Chapter: Biology of Disease: Toxicology
Symptomatic Poisoning
SYMPTOMATIC POISONING
In the symptomatic patient, the diagnosis of poisoning is usually made on the basis of clinical findings. However, in all cases of suspected poisoning, a number of biochemical investigations should be made as shown in Table12.1. The roles of the clinical laboratory in chemical toxicology in identifyinga suspected poison in blood or urine and in monitoring vital functions cannot be overestimated.
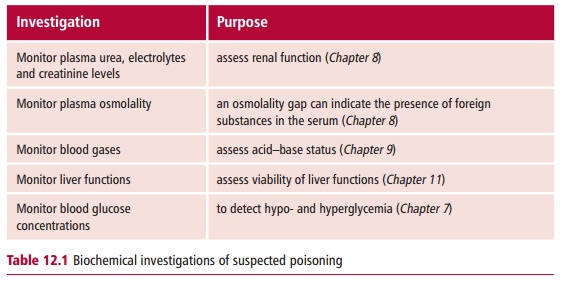
The clinical management of patients is directed towards supporting their vital functions and attempting to remove the poison from the body as rapidly as possible. Unfortunately, few of the signs or symptoms that patients present with are specific for any one type of drug or poison. Also, patients may well present in a coma and so be unable to give relevant information. A drug screen on a urine specimen may be carried out but this will only indicate that a drug has been ingested and may give no indication of the severity of the overdose.
COMMON POISONS
Humans are exposed to numerous xenobiotics, including drugs, pesticides, environmental pollutants, industrial chemicals and food additives. Any of these are potentially capable of perturbing the biochemistry and physiology of the body either directly or after being metabolically transformed. However, the most frequent poisons encountered in emergency toxicology include paracetamol (acetaminophen), aspirin, alcohols (ethanol, methanol, ethylene glycol), barbiturates (though this is now mainly historical), carbon monoxide, paraquat and several metals.
Related Topics