Chapter: 11th 12th std standard Home Science Maintain Basic Knowledge for family life Higher secondary school College
Formation of Urine
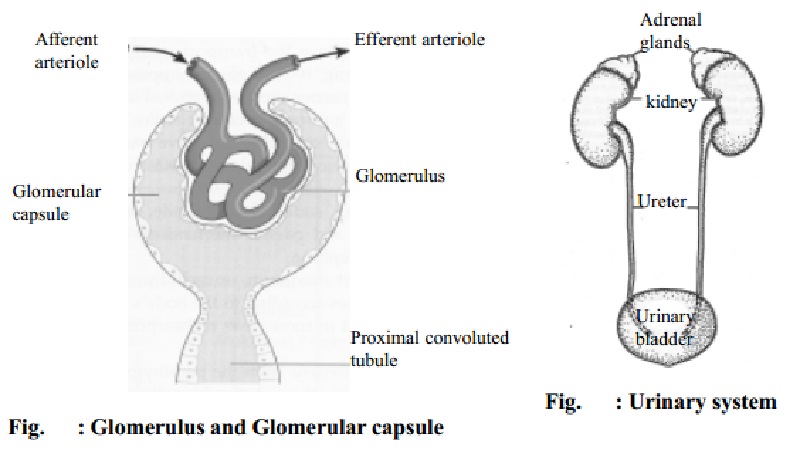
Formation of Urine
There are 3 phases to urine formation:
Simple filtration
Selective reabsorption
Secretion
Simple Filtration
Filtration takes place through the semipermeable walls of the glomerulus and glomerular capsule. Water and a large number of small molecules pass through. Blood cells, and plasma proteins are unable to filter through and remain in the capillaries. Difference between the blood pressure in the glomerulus and the pressure of the filtrate in the glomerular capsule helps in filtration. The volume of filtrate formed by both the kidneys each minute is called glomerular filtration rate (GFR). In a healthy adult the GFR is about 125 ml / min. Each day 180 litres of dilute filtrate is formed by the two kidneys. Most of this is reabsorbed and only 1 to 1.5 litres is excreted as urine.
Selective reabsorption
The glomerular filtrate passes further to the proximal convoluted tubule, loop of Henle, the distal convoluted tubule and the collecting tubules. Selective reabsorption is the process by which substances such as glucose, amino acids, sodium, calcium, potassium, phosphate and chloride are reabsorbed. This is mainly done to maintain the fluid and electrolyte balance of the blood. About 80% of reabsorption takes place in the proximal tubules and the rest is absorbed in the distal tubules, and sent back to the blood stream. Reabsorption of water is done with the help of anti diuretic hormone (ADH) which is secreted by the posterior pituitary gland. It acts by increasing the permeability of the distal convoluted tubules and collecting tubules. Substances that are not normal blood constituents are not reabsorbed. The final urine is devoid of glucose, amino acids, certain salts (phosphates and sodium) and has a very high urea concentration.
Secretion
Substances not required and foreign materials, for example drugs such as pencillin and aspirin are not cleared by filtration due to the short time it remains in the glomerulus. Such substances are cleared by secretion into the convoluted tubules and excreted from the body in the urine. Tubular secretion of H+ ions is important in maintaining homeostasis of blood pH.
The urine thus formed collects into the bladder through the ureters which are long, slender, muscular tubes that extend from the kidney to the lower part of the urinary bladder.
Micturition
The bladder is a muscular bag which collects the urine and voids it at intervals through the urethra. When the bladder is empty, the muscular wall becomes thick and the entire organ feels firm.
As the organ fills, the muscular wall becomes thinner and the organ may increase from a length of 2 or 3 inches to 5 inches or more inches. A moderately full bladder holds about 800 ml of urine. When 400 ml of urine is collected in the bladder, the normal desire for micturition is felt. The process of expelling urine through the urethra is called urination or micturition. The act of micturition is a reflex action. It is controlled by the action of circular muscles, continuous with those in the walls of the bladder and in the urethra.
Related Topics