Chapter: Human Nervous System and Sensory Organs : Spinal Cord and Spinal Nerves
Sacral Plexus - Peripheral Nerves
Sacral Plexus
The lumbosacral trunk (parts of L4 and L5) and the anterior branches of S1 – S3 join on the anterior surface of the piriform muscle to form the sacral plexus. Direct branches extend from the plexus to the muscles of the pelvic region, namely, to the piriform muscle, the gemellus muscles (F9), the in-ternal obturator muscle, and the quadrate muscle of thigh (F10).
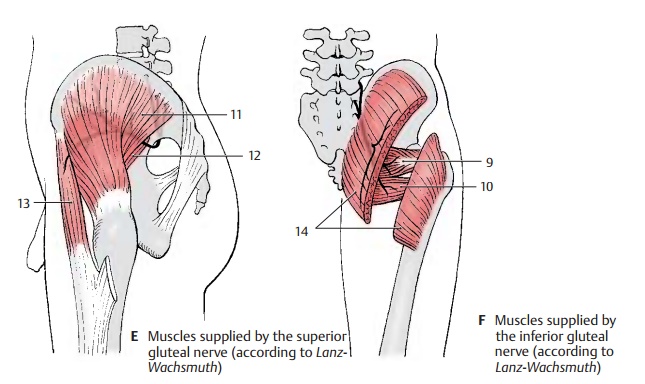
Superior Gluteus Nerve (L4 – S1) (E)
The nerve extends across the upper margin of the piriform muscle in dorsal direction through the suprapiriform foramen to the gluteus medius (E11) and minimus (E12) muscles and supplies both with motor fibers. The nerve continues between the two muscles to the tensor muscle of the fas-cia lata (E13).
Clinical Note: Paralysis of the nerve weakensabduction of the leg. Standing on the affected leg and lifting the healthy leg makes the pelvis of the other side drop (Trendelenburg’s symptom).
Inferior Gluteus Nerve (L5 – S2) (F)
The nerve leaves the pelvis through the in-frapiriform foramen and gives off several branches to the gluteus maximus muscle (F14).
Clinical Note: Paralysis of the nerve weakensextension of the hip joint (for example, when standing up or climbing stairs).
Posterior Cutaneous Nerve of Thigh (S1 – S3) (D)
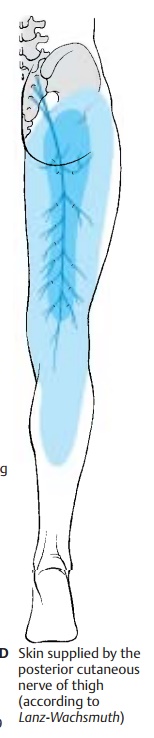
The nerve leaves the pelvis together with sciatic nerve and inferior gluteus nerve through the infrapiriform foramen and reaches below the gluteus maximus muscle to the posterior aspect of the thigh. Located directly beneath the fascia lata, it extends along the middle of the thigh into the pop-liteal fossa. This exclusively sensory nerve gives off branches to the lower part of the buttock, the inferior cluneal nerves, and to the perineal region, the perineal branches. It pro-vides sensory innervation to the posterior aspect of the thigh from the lower buttock region into the popliteal fossa and reaches to the proximal aspect of the lower leg.
Innervation of the skin (C, D).Autonomiczone (dark blue) and maximum zone (light blue).
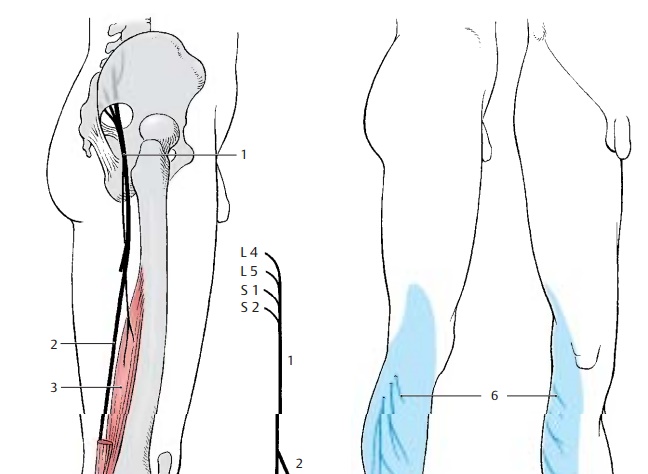
Sciatic Nerve (L4 – S3) (A – C)
The nerve has two components, the commonperoneal nerve (common fibular nerve) andthe tibial nerve; they appear as a uniform nerve trunk (AC1) because they are sur-rounded by a common connective-tissue sheath in the small pelvis and in the thigh. The sciatic nerve leaves the pelvis through the infrapiriform foramen and extends beneath the gluteus maximus muscle and biceps muscle along the posterior aspects of the internal obturator muscle, the quadrate muscle of femur, and the great adductor muscle in the direction of the knee joint. Peroneal nerve and tibial nerve separate above the knee joint. In the pelvis within the connective tissue sheath, the peroneal nerve is on the top and the tibial nerve below. In the thigh, the peroneal nerve lies laterally and the tibial nerve medially. However, both may run completely sepa-rately, in which case only the tibial nerve passes through the infrapiriform foramen, while the peroneal nerve penetrates the pir-iform muscle.
Common peroneal nerve (common fibu-lar nerve) (L4 – S2). In the thigh, the per-oneal part (AC2) of the sciatic nerve gives off a muscular branch to the short head of the biceps muscle of the thigh (A3).
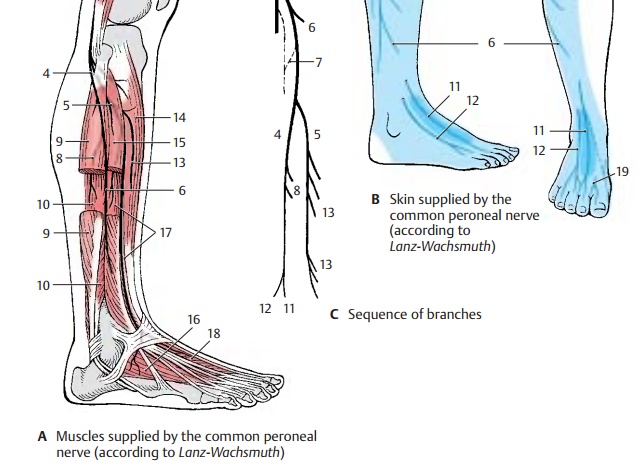
After division of the sciatic nerve, the com-mon peroneal nerve extends along the bi-ceps muscle at the lateral edge of the pop-liteal fossa to the head of the fibula. It then winds around the neck of the fibula to the anterior aspect of the lower leg and enters into the long peroneal (fibular) muscle. The common peroneal nerve divides within this muscle into the superficial peroneal nerve (AC4) and the deep peroneal nerve (AC5). The superficial peroneal nerve is predomi-nantly sensory and runs between the long peroneal muscle and the fibula to the back of the foot. The deep peroneal nerve is pre-dominantly a motor nerve; it turns toward the front to the extensor muscles of the lower leg and extends on the lateral surface of the anterior tibial muscle to the back of the foot.
At the lateral margin of the popliteal fossa, the common peroneal nerve gives off two main branches for the skin, the lateral suralcutaneous nerve (A– C6), which supplies theskin at the lateral aspect of the lower leg, and the fibular communicating branch (C7), which joins the medial sural cutaneous nerve to form the sural nerve.
The superficial peroneal nerve gives off muscu-lar branches (AC8) to the long (A9) and short(A10) peroneal muscles. The rest of the nerve is exclusively sensory; it ramifies into terminal branches, the medial dorsal cu-taneous nerve (BC11) and the intermediate dorsal cutaneous nerve(BC12), which supplythe skin of the back of the foot except for the interdigital space between great toe and second toe.
The deep peroneal nerve gives off several muscular branches (AC13) to the extensor muscles of the lower leg and the foot, namely, to the anterior tibial muscle (A14), the long (A15) and short (A16) extensor muscles of toes, and the long (A17) and short (A18) extensor muscles of the great toe. The terminal branch is sensory and sup-plies the apposing skin surfaces of the inter-digital space between great toe and second toe (B19).
Clinical Note: Injury to the nerve affects theextensor muscles of the foot. The foot can no longer be lifted in the ankle joint. When walking, the foot hangs down and the toes drag along the floor. The leg must be lifted higher than normal, resulting in the so-called steppage gait.
Innervation of the skin (B).Autonomiczone (dark blue) and maximum zone (light blue).
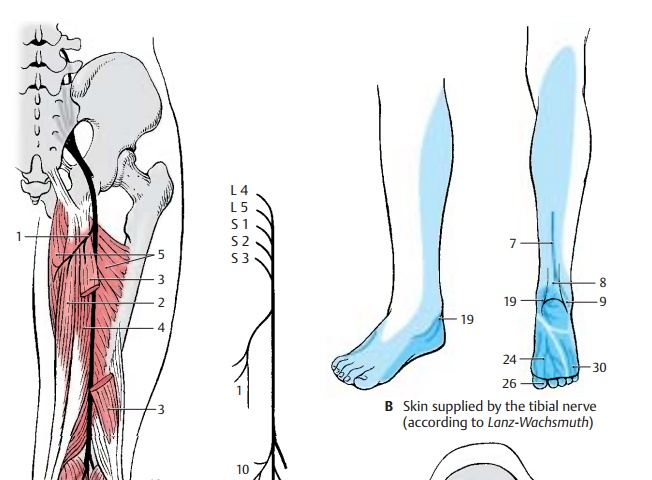
Sciatic Nerve (continued) (A – D)
Tibial nerve (L4 – S3). Severalmotorbranches (AC1) originate from the tibial por-tion of the sciatic nerve, namely, those for the proximal and distal parts of the semi-tendinous muscle (A2), for the long head of the biceps muscle (A3), and a branch divid-ing further for the semimembraneous muscle (A4) and the medial part of the great adductor muscle (A5).
After the division of the sciatic nerve, the tibial nerve descends vertically through the middle of the popliteal fossa and under-neath the gastrocnemius muscle. It then lies under the tendinous arch of the soleus muscle and, further distal, between the long flexor muscle of the great toe and the long flexor muscle of toes. It extends between the tendons of both muscles to the back of the medial ankle and winds around it. Below the ankle, it divides into two terminal branches, the medial plantar nerve and the lateral plantar nerve.
The medial sural cutaneous nerve (C6) branches off in the popliteal fossa; it de-scends between the two heads of the gastrocnemius muscle and joins the com-municating branch of the peroneal nerve to form the sural nerve (BC7). The latter extends laterally from the Achilles tendon behind the lateral ankle and around it to the lateral aspect of the foot. It gives off the lateral cal-caneal branches (BC8) to the skin of thelateral side of the heel and the lateral dorsalcutaneous nerve (BC9) to the lateral aspect ofthe foot.
Also in the popliteal fossa, motor branches (AC10) go off to the flexor muscles of the lower leg, namely, to the two heads of the gastrocnemius muscle (A11), to the soleus muscle (A12), to the plantar muscle and the popliteal muscle (A13). The popliteal branch gives rise to the interosseous nerve of the leg (C14), which runs along the dorsal surface of the interosseous membrane and provides sensory innervation to the periosteum of the tibia, the upper ankle joint, and the tib-iofibular joint. The tibial nerve gives offmuscular branches (C15) to the posteriortibial muscle (A16), the long flexor muscle of toes (A17), and the long flexor muscle of the great toe (A18). Before the nerve trunk ramifies into terminal branches, it sends off the medial calcaneal branches (B19) to the me-dial skin area of the heel.
The medial of the two terminal branches, the medial plantar nerve (CD20), innervates the abductor muscle of the great toe (D21), the short flexor muscle of toes (D22), and the short flexor muscle of the great toe (D23). Finally, it divides into the three com-mon plantar digital nerves (BC24), whichsupply lumbrical muscles 1 and 2 (D25) and divide further into the proper plantar digital nerves (BC26 ) for the skin of the interdigital spaces from the great toe up to the fourth toe.
The second terminal branch, lateral plantarnerve (CD27), divides into a superficial branch (C28) with the common plantar digitalnerves (C29) and proper plantar digital nerves (BC30) for the skin of the little toearea and into a deep branch (CD31) with the muscular branches for the interosseousmuscles (D32), the adductor muscle of great toe (D33 ) and the three lateral lumbrical muscles. D34, short flexor muscle of the little toe.
Clinical Note: Injury of the tibial nerve leadsto paralysis of the flexor muscles of toes and foot. The foot can no longer be moved in plantar direc-tion: tiptoeing becomes impossible.
Innervation of the skin (B).Autonomiczone (dark blue) and maximum zone (light blue).
Pudendal Nerve (S2 – S4) (A, B)
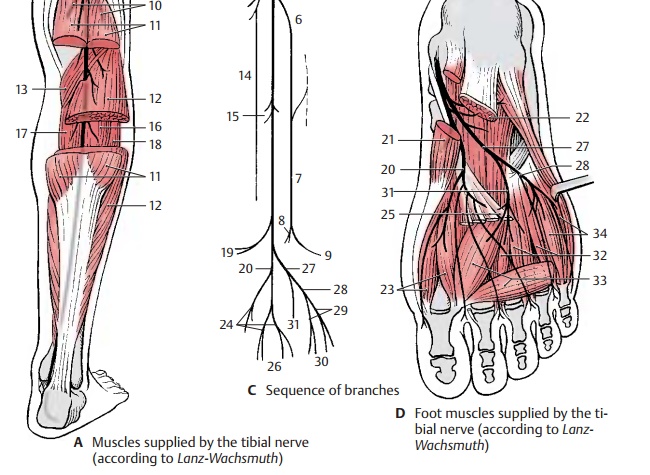
The pudendal nerve (AB1) leaves the pelvis through the infrapiriform foramen (AB2), extends dorsally around the sciatic spine (AB3) and passes through the lesser sciatic foramen (AB4) into the ischioanal fossa. It then runs along the lateral wall of the fossa within the pudendal canal (Alcock’s canal) to below the symphysis, sending its terminal branch to the dorsal side of the penis or cli-toris, respectively.
Numerous branches are given off in the pu-dendal canal; the inferior rectal nerves (A – C5), which may also originate directly from the second to fourth sacral nerves, penetrate through the wall of the canal to the perineum and supply motor fibers to the external sphincter muscle of anus (AB6) and sensory fibers to the skin around the anus as well as the lower two-thirds of the anal canal.
The perineal nerves (AB7) subdivide into deep and superficial branches. The deep branches participate in the innervation of the external sphincter muscle of the anus. More superficially, they supply the bulbo-cavernous muscle, the ischiocavernous muscle, and the superficial transverse per-ineal muscle. The superficial branches supply sensory fibers to the posterior part of the scrotum (posterior scrotal nerves) (AC8) in males and to the labia majora (posterior labial nerves) (BC9) in females. They also supply the mucosa of the urethra and the bulb of penis in males, and the external urethral opening and the vestibule of vagina in females.
The terminal branch, the dorsal nerve of thepenis (A10) or dorsal nerve of the clitoris (B11),respectively, sends motor branches to the deep transverse perineal muscle, the deep sphincter muscle, and the sphincter muscle of urethra (B12). After passing through the urogenital diaphragm (AB13), it gives off a branch to the cavernous body of the penis in males, and to the cavernous body of the cli-toris in females. In males, the nerve runs along the dorsum of the penis and gives offsensory branches to the skin of the penis and the glans. In females, it supplies sensory fibers to the clitoris including the glans.
Muscular Branches (S3, S4)
The levator ani muscle and the coccygeal muscle are supplied directly by nerve branches from the sacral plexus.
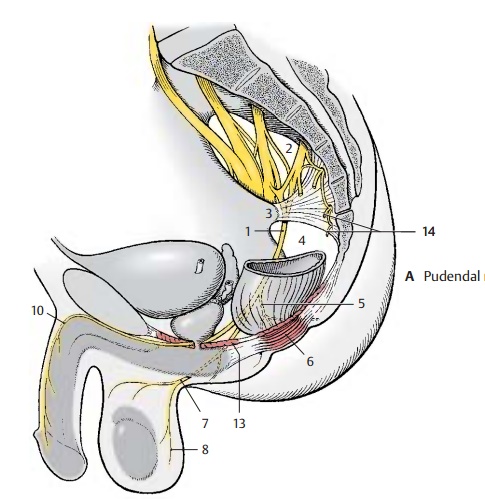
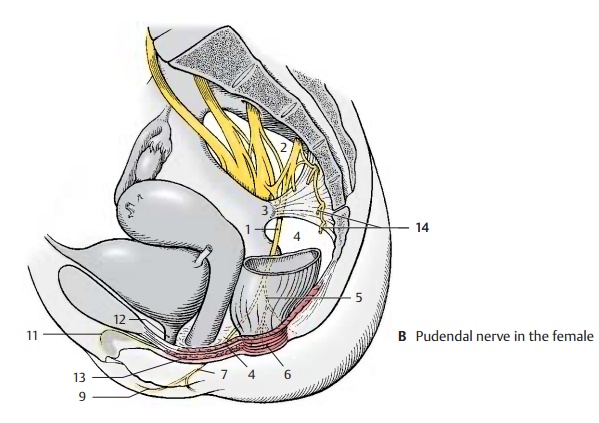
Coccygeal Plexus (S4 – Co) (A – C)
The anterior branches of the fourth and fifth sacral nerves form a fine plexus on the coccygeal muscle, the coccygeal plexus (AB14). Theanococcygeal nerves originate from here; they supply sensory fibers to the skin over the coccyx and between coccyx and anus (C14).
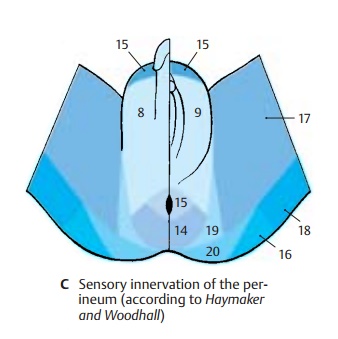
Sensory Innervation of Pelvis and Perineum (C)
In addition to the sacral and coccygeal nerves, the following nerves participate: the ilioinguinal nerve and the genitofemoral nerve (C15), theiliohypogastric nerve (C16),the obturator nerve (C17), the posterior cu-taneous nerve of the thigh (C18), the inferior cluneal nerves (C19), and themedial cluneal nerves (C20).
External openings of genitals, bladder, and rectum are border areas between involun-tary smooth intestinal muscles and volun-tary striated muscles. Accordingly, auto-nomic and somatomotor fibers are here in-tertwined. The pudendal nerve contains, apart from sensory, somatomotor, and sym pathetic fibers, also parasympathetic fibers from the sacral spinal cord. Sympathetic fibers also originate as pelvic splanchnic nerves from the second to fourth sacral nerves.
Related Topics