Chapter: Essential Clinical Immunology: Immunological Aspects of Immunodeficiency Diseases
Clinical Manifestations of Antibody Deficiency
Clinical Manifestations of Antibody Deficiency
KEY CONCEPTS
1. Patients with antibody deficiency typi-cally develop recurrent infection with encapsulated bacteria such as Strep-tococcus pneumoniae and Haemophilus influenzae type B. The common sites affected are the upper and lower respi-ratory tracts and the middle ear. From these sites, infection can spread via the bloodstream to produce metastatic infections, for example, meningitis or bone and joint infection.
2. Structural lung damage (bronchiecta-sis, pulmonary fibrosis) can be a con-sequence of recurrent respiratory tract infections in inadequately treated, anti-body-deficient patients, and contributes to morbidity and mortality.
3. Once respiratory tract damage is estab-lished, patients are prone to sinopul-monary sepsis caused by nontypeable Haemophilus influenzae strains.
4. Overgrowth of commensal bacteria in the small intestines or chronic infection by intestine pathogens (Giardia, Salmo-nella, Campylobacter) may give rise to diarrhea or malabsorption secondary to villous atrophy.
5. In general, the course of uncomplicated viral infection (chicken pox, measles, etc.) is not significantly different from those in normal individuals, indicat-ing that antibody production is not essential for recovery from acute viral infections. However, long-term immu-nity, which depends on the ability to develop neutralizing antibodies does not develop and the infections can recur.
6. Fungal and intracellular bacterial infec-tions are not a feature of antibody deficiency.
7. About a fifth of patients with antibody deficiency due to common variable immune deficiency (which is described in a later section) develop autoimmune disorders. These include autoimmune hematological disorders (hemolytic ane-mia, autoimmune thrombocytopenia, pernicious anemia), autoimmune endo-crinopathies (e.g., thyroid disease) or neurological diseases such as Guillain-Barré syndrome, and, rarely, a lupus-like syndrome.
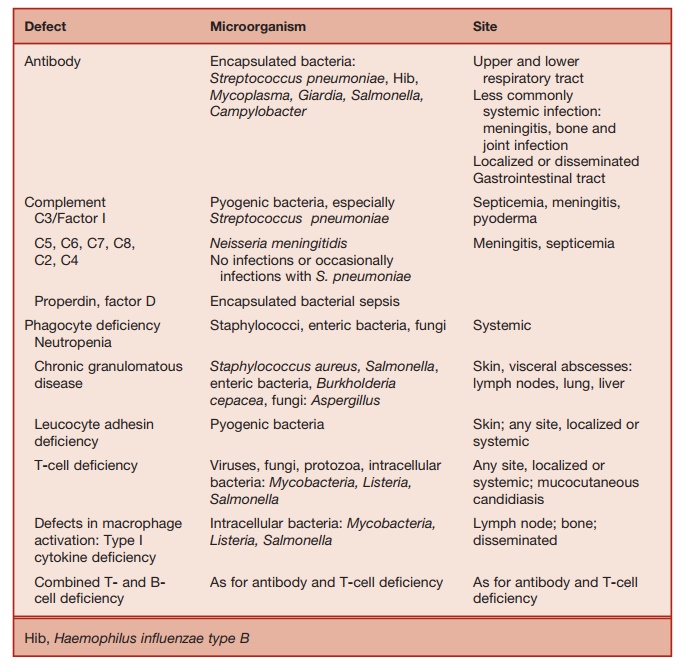
Table 5.3 Pattern of Microbial Infection in Immunodeficiency
Related Topics