Chapter: Human Nervous System and Sensory Organs : Telencephalon
Imaging Procedures of Brain Telencephalon
Imaging Procedures
The development of imaging methods for clinical diagnostics has been extremely rapid during the last 20 years. The currently most important methods for visualizing the central nervous system are:
! Contrast medium-assisted projection radi-ography for the visualization of bloodvessels and the ventricular system
! Computed tomography (CT)
! Magnetic resonance imaging (MRI)
Conventional radiography is mainly used for the visualization of bony structures. Ul- trasound is not suitable for the central nervous system because sonic waves do no penetrate the cranial bones in adults. However,examination by ultrasound doe play a major role in diagnostics during early childhood. In addition to purely anatomical imaging methods, there is also the possi- bility of visualizing functional parameters following the injection of a suitable radioac- tive nuclide. The methods of nuclear medi- cine—single-photon emission computed to- mography (SPECT) and positron emission to- mography (PET) - can be used for studying cerebral blood flow and metabolic activity as well as for mapping specific re- ceptor systems. In the following section,some areas of application are briefly de- scribed for the most important procedures.
Contrast Radiography (A)
Radiation emitted by an X-ray source pene- trates the body.Absorbing structures (mainly the bones) appear as silhouettes on the recording screen. The screen consists either of a light-sensitive film or, to an in- creasing extent, of digital receiver arrange-with contrast medium. The contrast me-dium is usually administered to a selected vessel by introducing a catheter into the vascular system of interest. The result is a selective high-resolution image of the corresponding vascular segments (A). However, intra-arterial digital subtraction angiography (DSA) subjects the patient to considerable stress due to the introduction of the arterial catheter. Intravenous DSA, where contrast medium is injected into a brachial vein, produces images of lower contrast because the contrast medium is di-luted by the blood volume; furthermore, it results in nonspecific coloration of the ves-sels. Hence, it has not yet gained acceptance in the practice.
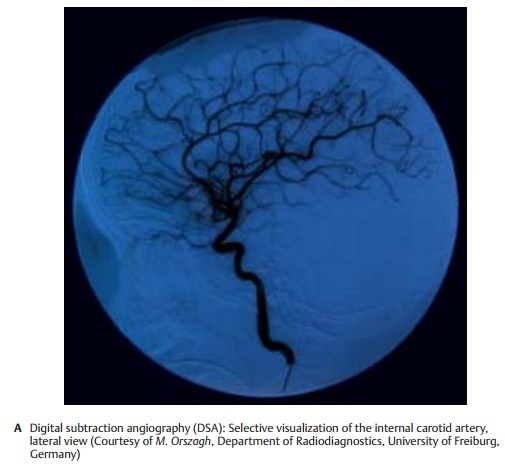
The same recording principle is used for myelography, in which contrast medium is administered directly into the cerebrospinal fluid following puncture of the lumbar spine.
Computed Tomography (B)
Computed tomography (CT), or computed axial tomography (CAT), also produces im- ages by means of X-rays. However, the im- aging principle is not based on the creation of silhouettes as in the projection method. Rather, individual transmissions through a thin layer of tissue (“slice”) defined by the geometry of the X-ray are recorded. After obtaining the absorption profiles at differ- ent projection angles (in Figure B shown as red, green, and blue areas), a two-dimen- sional image of the slice penetrated by the X-rays is computed by means of the filtered back projection. Only digital photocells of very high sensitivity are used as detectors. These allow the detection of even soft tissue structures with great sensitivity and preci sion, in addition to bony structures.
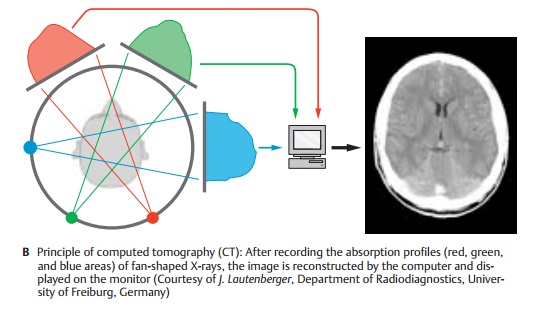
The main area of CT application for the CNS is above all the examination of patients with head trauma: apart from high-precision im-aging of bony displacements, CT is also very sensitive for the visualization of hemor-rhages. Furthermore, all types of space-oc-cupying processes can be examined by means of CT because of the highly detailed precision of the anatomical imaging. However, these areas of application are now shifting increasingly to magnetic resonance imaging owing to its higher sensitivity.
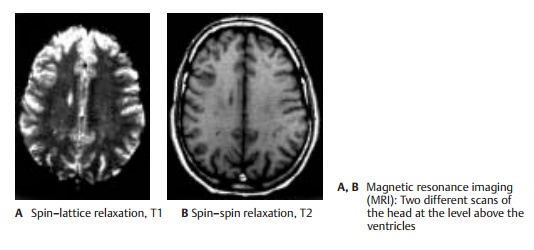
Magnetic Resonance Imaging (A, B)
Magnetic resonance imaging (MRI) is based on the magnetic properties of the atomic nuclei in the body (mainly hydrogen nuclei) and uses radiofrequency resonance tech-nique to measure the magnetic moment in-duced by an external magnetic field. Varia-tions imposed on the magnetic field allow spatial visualization of the T1 and T2 relaxa-tion times, which are nuclear magnetic properties governed by the chemical form of the hydrogen atoms containing the nuclei in the tissues. These relaxation times, which mainly reflect the ratio of free to bound water molecules, produce a contrast mecha-nism that delineates not only different tis-sues but also pathological tissue changes. The images in A and B display the same ana-tomic section and illustrate the exquisite contrast achievable by MRI, which makes it an excellent method for the identification ofpathological processes. The static magneticand electromagnetic fields used with MRI have not been found to be hazardous to patients. Furthermore, MRI has the advan-tage over CT that the images can be recon-structed in any plane. The spatial resolution of MRI is in the range of 0.7 – 1.0 mm for a section thickness of 5 mm. It takes several minutes to acquire and process the data for the axial, coronal, and sagittal sections con-stituting a standard cranial MRI.
PET and SPECT (C, D)
Both of these imaging methods of nuclear medicine are based on detecting the radiation of radioactive nuclides administered prior to the investigation.Single-photonemission computed tomography (SPECT)uses gamma-emitters. Detection of the generated radiation is carried out by means of photocells in a similar way as in CT. The geometry of the detected radiation, however, is not predetermined by the arrangement of transmitter and receiver; in-stead, both intensity and direction of the received gamma rays must be determined. This yields a spatial resolution of about 1 cm, clearly less favorable than when using computed tomography. Hence, highresolution anatomical images cannot be obtained; nevertheless, SPECT is suitable for the deter-mination of cerebral blood flow by means oftimeresolved kinetics of the detected signals.
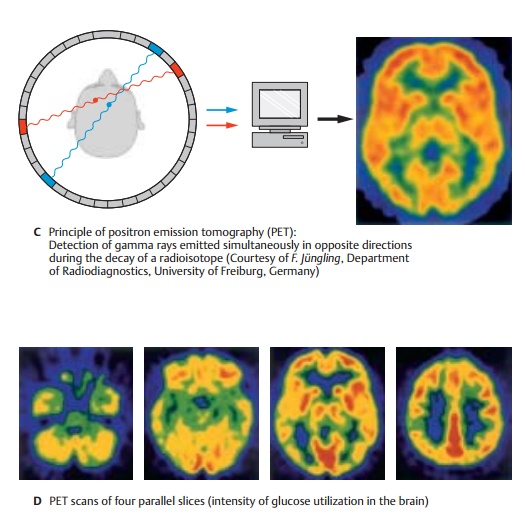
Positron emission tomography (PET) usesemitters of beta particles (positrons). The positrons almost instantly combine with electrons in the immediate surrounding, with both particles undergoing mutual annihilation and giving rise to two gamma rays of 511 keV energy emitted in opposite directions (C). The geometry of these gamma rays can be much better defined than in the case of SPECT, namely, by rec-ording the coincidence of the two gamma photons received in the detector ring. Therefore, the spatial resolution of PET lies at 2 – 4 mm, though this is clearly still not as good as in the case of CT and MRI. Through incorporation of suitable radioisotopes into biologically active molecules, PET also al-lows us to carry outmetabolic studies in ad-dition to measurements of blood flow (D), or to selectively visualize receptor systems (for example, dopamine receptors).
Related Topics