Chapter: Clinical Anesthesiology: Regional Anesthesia & Pain Management: Spinal, Epidural & Caudal Blocks
Epidural Needles and Epidural Catheters
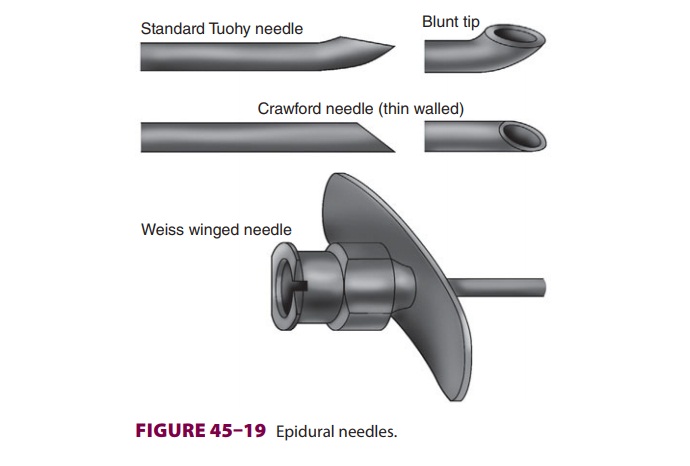
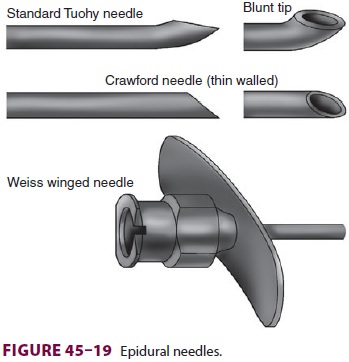
Epidural Needles
The standard epidural needle is typically
17–18 gauge, 3 or 3.5 inches long, and has a blunt bevel with a gentle curve of
15–30° at the tip. The Tuohy
needle is most commonly used (Figure 45–19).
The blunt, curved tip theoretically helps to push away the dura after passing
through the ligamentum flavum instead of penetrating it. Straight needles
without a curved tip (Crawford needles) may have a greater incidence of dural
puncture, but facilitate passage of an epidural catheter. Needle modifications
include winged tips and introducer devices set into the hub designed for
guiding catheter placement.
Epidural Catheters
Placing a catheter into the epidural space allows for continuous
infusion or intermittent bolus tech-niques. In addition to extending the
duration of the block, it may allow a lower total dose of anesthetic to be
used.
Epidural catheters are useful for intraoperative epidural anesthesia and/or postoperative analgesia. Typically, a 19- or 20-gauge catheter is introduced through a 17- or 18-gauge epidural needle. When using a curved tipped needle, the bevel opening is directed either cephalad or caudad, and the cath-eter is advanced 2–6 cm into the epidural space. The shorter the distance the catheter is advanced, the more likely it is to become dislodged. Conversely, the further the catheter is advanced, the greater the chance of a unilateral block, due to the catheter tip either exiting the epidural space via an intervertebral foramen or coursing into the anterolateral recesses of the epidural space. After advancing the catheter the desired depth, the needle is removed, leaving the catheter in place. The catheter can be taped or otherwise secured along the back. Catheters that will remain in place for prolonged times (eg, >1 wk) may be tunneled under the skin. Catheters have either a single port at the distal end or multiple side ports close to a closed tip. Some have a stylet for easier insertion. Spiral wire-reinforced catheters are very resistant to kinking. The spiral or spring tip is asso-ciated with fewer, less intense paresthesias and may be associated with a lower incidence of inadvertent intravascular insertion.
Related Topics