Chapter: Essentials of Anatomy and Physiology: Respiratory System
Anatomy of the Respiratory System
ANATOMY OF THE RESPIRATORY SYSTEM
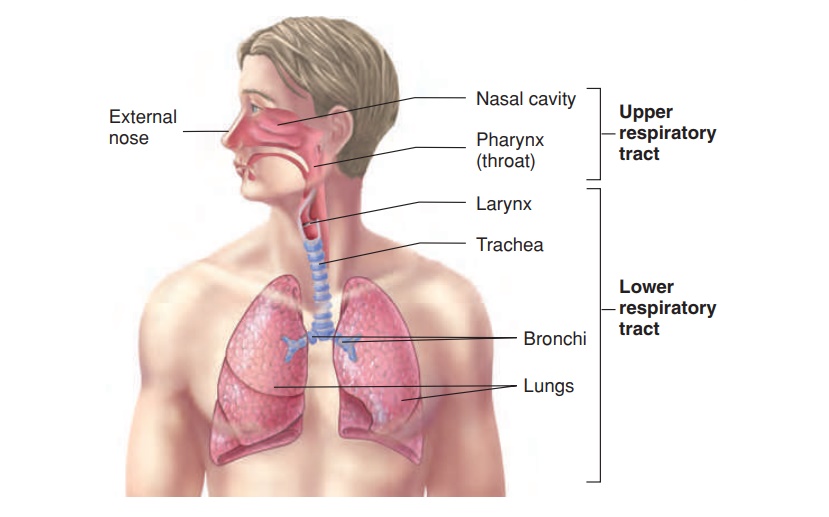
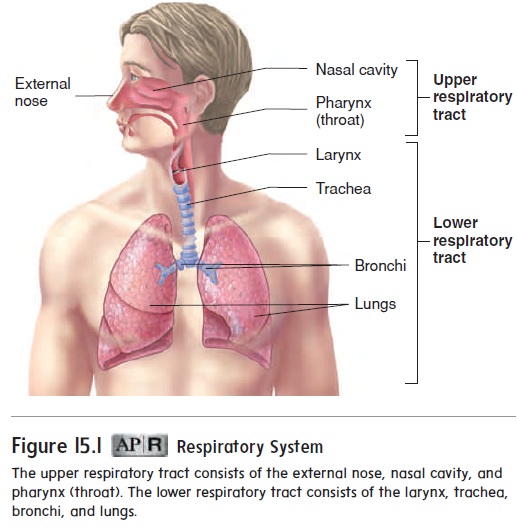
The respiratory system is divided into the upper respiratory tract and the lower respiratory tract (figure 15.1). The upperrespiratory tract includes the external nose, the nasal cavity, thepharynx, and associated structures; the lower respiratory tract includes the larynx, the trachea, the bronchi, and the lungs. Keep in mind, however, that upper and lower respiratory tract are not official anatomical terms. Rather, they are arbitrary divisions for the purposes of discussion, and some anatomists define them differently. For example, one alternative places the larynx in the upper respiratory tract. Also, the oral cavity is considered part of the digestive system, not the respiratory system, even though air frequently passes through the oral cavity.
Nose
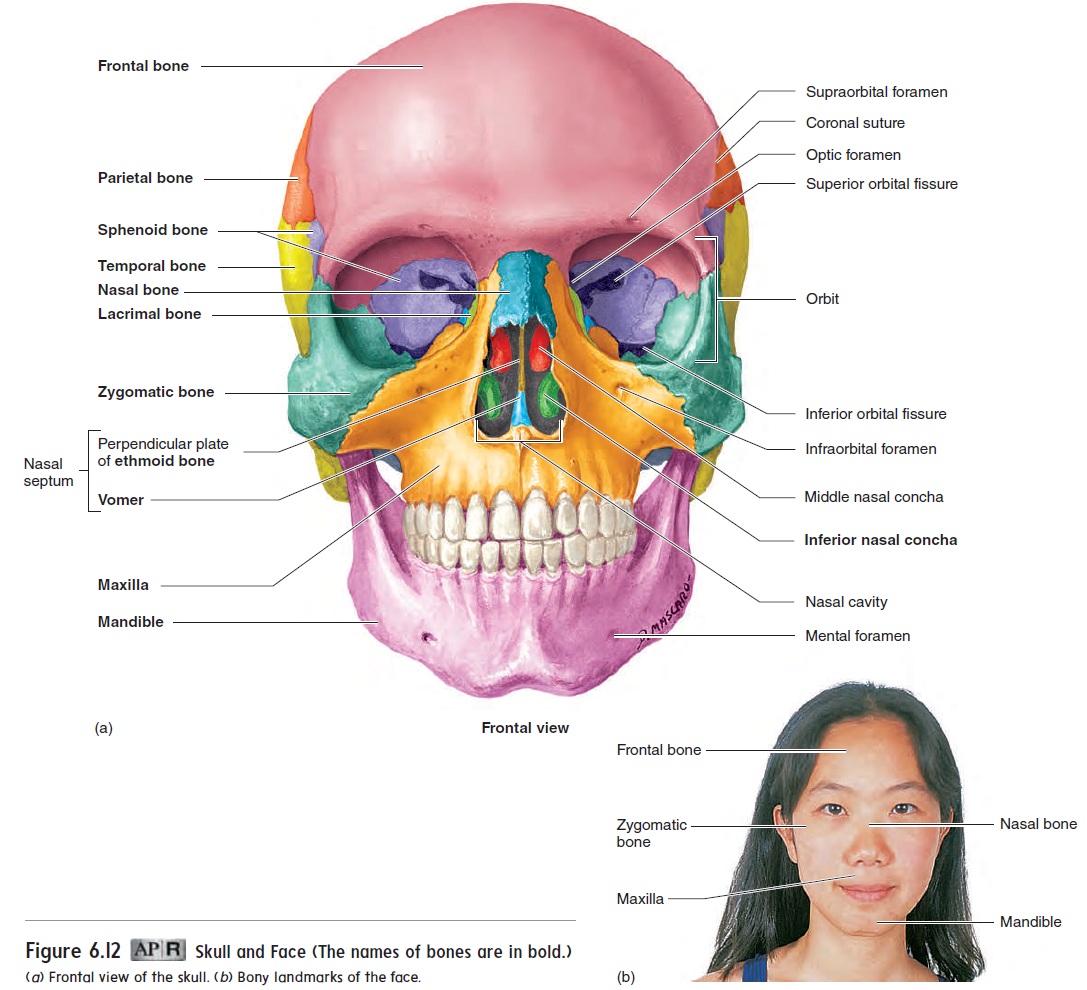
The nose consists of the external nose and the nasal cavity. The external nose is the visible structure that forms a prominent fea-ture of the face. Most of the external nose is composed of hyaline cartilage, although the bridge of the external nose consists of bone (see figure 6.12). The bone and cartilage are covered by connective tissue and skin.
The nares (nā′ rēs; sing. nā′ris), or nostrils, are the external openings of the nose, and the choanae (k ō′ an-ē; funnels) are the openings into the pharynx. The nasal (nā′ zăl) cavity extends from
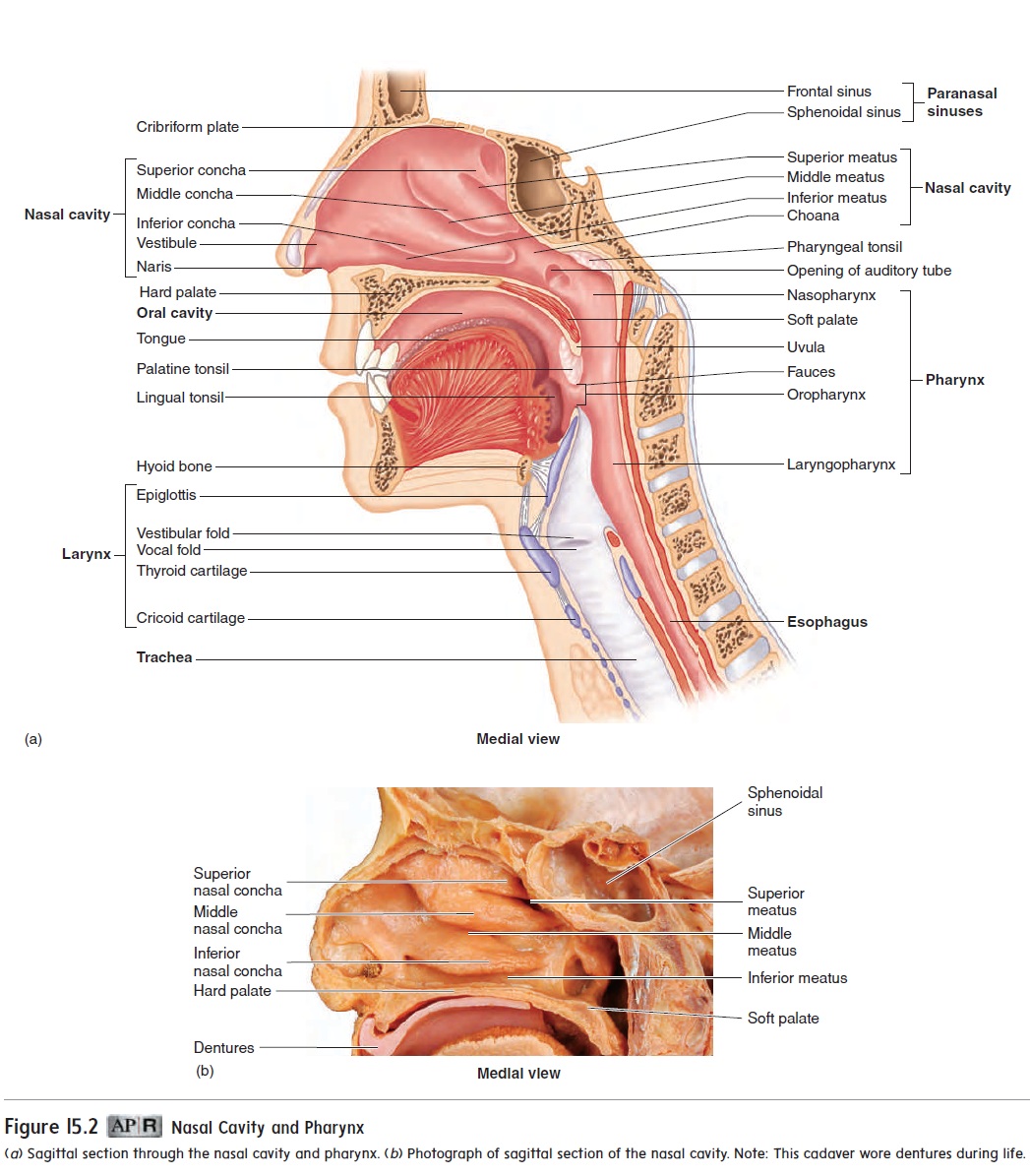
The nasal septum is a parti-tion dividing the nasal cavity into right and left parts. A deviatednasal septum occurs when the septum bulges to one side. The hard palate(pal′ăt) forms the floor of the nasal cavity, separat-ing the nasal cavity from the oral cavity. Air can flow through the nasal cavity when the oral cavity is closed or full of food.
Three prominent bony ridges called conchae (kon′ kē) are present on the lateral walls on each side of the nasal cavity. The conchae increase the surface area of the nasal cavity and cause air to churn, so that it can be cleansed, humidified, and warmed.
The paranasal (par-ă-nā′ săl) sinuses are air-filled spaces within bone. They include the maxillary, frontal, ethmoidal, and sphenoidal sinuses, each named for the bones in which they are located. The paranasal sinuses open into the nasal cavity and are lined with a mucous membrane. They reduce the weight of the skull, produce mucus, and influence the quality of the voice by acting as resonating chambers.
The nasolacrimal (nā-zō-lak′ ri-măl) ducts, which carry tears from the eyes, also open into the nasal cavity. Sensory receptors for the sense of smell are in the superior part of the nasal cavity .
Air enters the nasal cavity through the nares. Just inside the nares, the lining of the cavity is composed of stratified squamous epithelium containing coarse hairs. The hairs trap some of the large particles of dust suspended in the air. The rest of the nasal cavity is lined with pseudostratified columnar epithelial cells containing cilia and many mucus-producing goblet cells . Mucus produced by the goblet cells also traps debris in the air. The cilia sweep the mucus posteriorly to the pharynx, where it is swallowed. As air flows through the nasal cavities, it is humidified by moisture from the mucous epithelium and warmed by blood flowing through the superficial capillary net-works underlying the mucous epithelium.
The sneeze reflex dislodges foreign substances from the nasal cavity. Sensory receptors detect the foreign substances, and action potentials are conducted along the trigeminal nerves to the medulla oblongata, where the reflex is triggered. During the sneeze reflex, the uvula and the soft palate are depressed, so that rapidly flowing air from the lungs is directed primarily through the nasal passages, although a considerable amount passes through the oral cavity.
About 17–25% of people have a photic sneeze reflex, which is stimulated by exposure to bright light, such as the sun. Another reflex, the pupillary reflex, causes the pupils to con-strict in response to bright light. Physiologists speculate that the complicated “wiring” of the pupillary and sneeze reflexes are intermixed in some people, so that, when bright light activates a pupillary reflex, it also activates a sneeze reflex. Sometimes the photic sneeze reflex is fancifully called ACHOO, which stands for autosomal-dominant-compelling-helio-ophthalmic-outburst.
Pharynx
The pharynx (far′ ingks; throat) is the common passageway for both the respiratory and the digestive systems. Air from the nasal cavity and air, food, and water from the mouth pass through the pharynx. Inferiorly, the pharynx leads to the rest of the respiratory system through the opening into the larynx and to the digestive system through the esophagus. The pharynx can be divided into three regions: the nasopharynx, the oropharynx, and the laryngo-pharynx (figure 15.2a).
The nasopharynx (nā′ zō-far′ ingks) is the superior part of the pharynx. It is located posterior to the choanae and superior to the soft palate, which is an incomplete muscle and connective tissue partition separating the nasopharynx from the oropharynx. The uvula (ū′ vū-lă; a little grape) is the posterior extension of the soft palate. The soft palate forms the floor of the nasopharynx. The nasopharynx is lined with pseudostratified ciliated columnar epithelium that is continuous with the nasal cavity. The auditory tubes extend from the middle ears and open into the nasopharynx. The posterior part of the nasopharynx contains the pharyngeal (fă-rin′ jē-ăl) tonsil, which helps defend the body against infection . The soft palate is elevated during swallowing; this movement closes the nasopharynx and prevents food from passing from the oral cavity into the nasopharynx.
The oropharynx (ōr′ ō-far′ ingks) extends from the uvula to the epiglottis, and the oral cavity opens into the oropharynx. Thus, food drink, and air all pass through the oropharynx. The oropharynx is lined with stratified squamous epithelium, which protects against abrasion. Two sets of tonsils, the palatine tonsils and the lingual ton-sil, are located near the opening between the mouth and the orophar-ynx. Thepalatine (pal′ ă-tı̄n) tonsils are located in the lateral walls near the border of the oral cavity and the oropharynx. The lingualtonsil is located on the surface of the posterior part of the tongue.
The laryngopharynx (lă-ring′ gō-far-ingks) passes posterior to the larynx and extends from the tip of the epiglottis to the esophagus. Food and drink pass through the laryngopharynx to the esophagus. A small amount of air is usually swallowed with the food and drink. Swallowing too much air can cause excess gas in the stomach and may result in belching. The laryngopharynx is lined with stratified squamous epithelium and ciliated columnar epithelium.
Larynx
The larynx (lar′ ingks) is located in the anterior throat and extends from the base of the tongue to the trachea (figure 15.2a). It is a pas-sageway for air between the pharynx and the trachea. The larynx consists of an outer casing of nine cartilages connected to one another by muscles and ligaments (figure 15.3). Three of the nine cartilages are unpaired, and six of them form three pairs. The largest cartilage is the unpaired thyroid (thı̄′ royd; shield-shaped) cartilage, or Adam’s apple. The thyroid cartilage is attached superiorly to the hyoid bone. The most inferior cartilage of the larynx is the unpaired cricoid (krı̄′koyd; ring-shaped) cartilage, which forms the base ofthe larynx on which the other cartilages rest. The thyroid and cricoid cartilages maintain an open passageway for air movement.
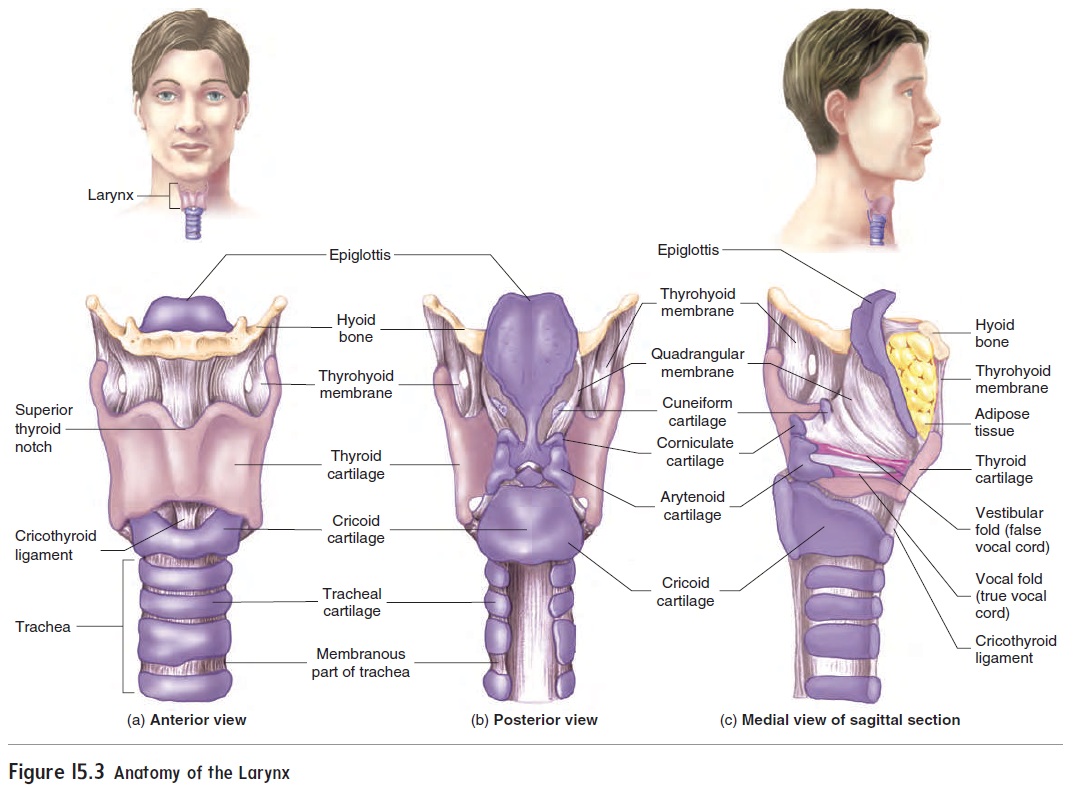
The third unpaired cartilage is the epiglottis (ep-i-glot′ is; on the glottis). It differs from the other cartilages in that it consists of elastic cartilage rather than hyaline cartilage. Its inferior margin is attached to the thyroid cartilage anteriorly, and the superior part of the epiglottis projects superiorly as a free flap toward the tongue. The epiglottis helps prevent swallowed materials from entering the larynx. As the larynx elevates during swallowing, the epiglottis tips posteriorly to cover the opening of the larynx.
The six paired cartilages consist of three cartilages on each side of the posterior part of the larynx (figure 15.3b). The top carti-lage on each side is the cuneiform (kū′ nē-i-fōrm; wedge-shaped) cartilage, the middle cartilage is the corniculate (kōr-nik′ū-lāt;horn-shaped) cartilage, and the bottom cartilage is the arytenoid (ar-i-tē′ noyd; ladle-shaped) cartilage. The arytenoid cartilages articulate with the cricoid cartilage inferiorly. The paired carti-lages form an attachment site for the vocal folds.
Two pairs of ligaments extend from the posterior surface of the thyroid cartilage to the paired cartilages. The superior pair forms the vestibular (ves-tib′ ū-lăr) folds, or false vocal cords, and the inferior pair composes the vocal folds, or true vocal cords (figure 15.4). When the vestibular folds come together, they pre-vent air from leaving the lungs, as when a person holds his or her breath. Along with the epiglottis, the vestibular folds also prevent food and liquids from entering the larynx.
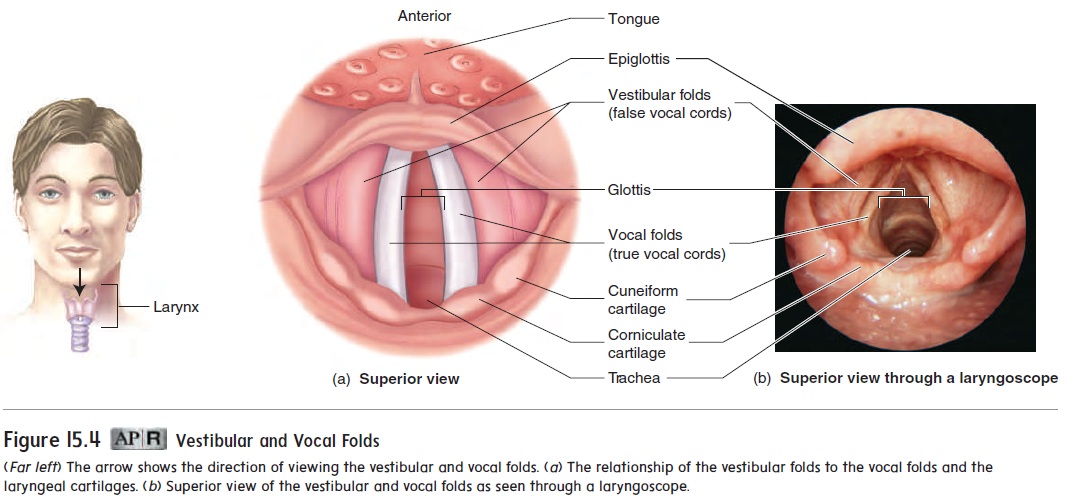
The vocal folds are the primary source of voice production. Air moving past the vocal folds causes them to vibrate, producing sound. Muscles control the length and tension of the vocal folds. The force of air moving past the vocal folds controls the loudness, and the tension of the vocal folds controls the pitch of the voice. An inflammation of the mucous epithelium of the vocal folds is called laryngitis (lar-in-jı̄′ tis). Swelling of the vocal folds during laryngitis inhibits voice production.
Trachea
The trachea (tr̄a ′ k̄e -̆a ), or windpipe, is a membranous tube attached to the larynx. It consists of connective tissue and smooth muscle, reinforced with 16–20 C-shaped pieces of hyaline cartilage (see figure 15.3). The adult trachea is about 1.4–1.6 centimeters (cm) in diameter and about 10–11 cm long. It begins immediately infe-rior to the cricoid cartilage, which is the most inferior cartilage of the larynx. The trachea projects through the mediastinum and
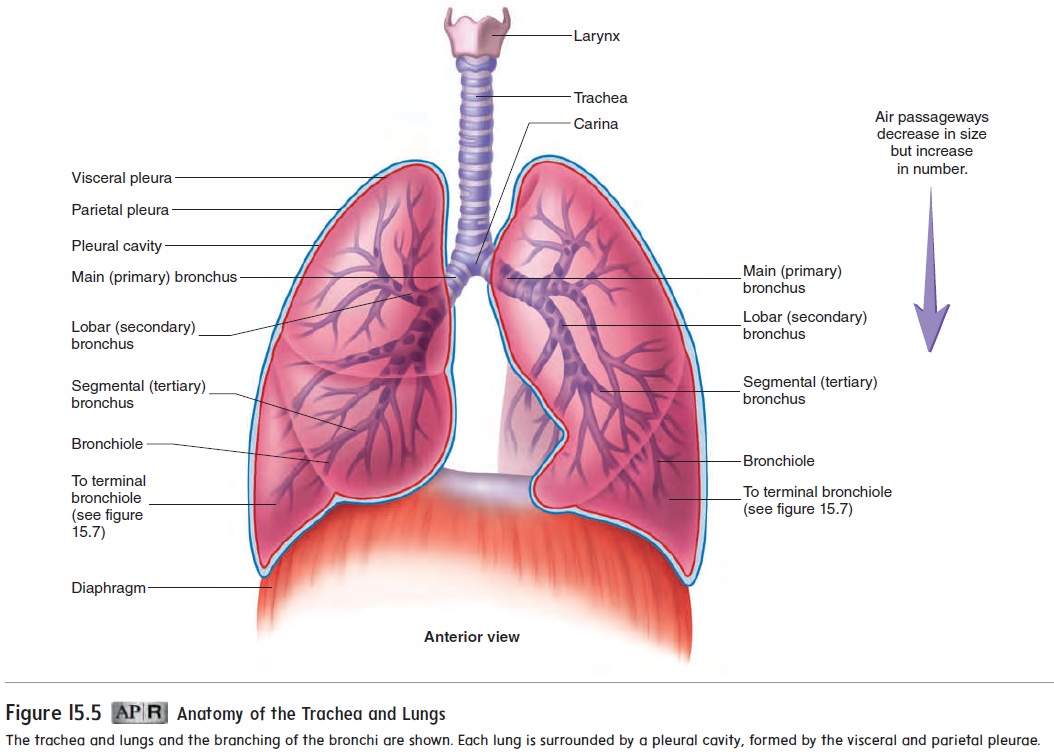
divides into the right and left primary bronchi at the level of the fifth thoracic vertebra (figure 15.5). The esophagus lies immedi-ately posterior to the trachea (see figure 15.2a).
C-shaped cartilages form the anterior and lateral sides of the trachea. The cartilages protect the trachea and maintain an open passageway for air. The posterior wall of the trachea has no carti-lage and consists of a ligamentous membrane and smooth muscle (see figure 15.3b). The smooth muscle can alter the diameter of
This occurs, for example, when the cough reflex dislodges foreign substances from the trachea. Sensory receptors detect the foreign substance, and action potentials travel along the vagus nerves to the medulla oblongata, where the cough reflex is triggered. During coughing, the smooth muscle of the trachea contracts, decreasing the trachea’s diameter. As a result, air moves rapidly through the trachea, which helps expel mucus and foreign substances. Also, the uvula and soft palate are elevated, so that air passes primarily through the oral cavity.
The trachea is lined with pseudostratified columnar epithelium, which contains numerous cilia and goblet cells. The cilia propel mucus produced by the goblet cells, as well as foreign particles embedded in the mucus, out of the trachea, through the larynx, and into the pharynx, from which they are swallowed.
Constant, long-term irritation of the trachea by cigarette smoke can cause the tracheal epithelium to change to stratified squamous epithelium. The stratified squamous epithelium has no cilia and therefore cannot clear the airway of mucus and debris. The accu-mulations of mucus provide a place for microorganisms to grow, resulting in respiratory infections. Constant irritation and inflamma-tion of the respiratory passages stimulate the cough reflex, resulting in “smoker’s cough.”
Bronchi
The trachea divides into the left and right main bronchi (brong′ k ; sing. bronchus, brong′ kŭ s; windpipe), or primary bronchi, each of which connects to a lung. The left main bronchus is morehorizontal than the right main bronchus because it is displaced by the heart (figure 15.5). Foreign objects that enter the trachea usu-ally lodge in the right main bronchus, because it is wider, shorter, and more vertical than the left main bronchus and is more in direct line with the trachea. The main bronchi extend from the trachea to the lungs. Like the trachea, the main bronchi are lined with pseudostratified ciliated columnar epithelium and are supported by C-shaped pieces of cartilage.
Lungs
The lungs are the principal organs of respiration. Each lung is cone-shaped, with its base resting on the diaphragm and its apex extending superiorly to a point about 2.5 cm above the clavicle (figure 15.5). The right lung has three lobes, called the superior, middle, and inferior lobes. The left lung has two lobes, called the superior and inferior lobes (figure 15.6). The lobes of the lungs are separated by deep, prominent fissures on the lung surface. Each lobe is divided into bronchopulmonary segments separated from one another by connective tissue septa, but these separations are not visible as surface fissures. Individual diseased bronchopulmo-nary segments can be surgically removed, leaving the rest of the lung relatively intact, because major blood vessels and bronchi do not cross the septa. There are nine bronchopulmonary segments in the left lung and ten in the right lung.
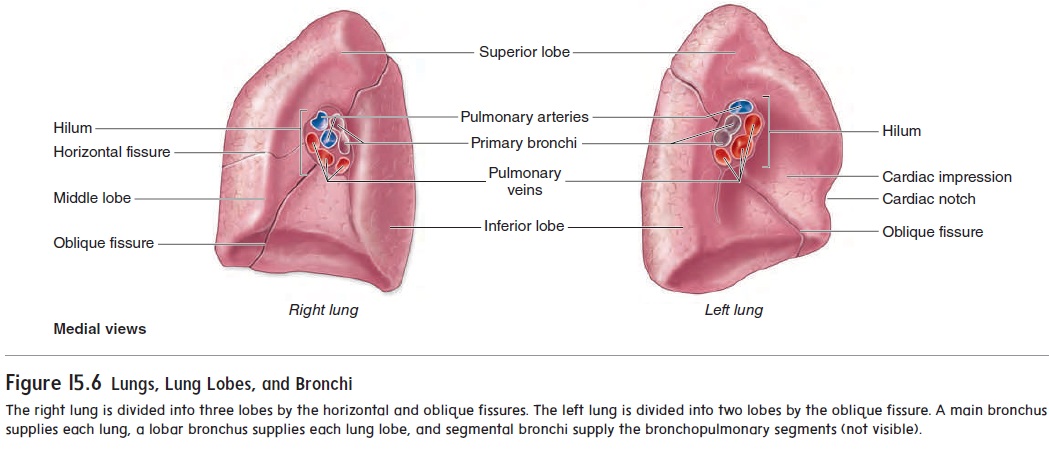
The main bronchi branch many times to form the tracheo-bronchial tree (see figure 15.5). Each main bronchus divides intolobar bronchi as they enter their respective lungs (figure 15.6). The lobar bronchi(orsecondary bronchi), two in the left lung andthree in the right lung, conduct air to each lobe. The lobar bronchi in turn give rise to segmental bronchi (or tertiary bronchi), which extend to the bronchopulmonary segments of the lungs.
The bronchi continue to branch many times, finally giving rise to bronchioles (brong′ kē-ōlz). The bronchioles also subdivide numerous times to give rise to terminal bronchioles, which then subdivide into respiratory bronchioles (figure 15.7). Each respiratory bronchiolesubdivides to form alveolar (al-vē′ ō-lăr) ducts, which are like long, branching hallways with many open doorways. The doorways open into alveoli (al-vē′ ō-lı̄; hollow sacs), which are small air sacs. The alveoli become so numerous that the alveolar duct wall is little more than a succession of alveoli. The alveolar ducts end as two or three alveolar sacs, which are chambers connected to two or more alveoli. There are about 300 million alveoli in the lungs.
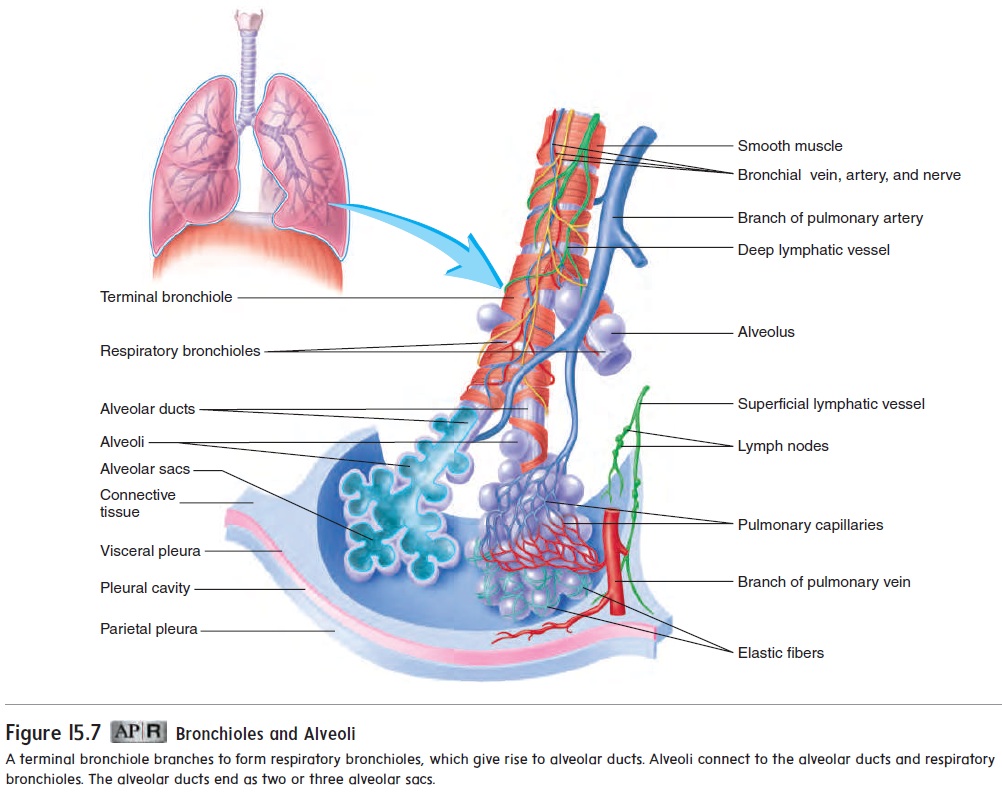
As the air passageways of the lungs become smaller, the structure of their walls changes. The amount of cartilage decreases and the amount of smooth muscle increases until, at the terminal bronchioles, the walls have a prominent smooth muscle layer but no cartilage. Relaxation and contraction of the smooth muscle within the bronchi and bronchioles can change the diameter of the air pas-sageways. For example, during exercise the diameter can increase, thus increasing the volume of air moved. During an asthma attack, however, contraction of the smooth muscle in the terminal bronchi-oles can result in greatly reduced airflow (see Systems Pathology). In severe cases, air movement can be so restricted that death results. Fortunately, medications, such as albuterol (al-bū′ ter-ol), help counteract the effects of an asthma attack bypromoting smooth muscle relaxation in the walls of terminal bron-chioles, so that air can flow more freely.
As the air passageways of the lungs become smaller, the lining of their walls also changes. The trachea and bronchi have pseu-dostratified ciliated columnar epithelium, the bronchioles have cili-ated simple columnar epithelium, and the terminal bronchioles have ciliated simple cuboidal epithelium. The ciliated epithelium of the air passageways functions as a mucus-cilia escalator, which traps debris from the inhaled air and removes it from the respiratory system.
As the air passageways beyond the terminal bronchioles become smaller, their walls become thinner. The walls of the respiratory bronchioles are composed of cuboidal epithelium, and those of the alveolar ducts and alveoli are simple squamous epithelium. The respiratory membrane of the lungs is where gas exchange between the air and blood takes place. It is formed mainly by the walls of the alveoli and the surrounding capillaries (figure 15.8), but the alveolar ducts and respiratory bronchioles also contribute. The respiratory membrane is very thin to facilitate the diffusion of gases. It consists of six layers:
1. a thin layer of fluid lining the alveolus
2. the alveolar epithelium, composed of simple squamous epithelium
3. the basement membrane of the alveolar epithelium
4. a thin interstitial space
5. the basement membrane of the capillary endothelium
6. the capillary endothelium, composed of simple squamous epithelium
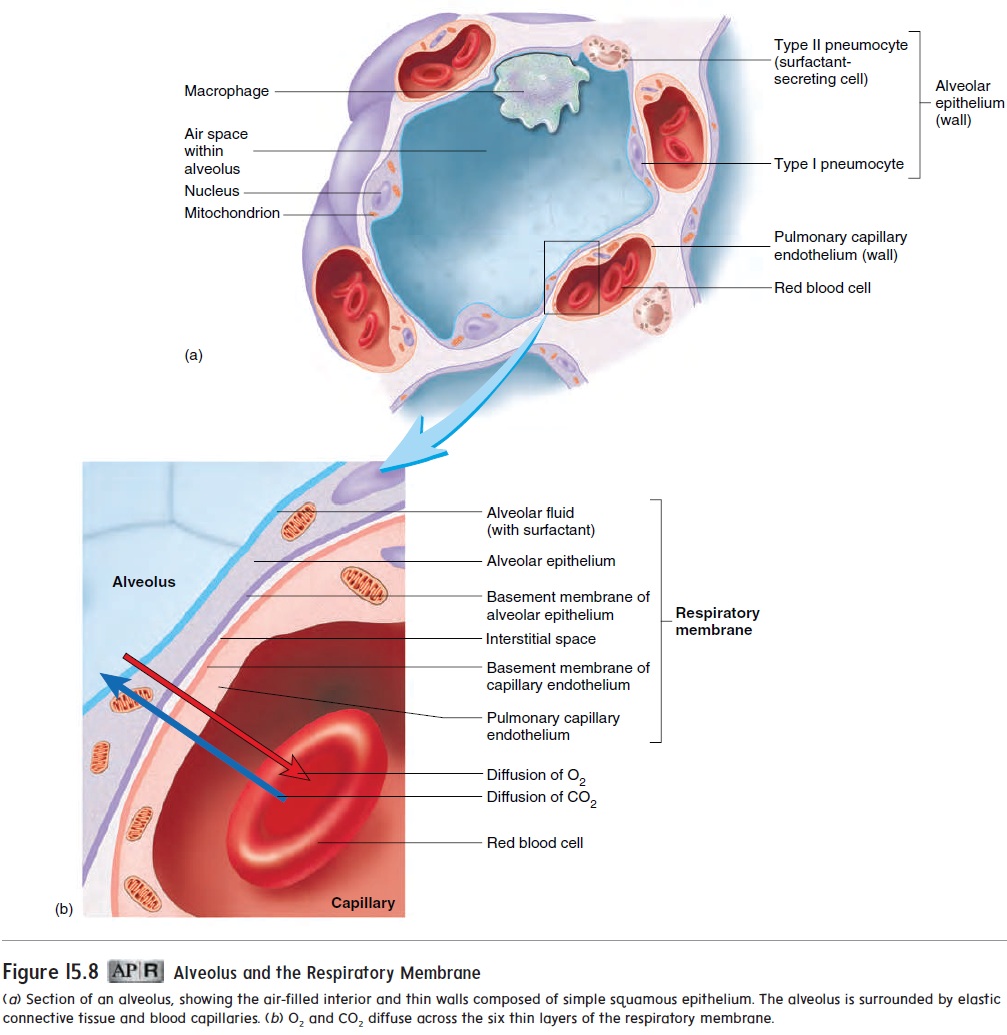
The elastic fibers surrounding the alveoli (figure 15.8) allow them to expand during inspiration and recoil during expiration. The lungs are very elastic and, when inflated, are capable of expelling the air and returning to their original, uninflated state. Specialized secretory cells within the walls of the alveoli (figure 15.8) secrete a chemical, called surfactant, that reduces the tendency of alveoli to recoil (see “Lung Recoil” later).
Pleural Cavities
The lungs are contained within the thoracic cavity. In addition, each lung is surrounded by a separate pleural (ploor′ ăl; relating to the ribs) cavity. Each pleural cavity is lined with a serous membrane called the pleura. The pleura consists of a parietal and a visceral part. The parietal pleura, which lines the walls of the thorax, dia-phragm, and mediastinum, is continuous with the visceral pleura, which covers the surface of the lung (figure 15.9; see figure 15.5).
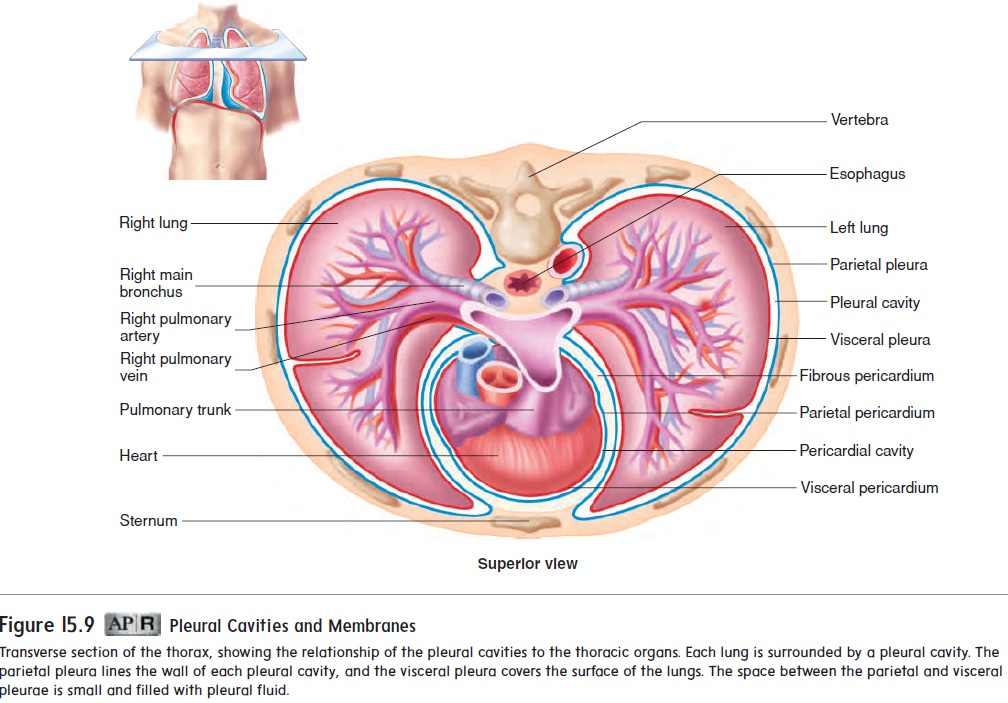
The pleural cavity, between the parietal and visceral pleurae, is filled with a small volume of pleural fluid produced by the pleural membranes. The pleural fluid performs two functions:
(1) It acts as a lubricant, allowing the visceral and parietal pleurae to slide past each other as the lungs and thorax change shape during respiration, and (2) it helps hold the pleural membranes together. The pleural fluid acts similarly to a thin film of water between two sheets of glass (the visceral and parietal pleurae); the glass sheets can slide over each other easily, but it is difficult to separate them
Lymphatic Supply
The lungs have two lymphatic supplies (see figure 15.7). The superficial lymphatic vessels are deep to the visceral pleura; theydrain lymph from the superficial lung tissue and the visceral pleura. The deep lymphatic vessels follow the bronchi; they drain lymph from the bronchi and associated connective tissues. No lymphatic vessels are located in the walls of the alveoli. Both the superficial and deep lymphatic vessels exit the lungs at the main bronchi.
Phagocytic cells within the lungs phagocytize most carbon particles and other debris from inspired air and move them to the lymphatic vessels. In older people, the surface of the lungs can appear gray to black because of the accumulation of these particles, especially if the person smoked or lived primarily in a city with air pollution. Other materials, such as cancer cells from the lungs, can also spread to other parts of the body through the lymphatic vessels
Related Topics