Chapter: Basic & Clinical Pharmacology : Opioid Analgesics & Antagonists
Clinical Use of Opioid Analgesics
Clinical Use of Opioid Analgesics
A. Analgesia
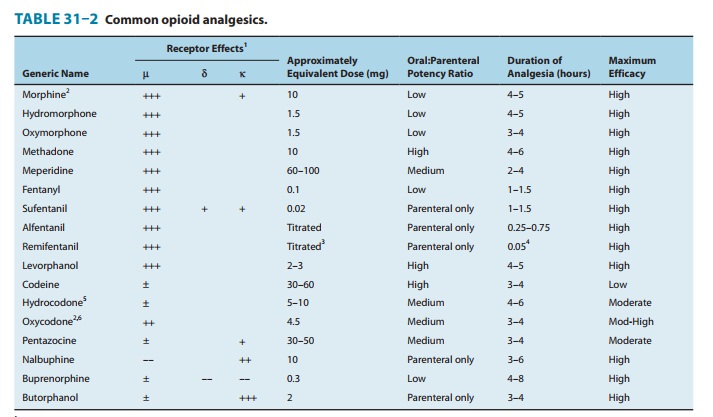
Severe, constant pain is usually relieved with
opioid analgesics with high intrinsic activity (see Table 31–2), whereas sharp,
intermit-tent pain does not appear to be as effectively controlled.
The pain associated
with cancer and other terminal illnesses must be treated aggressively and often
requires a multidisciplinary approach for effective management. Such conditions
may require continuous use of potent opioid analgesics and are associated with
some degree of tolerance and dependence. However,
this should notbe used as a barrier to providing patients with the best
possible care and quality of life. Research in the hospice movement has
demon-strated that fixed-interval administration of opioid medication (ie, a
regular dose at a scheduled time) is more effective in achieving pain relief
than dosing on demand. New dosage forms of opioids that allow slower release of
the drug are now available, eg, sus-tained-release forms of morphine (MS
Contin) and oxycodone (OxyContin). Their purported advantage is a longer and
more stable level of analgesia.
If disturbances of
gastrointestinal function prevent the use of oral sustained-release morphine,
the fentanyl transdermal system (fentanyl patch) can be used over long periods.
Furthermore, buc-cal transmucosal fentanyl can be used for short episodes of
break-through pain (see Alternative Routes of Administration). Administration
of strong opioids by nasal insufflation has been shown to be efficacious, and
nasal preparations are now available in some countries. Approval of such
formulations in the USA is grow-ing. In addition, stimulant drugs such as the
amphetamines have been shown to enhance the analgesic actions of the opioids
and thus may be very useful adjuncts in the patient with chronic pain.
Opioid analgesics are
often used during obstetric labor. Because opioids cross the placental barrier
and reach the fetus, care must be taken to minimize neonatal depression. If it
occurs, immediate injec-tion of the antagonist naloxone will reverse the
depression. The phenylpiperidine drugs (eg, meperidine) appear to produce less
depression, particularly respiratory depression, in newborn infants than does
morphine; this may justify their use in obstetric practice.
The acute, severe pain
of renal and biliary colic often requires a strong agonist opioid for adequate
relief. However, the drug-induced increase in smooth muscle tone may cause a
paradoxical increase in pain
secondary to increased spasm. An increase in the dose of opioid is usually
successful in providing adequate analgesia.
B. Acute Pulmonary Edema
The relief produced by
intravenous morphine in dyspnea from pulmonary edema associated with left
ventricular heart failure is remarkable. Proposed mechanisms include reduced
anxiety (per-ception of shortness of
breath) and reduced cardiac preload(reduced venous tone) and afterload
(decreased peripheral resis-tance). However, if respiratory depression is a
problem, furosemide may be preferred for the treatment of pulmonary edema. On
the other hand, morphine can be particularly useful when treating painful
myocardial ischemia with pulmonary edema.
C. Cough
Suppression of cough
can be obtained at doses lower than those needed for analgesia. However, in
recent years the use of opioid analgesics to allay cough has diminished largely
because a number of effective synthetic compounds have been developed that are
neither analgesic nor addictive. These agents are discussed below.
D. Diarrhea
Diarrhea from almost
any cause can be controlled with the opioid analgesics, but if diarrhea is
associated with infection such use must not substitute for appropriate
chemotherapy. Crude opium preparations (eg, paregoric) were used in the past to
control diar-rhea, but now synthetic surrogates with more selective gastrointes-tinal
effects and few or no CNS effects, eg, diphenoxylate or loperamide, are used.
Several preparations are available specifically for this purpose .
E. Shivering
Although all opioid
agonists have some propensity to reduce shiv-ering, meperidine is reported to
have the most pronounced anti-shivering properties. Meperidine apparently
blocks shivering mainly through an action on subtypes of the α2 adrenoceptor.
F. Applications in Anesthesia
The opioids are frequently used as premedicant
drugs before anes-thesia and surgery because of their sedative, anxiolytic, and
analge-sic properties. They are also used intraoperatively both as adjuncts to
other anesthetic agents and, in high doses (eg, 0.02–0.075 mg/ kg of fentanyl),
as a primary component of the anesthetic regimen . Opioids are most commonly
used in cardiovascu-lar surgery and other types of high-risk surgery in which a
primary goal is to minimize cardiovascular depression. In such situations,
mechanical respiratory assistance must be provided.
Because of their
direct action on the superficial neurons of the spinal cord dorsal horn,
opioids can also be used as regional anal-gesics by administration into the
epidural or subarachnoid spaces of the spinal column. A number of studies have
demonstrated that long-lasting analgesia with minimal adverse effects can be
achieved by epidural administration of 3–5 mg of morphine, followed by slow
infusion through a catheter placed in the epidural space. It was initially
assumed that the epidural application of opioids might selectively produce
analgesia without impairment of motor, autonomic, or sensory functions other
than pain. However, respi-ratory depression can occur after the drug is
injected into the epidural space and may require reversal with naloxone. Effects
such as pruritus and nausea and vomiting are common after epi-dural and
subarachnoid administration of opioids and may also be reversed with naloxone
if necessary. Currently, the epidural route is favored over subarachnoid
administration because adverse effects are less common and robust outcome
studies have shown a significant reduction in perioperative mortality and
morbidity with the use of thoracic epidural analgesia. The use of low doses of
local anesthetics in combination with fentanyl infused through a thoracic
epidural catheter has become an accepted method of pain control in patients
recovering from thoracic and major upper abdominal surgery. In rare cases,
chronic pain management spe-cialists may elect to surgically implant a
programmable infusion pump connected to a spinal catheter for continuous
infusion of opioids or other analgesic compounds.
G. Alternative Routes of Administration
Rectal suppositories of morphine and hydromorphone have beenused
when oral and parenteral routes are undesirable. The transder-mal patch provides stable blood levels of drug and better
pain con-trol while avoiding the need for repeated parenteral injections.
Fentanyl has been the most successful opioid in transdermal applica-tion and is
indicated for the management of persistent unremitting pain. Because of the
complication of fentanyl-induced respiratory depression, the Food and Drug
Administration (FDA) recommends that introduction of a transdermal fentanyl
patch (25 mcg/h) be reserved for patients with an established oral morphine
require-ment of at least 60 mg/d for 1 week or more. Extreme caution must be
exercised in any patient initiating therapy or undergoing a dose increase
because the peak effects may not be realized until 24–48 hours after patch
application. The intranasal route
avoids repeated parenteral drug injections and the first-pass metabolism of
orally administered drugs. Butorphanol is the only opioid cur-rently available
in the USA in a nasal formulation, but more are expected. Another alternative
to parenteral administration is the buccal
transmucosal route, which uses a fentanyl citrate lozengeor a “lollipop”
mounted on a stick.
Another type of pain
control called patient-controlled
analgesia(PCA) is now in widespread use for the management of break-through
pain. With PCA, the patient controls a parenteral (usually intravenous)
infusion device by pressing a button to deliver a pre-programmed dose of the
desired opioid analgesic. Claims of better pain control using less opioid are
supported by well-designed clinical trials, making this approach very useful in
postoperative pain control. However, health care personnel must be very
familiarwith the use of PCAs to avoid overdosage secondary to misuse or
improper programming. There is a proven risk of PCA-associated respiratory
depression and hypoxia that requires careful monitoring of vital signs and
sedation level, and provision of supplemental oxygen. This risk is increased if
patients are concurrently prescribed medications with sedative properties such
as benzodiazepines.
Related Topics