Chapter: Clinical Dermatology: Regional dermatology
Lichen sclerosus
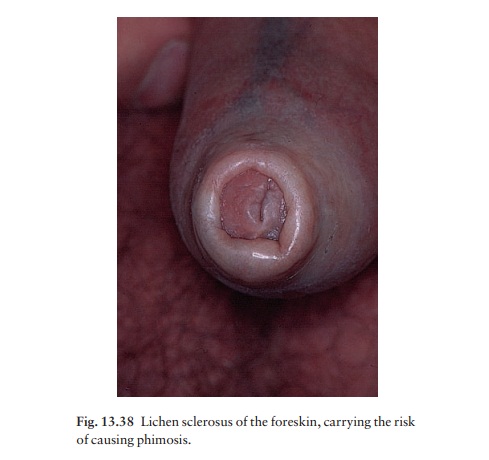
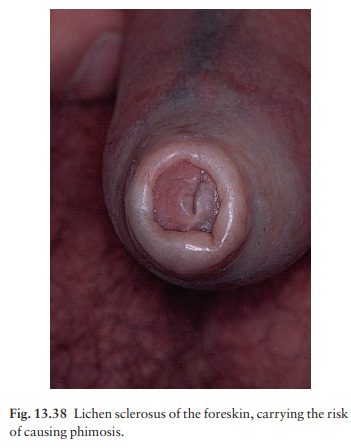
Lichen sclerosus
Cause
This
is unknown but local conditions have a role: not only does skin develop the
disease after being transplanted into affected areas, but the disease goes away
when the grafted skin is returned to a distant site.
Presentation
The affected areas on the vulva, penis (Fig. 13.38), perineum and/or perianal skin show well-marginated white thin fragile patches with a crinkled surface. Itching can be severe, especially in women. The fragil-ity of the atrophic areas may lead to purpura and erosions. Scratching can cause lichenification, and diagnostic confusion.
Women
are more commonly afflicted than men, but pre-adolescent girls and boys also
can develop this problem. In girls, the white patches circling the vulva and
anus take on an hourglass shape around the orifices.
Course
As
time goes on, scarring occurs. In adult women, the clitoral prepuce may scar
over the clitoris, and the vaginal introitus may narrow, preventing enjoyable
sexual intercourse. Scarring is rare in girls and boys; treatment may prevent
it occurring in adults.
Differential diagnosis
The
sharply marginated white patches of vitiligo can afflict the vulva and penis
but lack atrophy, and typical vitiligo may be found elsewhere on the body.
Neurodermatitis may be superimposed upon lichen sclerosus after incessant
scratching.
Investigations
Biopsy
is often unnecessary but the appearances are distinctive. The epidermis is
thin, the basal layer shows damage, and the papillary dermis contains a
homo-geneous pink-staining material and lymphocytes.
Treatment
At
first sight it might seem unwise to rub potent topical steroids onto atrophic
thin occluded skin. Yet, treatment with potent topical steroids not only
reduces itch, pain and misery, but also reverses hypo-pigmentation and atrophy
by shutting down its cause. However, atrophy, striae and other complications
can develop on untreated adjacent skin, if the medication spreads there.
Ointments are preferable to creams. Only small amounts (15 g) should be
dispensed. After a course of 8–12 weeks, weaker topical steroids can be used to
maintain a remission.
Complications
As
mentioned earlier, scarring can destroy anatomical structures and narrow the
vaginal opening. Squamous cell carcinomas may develop in men as well as women.
Any focal thickening needs a biopsy.
Related Topics