Chapter: Basic & Clinical Pharmacology : Opioid Analgesics & Antagonists
The Opioid Antagonists
THE OPIOID ANTAGONISTS
The pure opioid
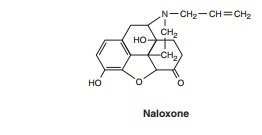
antagonist drugs naloxone, naltrexone,
and nalmefene are morphine
derivatives with bulkier substituents atthe N17 position. These agents have a relatively high
affinity for μ-opioid
binding sites. They have lower affinity for the otherreceptors but can also
reverse agonists at δ
and κ
sites.
Pharmacokinetics
Naloxone is usually
given by injection and has a short duration of action (1–2 hours) when given by
this route. Metabolic dis-position is chiefly by glucuronide conjugation like
that of the agonist opioids with free hydroxyl groups. Naltrexone is well
absorbed after oral administration but may undergo rapid first-pass metabolism.
It has a half-life of 10 hours, and a single oral dose of 100 mg blocks the
effects of injected heroin for up to 48 hours. Nalmefene, the newest of these
agents, is a derivative of naltrexone but is available only for intravenous
administration. Like naloxone, nalmefene is used for opioid overdose but has a
longer half-life (8–10 hours).
Pharmacodynamics
When given in the
absence of an agonist drug, these antagonists are almost inert at doses that
produce marked antagonism of ago-nist opioid effects.
When given intravenously
to a morphine-treated subject, the antagonist completely and dramatically
reverses the opioid effects within 1–3 minutes. In individuals who are acutely
depressed by an overdose of an opioid, the antagonist effectively normalizes
respiration, level of consciousness, pupil size, bowel activity, and awareness
of pain. In dependent subjects who appear normal while taking opioids, naloxone
or naltrexone almost instanta-neously precipitates an abstinence syndrome.
There is no tolerance
to the antagonistic action of these agents, nor does withdrawal after chronic
administration precipitate an abstinence syndrome.
Clinical Use
Naloxone is a pure
antagonist and is preferred over older weak agonist-antagonist agents that had
been used primarily as antago-nists, eg, nalorphine and levallorphan.
The major application
of naloxone is in the treatment of acute opioid overdose. It is
very important that therepeated whenever necessary. In using naloxone in
the severely opioid-depressed newborn, it is important to start with doses of
5–10 mcg/kg and to consider a second dose of up to a total of 25 mcg/kg if no
response is noted.
Low-dose naloxone
(0.04 mg) has an increasing role in the treatment of adverse effects that are
commonly associated with intravenous or epidural opioids. Careful titration of
the naloxone dosage can often eliminate the itching, nausea, and vomiting while
sparing the analgesia. For this purpose, oral naloxone, and more recently
modified analogs of naloxone and naltrexone, have been approved by the FDA.
These include methylnaltrexonebromide (Relistor)
for the treatment of constipation in patientswith late-stage advanced illness
and alvimopan (Entereg) for the
treatment of postoperative ileus following bowel resection surgery. The
principal mechanism for this selective therapeutic effect is believed to be
inhibition of peripheral μ receptors in the gut with minimal CNS
penetration.
Because of its long
duration of action, naltrexone has been proposed as a maintenance drug for
addicts in treatment pro-grams. A single dose given on alternate days blocks
virtually all of the effects of a dose of heroin. It might be predicted that
this approach to rehabilitation would not be popular with a large per-centage
of drug users unless they are motivated to become drug-free. A related use is
in combination with morphine sulfate in a controlled-release formulation
(Embeda) in which 20–100 mg of morphine is slowly released over 8–12 hours or
longer for the control of prolonged postoperative pain. Naltrexone, 0.4–4 mg,
is sequestered in the center of the formulation pellets and is present to
prevent the abuse of the morphine (by grinding and extraction of the morphine
from the capsules).
There is evidence that naltrexone decreases
the craving for alcohol in chronic alcoholics by increasing baseline β-endorphin release,
and it has been approved by the FDA for this purpose . Naltrexone also
facilitates abstinence from nicotine (cigarette smoking) with reduced weight
gain. In fact, a combina-tion of naltrexone plus bupropion may also offer an
effective and synergistic strategy for weight loss. If current trials
demonstrate cardiovascular safety during prolonged use, this and other
weight-loss medications compounded with naltrexone may eventually win FDA
approval.
Related Topics