Chapter: Medical Surgical Nursing: Vascular Disorders and Problems of Peripheral Circulation
Chronic Venous Insufficiency
CHRONIC
VENOUS INSUFFICIENCY
Venous insufficiency results from obstruction of the venous valves in the legs or a reflux of blood back through the valves. Superficial and deep leg veins can be involved. Resultant venous hypertension can occur whenever there has been a prolonged in-crease in venous pressure, such as occurs with deep venous throm-bosis.
Because the walls of veins are thinner and more elastic than the
walls of arteries, they distend readily when venous pressure is consistently
elevated. In this state, leaflets of the venous valves are stretched and
prevented from closing completely, allowing a backflow or reflux of blood in
the veins. Duplex ultrasonography confirms the obstruction and identifies the
level of valvular incompetence.
Clinical Manifestations
When
the valves in the deep veins become incompetent after a thrombus has formed,
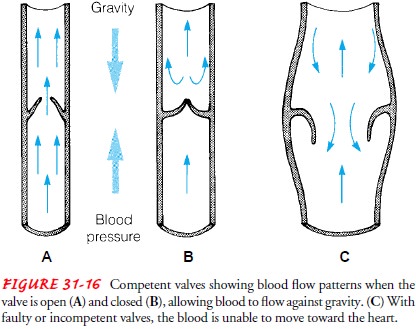
postthrombotic syndrome may develop (Fig. 31-16). This disorder is
characterized by chronic venous sta-sis, resulting in edema, altered
pigmentation, pain, and stasis der-matitis. The patient may notice the symptoms
less in the morning and more in the evening. Obstruction or poor calf muscle
pump-ing in addition to valvular reflux must be present for the develop-ment of
severe postthrombotic syndrome, which includes stasis ulceration (Caps et al.,
1999). Superficial veins may be dilated. The disorder is long-standing,
difficult to treat, and often disabling.
Stasis
ulcers develop as a result of the rupture of small skin veins and subsequent
ulcerations. When these vessels rupture, red blood cells escape into
surrounding tissues and then degenerate, leaving a brownish discoloration of
the tissues. The pigmentation and ulcerations usually occur in the lower part
of the extremity, in the area of the medial malleolus of the ankle. The skin
becomes dry, cracks, and itches; subcutaneous tissues fibrose and atrophy. The
risk of injury and infection of the extremities is increased.
Complications
Venous
ulceration is the most serious complication of chronic ve-nous insufficiency
and can be associated with other conditions affecting the circulation of the
lower extremities. Cellulitis or der-matitis may complicate the care of chronic
venous insufficiency and venous ulcerations.
Management
Management of the patient with venous insufficiency is directed at reducing venous stasis and preventing ulcerations. Measures that increase venous blood flow are antigravity activities, such as elevating the leg, and compression of superficial veins with elastic compression stockings.
Elevating
the legs decreases edema, promotes venous return, and provides symptomatic
relief. The legs should be elevated frequently throughout the day (at least 15
to 30 minutes every 2 hours). At night, the patient should sleep with the foot
of the bed elevated about 15 cm (6 inches). Prolonged sitting or standing still
is detrimental; walking should be encouraged. When sitting, the patient should
avoid placing pressure on the popliteal spaces, as occurs when crossing the
legs or sitting with the legs dangling over the side of the bed. Constricting
garments such as panty girdles or tight socks should be avoided.
Compression
of the legs with elastic compression stockings re-duces the pooling of venous
blood and enhances venous return to the heart. Elastic compression stockings
are recommended for people with venous insufficiency. The stocking should fit
so that pressure is greater at the foot and ankle and then gradually de-clines
to a lesser pressure at the knee or groin. If the top of the stocking is too
tight or becomes twisted, a tourniquet effect is cre-ated, which worsens venous
pooling. Stockings should be applied after the legs have been elevated for a
period, when the amount of blood in the leg veins is at its lowest.
Extremities
with venous insufficiency must be carefully pro-tected from trauma; the skin is
kept clean, dry, and soft. Signs of ulceration are immediately reported to the
health care provider for treatment and follow-up.
Related Topics