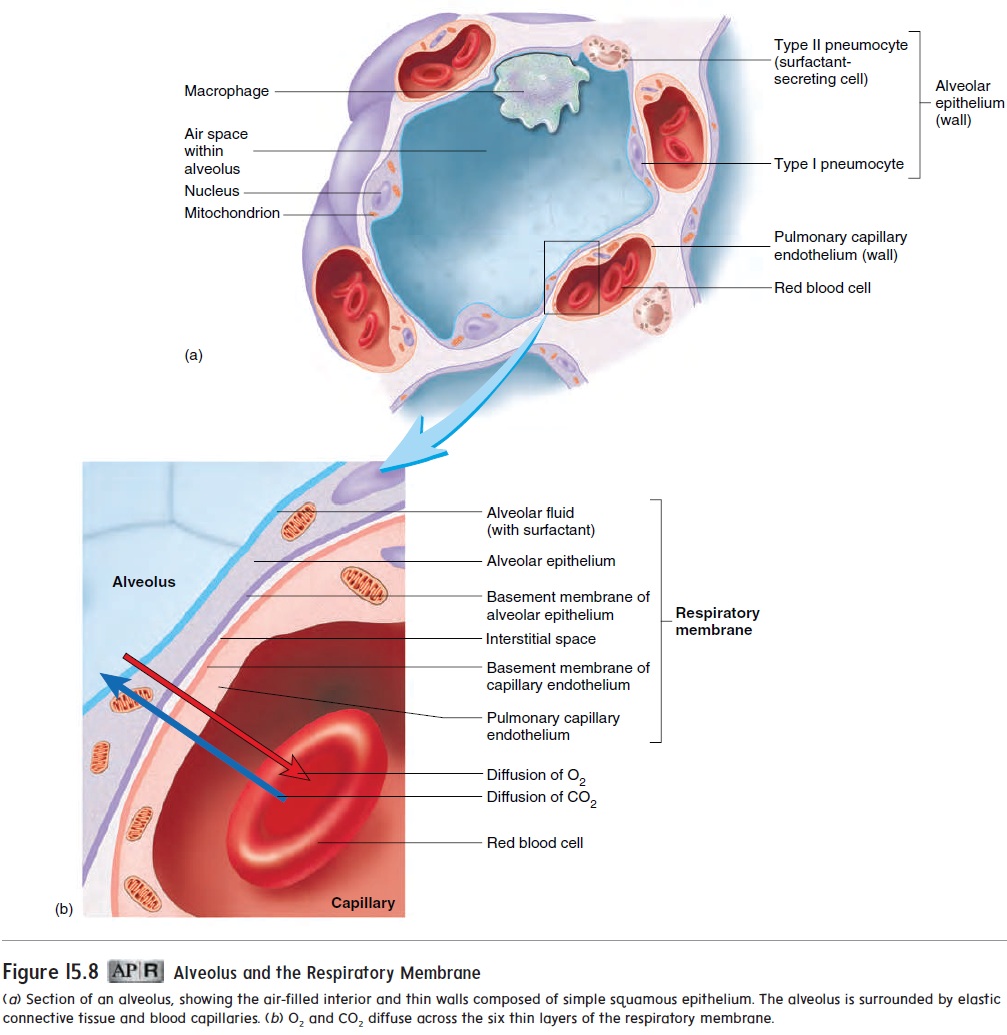
As the air passageways beyond the terminal bronchioles become smaller, their walls become thinner. The walls of the respiratory bronchioles are composed of cuboidal epithelium, and those of the alveolar ducts and alveoli are simple squamous epithelium. The respiratory membrane of the lungs is where gas exchange between the air and blood takes place. It is formed mainly by the walls of the alveoli and the surrounding capillaries (figure 15.8), but the alveolar ducts and respiratory bronchioles also contribute. The respiratory membrane is very thin to facilitate the diffusion of gases. It consists of six layers:
1. a thin layer of fluid lining the alveolus
2. the alveolar epithelium, composed of simple squamous epithelium
3. the basement membrane of the alveolar epithelium
4. a thin interstitial space
5. the basement membrane of the capillary endothelium
6. the capillary endothelium, composed of simple squamous epithelium
The elastic fibers surrounding the alveoli (figure 15.8) allow them to expand during inspiration and recoil during expiration. The lungs are very elastic and, when inflated, are capable of expelling the air and returning to their original, uninflated state. Specialized secretory cells within the walls of the alveoli (figure 15.8) secrete a chemical, called surfactant, that reduces the tendency of alveoli to recoil (see “Lung Recoil” later).
Related Topics