Chapter: Medicine and surgery: Hepatic, biliary and pancreatic systems
Nonalcoholic fatty liver disease
Nonalcoholic fatty liver disease
Definition
Nonalcoholic fatty liver disease (NAFLD) is a condition with histological features resembling alcohol-induced liver injury, occurring in patients with little or no history of alcohol consumption. The exact significance of NAFLD is currently unknown.
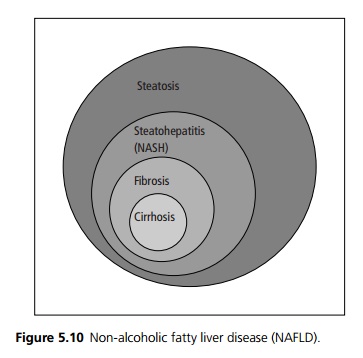
NAFLD encompasses a histological spectrum that ranges from fat accumulation in hepatocytes (hepatic steatosis) to hepatic steatosis with hepatic inflammation (nonalcoholic steatohepatitis or NASH) that may or may not have associated fibrosis, (see Fig. 5.10). NASH may progress to cirrhosis in up to 20% of patients.
Aetiology/pathophysiology
The pathogenesis of nonalcoholic fatty liver disease is not fully understood.
· Hepatic steatosis results from excessive triglyceride accumulation in the liver as a result of increased free fatty acid entering the liver, decreased free fatty acid leaving the liver or impaired beta-oxidation of free fatty acid. Insulin resistance appears to be important in the development of hepatic steatosis and steatohepatitis. Obesity, type II diabetes and insulin resistance are frequently seen in patients with NAFLD.
· Oxidative injury may be required for the development of hepatic inflammation and necrosis. Suggested mechanisms include increased hepatic iron, anti-oxidant deficiencies and intestinal bacterial over-growth.
Clinical features
Most patients are asymptomatic, fatigue, malaise and right upper abdominal discomfort may occur in some patients with NASH. Hepatomegaly is a frequent finding. Most cases are found on incidental abnormal liver function tests.
Complications
Histologic progression occurs in a small proportion of patients (up to 20%), a few of which progress to end-stage liver disease. Patients who develop cirrhosis may be at increased risk for hepatocellular carcinoma.
Investigations
Serum AST and ALT are raised (>90% of patients) and alkaline phosphatase is often normal as are serum bilirubin levels; however, patients with severely abnormal liver histology may have normal liver function tests. Ultrasound scan may indicate fatty infiltration. Liver biopsy is the only definitive method to diagnose or exclude NAFLD, although its exact role in the management of patients without definitive evidence of liver damage is undecided.
Management
Obesity, hyperlipidemia and diabetes should be managed; however, weight loss should be gradual as rapid weight loss may exacerbate the condition.
Potential treatments under investigation include vitamin E and C supplementation, oral hypoglycemic agents and ursodeoxycholic acid.
In the few patients who progress to end stage, liver failure transplantation may be required; however, recurrence in the transplanted liver has been reported.
Related Topics