Chapter: Basic Radiology : Imaging of the Heart and Great Vessels
Techniques and Normal Anatomy : Computed Tomography
Computed
Tomography
Cardiac computed tomographic angiography
has undergone a revolution over the past decade. Owing to improved detec-tors,
increased detector rows, and decreased scan times, breath-hold imaging of the
heart can now be performed in many cases without pharmaceutical intervention
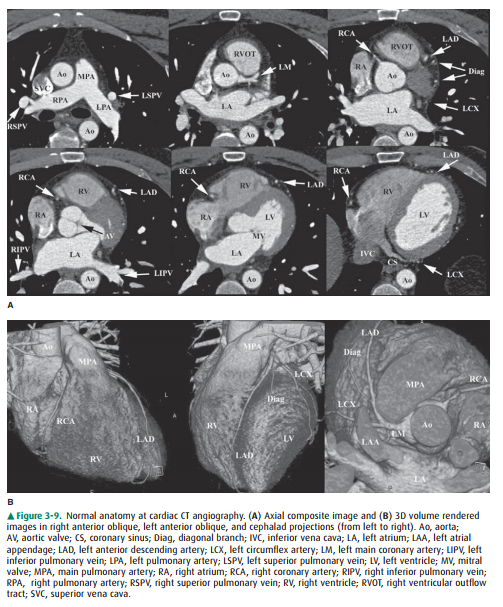
(Figure 3-9). The major indications for cardiac CT are to evaluate the coronary
arteries in subjects with indeterminate nuclear stress tests, to characterize
or confirm coronary or cardiac anomalies, to assess location and patency of
bypass grafts, and, in some cases, to assess for the presence of
atherosclerotic dis-ease in subjects presenting to the emergency department
with atypical chest pain. The last is often performed with an ex-tended
coverage of the chest to concomitantly evaluate for pul-monary embolism and
aortic dissection (triple rule-out). At the present time, some physicians also
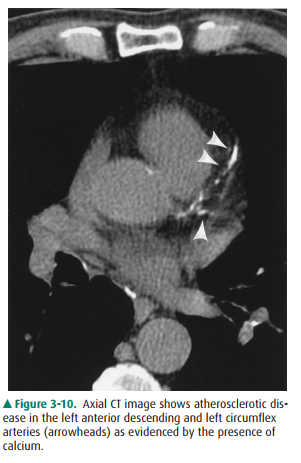
use the measurement of calcium in the coronary arteries detected at unenhanced
ECG-gated CT to stratify the risk of future cardiovascular events (Figure
3-10). Contrast administration is mandatory when there are questions related to
intrinsic cardiac anatomy or abnormalities of the thoracic aorta such as
dissection or for evaluation of the pulmonary arteries for pulmonary em-bolism.
For many of these applications, rapid administration of contrast is necessary
(up to 4–5 mL per second), and a well-functioning large-bore (at least 18- to
20-gauge) IV catheter must be present to ensure a high-quality study.
The major drawback to CT for
cardiac imaging at present is the use of ionizing radiation, which without
careful man-agement can be 4 to 5 times higher than for a standard chest CT.
Fortunately, many techniques have been developed that lower radiation exposure.
These include, but are not limited to, limiting scan distance, pulsing the
x-rays to limit exposure during systole, prospectively gating rather than
retrospec-tively reconstructing oversampled data, and modulating the x-ray beam
based on patient size.
Related Topics