Chapter: Medical Surgical Nursing: Management of Patients With Neurologic Dysfunction
Headache
Headache
Headache, or cephalgia, is one of the most common
of all human physical complaints. Headache is actually a symptom rather than a
disease entity; it may indicate organic disease (neurologic or other disease),
a stress response, vasodilation (migraine), skeletal muscle tension (tension
headache), or a combination of factors. A primaryheadache
is one for which no organic cause can be identified.These types of headache
include migraine, tension-type, and clus-ter headaches (Lin, 2001). Cranial
arteritis is another common cause of headache. A classification of headaches
was issued by the Headache Classification Committee of the International
Headache Society in 1988; an abbreviated list is shown in Chart 61-6.
Migraine is
a symptom complex characterized by periodicand recurrent attacks of severe
headache. The cause of migraine has not been clearly demonstrated, but it is
primarily a vascular disturbance that occurs more commonly in women and has a
strong familial tendency. The typical time of onset is puberty, and the
incidence is highest in adults 20 to 35 years of age. There are seven subtypes
of migraine, including migraine with and without aura. Most patients have
migraine without an aura.
Tension
headaches tend to be more chronic
than severe and areprobably the most common type of headache. Cluster headaches are a severe form of
vascular headache. They are seen five times more frequently in men than women
(Greenberg, 2001).
Inflammation of the cranial arteries is
characterized by a severe headache localized in the region of the temporal
arteries. The in-flammation may be generalized (in which cranial arteritis is
part of a vascular disease) or focal (in which only the cranial arteries are
involved). Cranial arteritis is a
cause of headache in the older population, reaching its greatest incidence in
those older than 70 years of age.
A secondary
headache is a symptom associated with an or-ganic cause, such as a brain
tumor or an aneurysm. Most headaches do not indicate serious disease, although
persistent headaches re-quire further investigation. Serious disorders related
to headache include brain tumors, subarachnoid hemorrhage, stroke, severe
hypertension, meningitis, and head injuries.
Assessment and Diagnostic Evaluation
The
diagnostic evaluation includes a detailed history, a physical assessment of the
head and neck, and a complete neurologic ex-amination. Headaches may manifest
differently within an indi-vidual over the course of a lifetime, and the same
type of headache may present differently from patient to patient. The health
his-tory focuses on assessing the headache itself, with emphasis on the factors
that precipitate or provoke it. Patients are asked to de-scribe headaches in
their own words.
Because headache is often the presenting symptom of
various physiologic and psychological disturbances, a general health his-tory
is an essential component of the patient database. Headache may be a symptom of
endocrine, hematologic, gastrointestinal, infectious, renal, cardiovascular, or
psychiatric disease. Therefore, questions addressed in the health history
should cover major medical and surgical illness as well as a body systems
review.
The medication history can provide insight into the
patient’s overall health status. Antihypertensive agents, diuretic
medica-tions, anti-inflammatory agents, and monoamine oxidase in-hibitors are a
few of the categories of medications that can provoke headaches. Although
sometimes exaggerated in importance, emo-tional factors can play a role in
precipitating headaches. Stress is thought to be a major initiating factor in migraine
headaches; therefore, sleep patterns, level of stress, recreational interests, appetite,
emotional problems, and family stressors are relevant (Cunningham, 2000). There
is a strong familial tendency for headache disorders, and a positive family
history may help in making a diagnosis.
A
direct relationship may exist between exposure to toxic sub-stances and
headache. Careful questioning may uncover chem-icals to which a worker has been
exposed. Under the Right to Know law, employees have access to the material
safety data sheets (commonly referred to as MSDSs) for all the substances with
which they come in contact in the workplace. The occupa-tional history also
includes assessment of the workplace as a pos-sible source of stress and a
possible ergonomic basis for muscle strain and headache.
A
complete description of the headache itself is crucial. The age at onset of
headache; the headache’s frequency, location, and duration; the type of pain;
factors that relieve and precipitate the event; and associated symptoms are
reviewed. The data obtained should include the patient’s own words about the
headache in response to the following questions:
·
What is the location? Is it
unilateral or bilateral? Does it ra-diate?
·
What is the quality—dull,
aching, steady, boring, burning, intermittent, continuous, paroxysmal?
·
How many headaches occur
during a given time?
·
What are the precipitating
factors, if any (environmental, such as sunlight and weather change; foods;
exertion; other)?
·
What makes the headache worse
(coughing, straining)?
·
What time (day or night) does
it occur?
·
Are there any associated
symptoms, such as facial pain, lacrimation (excessive tearing), or scotomas
(blind spots in the field of vision)?
·
What usually relieves the
headache (aspirin, NSAIDs, ergot preparation, food, heat, rest, neck massage)?
·
Does nausea, vomiting,
weakness, or numbness in the ex-tremities accompany the headache?
·
Does the headache interfere
with daily activities?
·
Do you have any allergies?
·
Do you have insomnia, poor appetite,
loss of energy?
·
Is there a family history of
headache?
·
What is the relationship of
the headache to lifestyle or phys-ical or emotional stress?
·
What medications are you
taking?
Diagnostic
testing is often not helpful in the investigation of headache as there are
often few objective findings. In patients who demonstrate abnormalities on the
neurologic examination, CT, cerebral angiography, or MRI may be used to detect
under-lying causes, such as tumor or aneurysm. Electromyography (EMG) may reveal
a sustained contraction of the neck, scalp, or facial muscles. Laboratory tests
may include complete blood count, erythrocyte sedimentation rate, electrolytes,
glucose, cre-atinine, and thyroid hormone levels.
Pathophysiology
The cerebral signs and symptoms of migraine result from dys-function of the
brain stem pathways that normally modulate sensory input (Goadsby, Lipton &
Ferrari, 2002). Abnormal me-tabolism of serotonin, a vasoactive
neurotransmitter found in platelets and cells of the brain, plays a major role.
The headache is preceded by a rise in plasma serotonin, which dilates the
cerebral vessels, but migraines are more than just vascular headaches. Theexact
mechanism of pain in migraine is not completely understood but is thought to be
related to the cranial blood vessels, the inner-vation of the vessels, and the
reflex connections in the brain stem.
Migraines
can be triggered by menstrual cycles, bright lights, stress, depression, sleep
deprivation, fatigue, overuse of certain medications, and certain foods
containing tyramine, monosodium glutamate, nitrites, or milk products. Foods in
these categories include aged cheese and many processed foods. Use of oral
con-traceptives may be associated with increased frequency and sever-ity of
attacks in some women.
Emotional
or physical stress may cause contraction of the muscles in the neck and scalp,
resulting in tension headache. The pathophysiology of cluster headache is not
fully understood. One theory is that it is due to dilation of orbital and nearby
extracra-nial arteries. Cranial arteritis is thought to represent an immune
vasculitis in which immune complexes are deposited within the walls of affected
blood vessels, producing vascular injury and in-flammation. A biopsy may be
performed on the involved artery to make the diagnosis.
Clinical Manifestations
MIGRAINE
The
migraine with aura can be divided into four phases: pro-drome, aura, the
headache, and recovery (headache termination and postdrome).
Prodrome.
The prodrome phase is experienced by 60% of pa-tients with symptoms that
occur hours to days before a migraine headache. Symptoms include depression,
irritability, feeling cold, food cravings, anorexia, change in activity level,
increased urina-tion, diarrhea, or constipation. Patients usually experience
the same prodrome with each migraine headache.
Aura Phase.
Aura occurs in up to 31% of patients who have
mi-graines (Goadsby et al., 2002). The aura usually lasts less than an hour and
may provide enough time for the patient to take the prescribed medication to
avert a full-blown attack (described in a later section). This period is
characterized by focal neurologic symptoms. Visual disturbances (ie, light
flashes and bright spots) are common and may be hemianopic (affecting only half
of the visual field). Other symptoms that may follow include numbness and
tingling of the lips, face, or hands; mild confusion; slight weakness of an
extremity; drowsiness; and dizziness.
This period of aura corresponds to the painless
vasoconstric-tion that is the initial physiologic change characteristic of
classic migraine. Cerebral blood flow studies performed during migraine
headaches demonstrate that during all phases of the attack, cere-bral blood
flow is reduced throughout the brain, with subsequent loss of autoregulation
and impaired CO2 responsiveness.
Headache Phase.
As vasodilation and a decline in serotonin lev-els
occur, a throbbing headache (unilateral in 60% of patients) intensifies over
several hours. This headache is severe and inca-pacitating and is often
associated with photophobia, nausea, and vomiting. Its duration varies, ranging
from 4 to 72 hours (Goadsby et al., 2002).
Recovery Phase.
In the recovery phase (termination and post-drome),
the pain gradually subsides. Muscle contraction in the neck and scalp is
common, with associated muscle ache and lo-calized tenderness, exhaustion, and
mood changes. Any physical exertion exacerbates the headache pain. During this
postheadache phase, patients may sleep for extended periods.
OTHER HEADACHE TYPES
The tension headache is characterized by a steady,
constant feel-ing of pressure that usually begins in the forehead, temple, or
back of the neck. It is often bandlike or may be described as “a weight on top
of my head.”
Cluster headaches are unilateral and come in
clusters of one to eight daily, with excruciating pain localized to the eye and
orbit and radiating to the facial and temporal regions. The pain is
accompa-nied by watering of the eye and nasal congestion. Each attack lasts 30
to 90 minutes and may have a crescendo–decrescendo pattern (Greenberg, 2001).
The headache is often described as penetrat-ing and steady.
Cranial arteritis often begins with general
manifestations, such as fatigue, malaise, weight loss, and fever. Clinical
manifestations associated with inflammation (heat, redness, swelling,
tenderness, or pain over the involved artery) usually are present. Sometimes a
tender, swollen, or nodular temporal artery is visible. Visual problems are
caused by ischemia of the involved structures.
Prevention
Prevention begins by having the patient avoid
specific triggers that are known to initiate the headache syndrome. Preventive
medical management of migraine involves the daily use of one or more agents
that are thought to block the physiologic events lead-ing to an attack.
Medication therapy should be considered for mi-graine if attacks occur 3 to 4
days per month (Goadsby et al., 2002). Treatment regimens vary greatly, as do
patient responses; thus, close monitoring is indicated.
There
are several proven or widely used medications for the prevention of migraine.
Two beta-blocking agents, propranolol (Inderal) and metoprolol (Lopressor),
inhibit the action of beta-receptors—cells in the heart and brain that control
the dilation of blood vessels. This is thought to be a major reason for their
an-timigraine action. Other medications that are prescribed for mi-graine
prevention include amitriptyline hydrochloride (Elavil), divalproex
(Valproate), flunarizine, and several serotonin antag-onists (Goadsby et al.,
2002).
Calcium
antagonists (verapamil HCl) are widely used but may require several weeks at a
therapeutic dosage before improvement is noted. Calcium-channel blockers are
not as effective as beta-blockers for prevention but may be more appropriate
for some patients, such as those with bradycardia, diabetes mellitus, or asthma
(Goadsby et al., 2002).
Alcohol,
nitrites, vasodilators, and histamines may precipitate cluster headaches.
Eliminating these factors helps in preventing the headaches (Silberstein &
Rosenberg, 2000). Prophylactic medication therapy may include beta-blockers,
ergotamine tar-trate (occasionally), lithium, naproxen (Naprosyn), and
methy-sergide (Sansert); such therapy is effective in 20% to 40% of cases
(Greenberg, 2001).
Medical Management
Therapy
for migraine headache is divided into abortive (sympto-matic) and preventive
approaches. The abortive approach, best employed in patients who suffer less
frequent attacks, is aimed at relieving or limiting a headache at the onset or
while it is in progress. The preventive approach is used in patients who
expe-rience more frequent attacks at regular or predictable intervals and may
have medical conditions that preclude the use of abortive therapies (Evans
& Lipton, 2001).
The triptans, serotonin receptor agonists, are the
most specific antimigraine agents available. These agents cause
vasoconstriction, reduce inflammation, and may reduce pain transmission. The
five triptans in routine clinical use include sumatriptan (Imitrex),
naratriptan (Amerge), rizatriptan (Maxalt), zolmitrip-tan (Zomig), and
almotriptan (Goadsby et al., 2002). Numerous serotonin receptor agonists are
under study.
Ergotamine preparations (taken orally,
sublingually, subcuta-neously, intramuscularly, by rectum, or by inhalation)
may be ef-fective in aborting the headache if taken early in the migraine
process. They are low in cost. Ergotamine tartrate acts on smooth muscle,
causing prolonged constriction of the cranial blood vessels. Each patient’s
dosage is based on individual needs. Side effects in-clude aching muscles,
paresthesias (numbness and tingling), nau-sea, and vomiting. Cafergot, a
combination of ergotamine and caffeine, can arrest or reduce the severity of
the headache if taken at the first sign of an attack (Karch, 2002).
Perhaps the most widely used triptan is sumatriptan
succinate (Imitrex); it is available in oral, intranasal, and subcutaneous
prepa-rations and is effective for the treatment of acute migraine and clus-ter
headaches in adults (McAlhany, 2001). The subcutaneous form usually relieves
symptoms within an hour and is available in an auto-injector for immediate
patient use, although it is expensive in this form. Sumatriptan has been found
to be effective in relieving mod-erate to severe migraines in a large number of
adult patients. Suma-triptan may cause chest pain and is contraindicated in
patients with ischemic heart disease (Goadsby et al., 2002). Careful
administra-tion and dosing instructions to patients are important to prevent
adverse reactions such as increased blood pressure, drowsiness, muscle pain,
sweating, and anxiety. There are possible interactions when taken in
conjunction with St. John’s wort (Karch, 2002).
Many of the triptan medications are available in a
variety of formulations, such as nasal sprays, inhalers, suppositories, or
in-jections; however, 80% of patients prefer the oral formulations (Goadsby et
al., 2002). None of these medications should be taken concurrently with
medications containing ergotamine due to the potential for a prolonged
vasoactive reaction (Karch, 2002).
The
medical management of an acute attack of cluster head-aches may include 100%
oxygen by face mask for 15 minutes, ergotamine tartrate, sumatriptan, steroids,
or a percutaneous sphenopalatine ganglion blockade (Greenberg, 2001).
The
medical management of cranial arteritis consists of early administration of a
corticosteroid to prevent the possibility of loss of vision due to vascular
occlusion or rupture of the involved artery (Greenberg, 2001). The patient is instructed not to stop the medication abruptly
because this can lead to relapse. Anal-gesic agents are prescribed for comfort.
Nursing Management
When migraine or the other types of headaches
described above have been diagnosed, the goals of nursing management are to
en-hance pain relief. It is reasonable to try nonpharmacologic inter-ventions
first, but the use of pharmacologic agents should not be delayed. The goal is
to treat the acute event of the headache and to prevent recurrent episodes.
Prevention involves patient educa-tion regarding precipitating factors,
possible lifestyle or habit changes that may be helpful, and pharmacologic
measures.
RELIEVING PAIN
Individualized treatment depends on the type of headache and differs for migraine, cluster headaches, cranial arteritis, and ten-sion headache (Greenberg, 2001; Silberstein & Rosenberg, 2000). Nursing care is directed toward treatment of the acute episode.
A migraine or a cluster headache in the early phase requires abortive
medication therapy instituted as soon as possible. Some headaches may be
prevented if the appropriate medications are taken before the onset of pain.
Nursing care during a fully devel-oped attack includes comfort measures such as
a quiet, dark en-vironment and elevation of the head of the bed to 30 degrees.
In addition, symptomatic treatment such as antiemetics may be in-dicated
(Goadsby et al., 2002).
Symptomatic
pain relief for tension headache may be obtained by application of local heat
or massage. Additional strategies may include the use of analgesic agents,
antidepressant medications, and muscle relaxants.
HOME AND COMMUNITY-BASED CARE
Teaching Patients Self-Care.
Headaches, especially migraines,are more likely to
occur when the patient is ill, overly tired, or stressed. Nonpharmacologic
therapies are important and include patient education about the type of
headache, its mechanism (if known), and appropriate changes in lifestyle to
avoid triggers. Regular sleep, meals, exercise, avoidance of peaks and troughs
of relaxation, and avoidance of dietary triggers may be helpful in avoiding
headaches (Goadsby et al., 2002; Rice, 2000).
The patient with tension headaches needs teaching
and reas-surance that the headache is not due to a brain tumor. This is a
common unspoken fear. Stress reduction techniques, such as biofeedback,
exercise programs, and meditation, are examples of nonpharmacologic therapies
that may prove helpful. Patients and their families need to be reminded of the
importance of follow-ing the prescribed treatment regimen for headache and
keeping follow-up appointments. In addition, they are reminded of the
importance of participating in health promotion activities and recommended
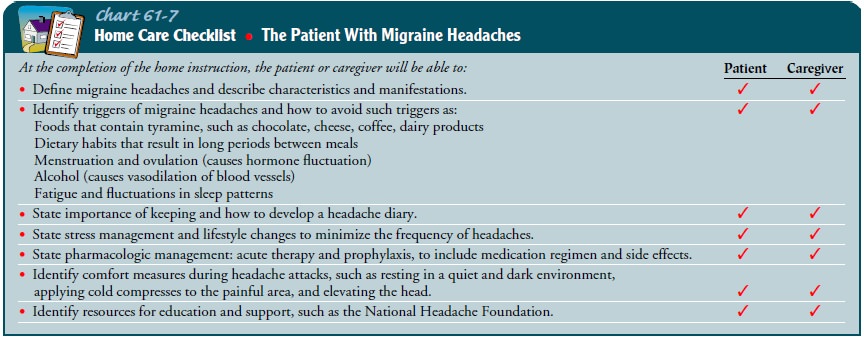
health screenings to promote a healthy lifestyle. See Chart 61-7 for a home
care checklist for the patient with mi-graine headaches.
Continuing Care.
The National Headache Foundation provides a list of clinics in the United
States and the names of physicians who specialize in headache and who are members
of the American Association for the Study of Headache.
Related Topics