Chapter: Essential Anesthesia From Science to Practice : Applied physiology and pharmacology : Anesthesia and the lung
The work of breathing
The work of breathing
The medullary centers control the PaCO2 by altering the minute ventilation (V˙E ):
V˙E= VT× f
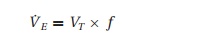
where VT= tidal volume and f= respiratory rate. How these parameters change to maintain minute ventilation depends on the work of breathing. Because inhaling requires the work of muscles, it is “costly,” in an energy expenditure sense, to breathe. In general, a few large breaths are more efficient than many small ones because all breaths must move the same amount of deadspace volume (about 150 mL for the average adult, see below). Endotracheal tubes offer much resistance and can greatly increase the work of breathing. The ventilator will ease this burden by doing the inspiratory work for the patient. Just as with all other muscles, disuse leads to reduced strength and stamina. Several investigators continue to study the optimal amount of respiratory muscle loading to prevent muscle atrophy and weaning difficulties.
Patients with low pulmonary compliance, e.g., pulmonary fibrosis, tend to breathe rapidly with low tidal volumes because of the great work required to expand a stiff lung. Compliance (C ) describes the relationship between volume (V) and pressure (P) in any enclosed space (lung, cardiac ventricle):
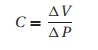
Conversely, a patient with high airway resistance cannot move air rapidly through the bronchial tree and tends to breathe slowly, which decreases turbulence. The resulting shift toward laminar movement of air increases flow.
Since resistance decreases as the fourth power of the radius, we can easily see why even a small amount of bronchospasm so drastically affects air movement, and why babies with subglottic edema present us with such great difficulties.
Related Topics