Chapter: Medicine and surgery: Hepatic, biliary and pancreatic systems
Cirrhosis - Patterns of liver disease
Cirrhosis
Definition
Cirrhosis is an irreversible change of the liver architecture, characterised by nodules of regenerated liver cells separated by bands of fibrous scar tissue.
Aetiology
Cirrhosis results from continued hepatocellular necrosis and chronic inflammation. Fibrous scarring causes disruption of the normal architecture, although regeneration of hepatocytes occurs between the fibrous tracts, their function, which depends on intact architecture, is impaired.
· Alcohol accounts for more than 80% of cirrhosis in the United Kingdom.
· Viral hepatitis due to hepatitis B and C is the most common cause worldwide.
· Other conditions include primary biliary cirrhosis (PBC), autoimmune hepatitis, nonalcoholic steatohepatitis (NASH), haemachromatosis, α1antitrypsin disease, galactosaemia, cystic fibrosis, Wilson’s disease and drugs.
Pathophysiology
All the liver functions are impaired (bilirubin metabolism, bile salt synthesis, specialised protein synthesis, detoxification of hormones, drugs and toxins). Impaired blood flow through sinusoids leads to an exacerbation of the functional deficit and portal hypertension. Feminisation in males and amenorrhea in females are common in alcoholic liver disease and haemochromatosis due to alterations in the hypothalamic–pituitary–gonadal axis. Reduced immune competence and increased susceptibility to infection also occur.
Clinical features
Patients may present with complications such as bleeding from oesophageal varices or encephalopathy. Patients with active chronic hepatitis may present with features of chronic liver disease before cirrhosis is established. Signs of chronic liver disease:
1. General appearance: Jaundice, pigmented (haemochromatosis), pallor (anaemia), bruises (clotting abnormalities), petechiae (thrombocytopenia), scratch marks (pruritus), spider naevi on trunk, muscle wasting (malnutrition).
2. Hands: Leuconychia (if hypoalbuminaemic), clubbing, palmar erythema, Dupuytren’s contracture, hepatic flap (asterixis, sign of hepatic encephalopathy), tremor may occur in alcoholism and Wilson’s disease.
3. Abdomen: Dilated veins around the umbilicus, striae may result from abdominal distension. The liver is usually enlarged, firm and irregular, but is shrunken in late disease. The spleen may be enlarged due to portal hypertension. Ascites may be present.
Macroscopy
The liver is often enlarged and nodular, with a bosselated surface. The cut surface shows nodules of liver tissue, separated by fine or coarse fibrous strands. Micronodular cirrhosis consists of nodules less than 3 mm, if larger nodules are seen it is termed macronodular cirrhosis.
Complications
Bleeding oesophageal varices secondary to portal hypertension, hepatocellular carcinoma.
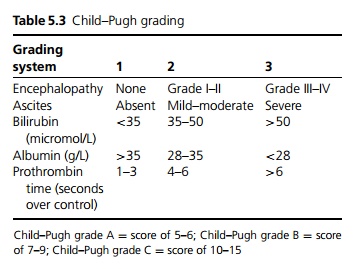
Child–Pugh grade A = score of 5–6; Child–Pugh grade B = score of 7–9; Child–Pugh grade C = score of 10–15
Investigations
Aimed at diagnosis of underlying cause and assessment of severity/degree of reversible liver injury. The severity of liver disease may be graded A–C by means of a modified Child–Pugh grading system (see Table 5.3). Liver biopsy is often required for assessment.
Management
Treatment is largely supportive. Withdrawal from alcohol is essential in all patients. Malnutrition is common and may require nutritional support. Liver transplantation may be required when end stage liver failure occurs.
Prognosis
Cirrhosis is an irreversible, progressive condition which often continues to end-stage liver failure despite the with-drawal of precipitating factors. The higher the Child– Pugh grade, the worse the prognosis, particularly for death from bleeding varices or following surgery.
Related Topics