Morphology, Cultural Characteristics, Virulence Factors, Pathogenicity, Laboratory Diagnosis, Treatment - Staphylococcus Aureus (Pyogenic Cocci) | 12th Microbiology : Chapter 7 : Medical Bacteriology
Chapter: 12th Microbiology : Chapter 7 : Medical Bacteriology
Staphylococcus Aureus (Pyogenic Cocci)
Staphylococcus Aureus (Pyogenic Cocci)
The genus
Staphylococcus is included in the
family Micrococcaceae. Staphylococcus
is a normal flora of skin and mucous membranes, but it accounts for human
infections, which is known as staph infection. The name Staphylococcus was derived from a Greek word, ‘staphyle’ means bunch of
grapes and ‘kokkos’ means berry. Staphylococcus aureus is a pathogenic species that causes pyogenic
infections in human.
Morphology
• Staphylococci
are gram
positive spherical cocci, (0.8µm–1.0µm
in diameter) arranged characteristically in grape like clusters (Figure 7.1).
• They
are non-motile and non-sporing and few strains are capsulated.
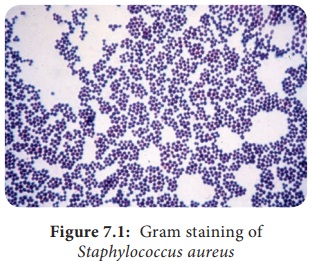
The grape like cluster formation in
Staphylococcus aureus is due to cell division occurring in three perpendicular
planes, with daughter cells tending to be remaining in close proximity.
Cultural Characteristics
• They are aerobes and facultative anaerobes,
optimal temperature is 37°C and optimum pH is 7.4–7.6.
• They grow on the following media and shows the
characteristic colony morphology (Table 7.1 & Figure 7.2).
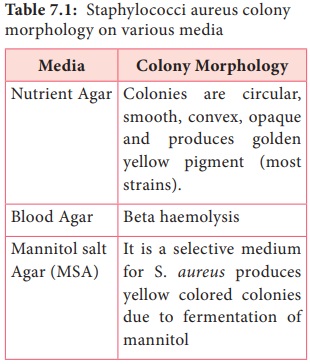
Table 7.1: Staphylococci aureus colony morphology on various
media
Media Colony: Morphology
Nutrient Agar: Colonies are circular, smooth,
convex, opaque and produces golden yellow pigment (most strains).
Blood Agar: Beta haemolysis
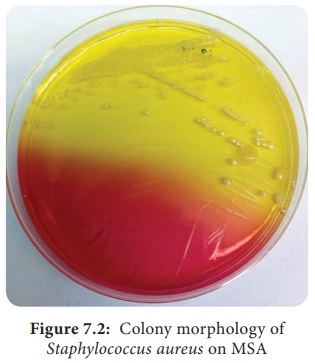
Mannitol salt Agar (MSA): It is a
selective medium for S. aureus produces yellow colored colonies due to
fermentation of mannitol
Virulence Factors
1. Peptidoglycan
→ It is a polysaccharide polymer. It activates complement and induces the
release of inflammatory cytokines
2. Teichoic
acid → it facilitates adhesion of cocci to the host cell surface. Protein A →
It is chemotactic, antiphagocytic, anticomplementary and induce platelet injury.
3. Toxins:
• Hemolysins
– It is an exotoxin, those lysis red blood cells. They are of four types namely
α-lysin, β-lysin, γ-lysin and delta lysin.
• Leucocidin
– It damages PMNL (polymorphonuclear leucocytes) and macrophages.
• Enterotoxin
– It is responsible for manifestations of Staphylococcus food poisoning.
• Exfoliative
toxin – This toxin causes epidermal splitting resulting in blistering diseases.
• Toxic
shock syndrome toxin – TSST is responsible for toxic shock syndrome.
5. Enzymes: S. aureus produces several enzymes, which are
related to virulence of the bacteria.
• Coagulase
– It clots human plasma and converts fibrinogen into fibrin.
• Staphylokinase
– It has fibrinolytic activity.
• Hyaluronidase
– It hydrolyzes hyaluronic acid of connective tissue, thus facilitates the
spread of the pathogens to adjacent cells.
• Other
enzymes – S. aureus also produces lipase, nucleases and proteases
Pathogenicity
S. aureus is an opportunistic pathogen
which causes infection most commonly at sites of lowered host resistance.
(Example: damaged skin)
Mode of
Transmission: Staphylococcus
infections are transmitted by the following ways.
HOTS
Why many hospitalized patients are at increased risk for opportunistic infection?
Staphylococcal diseases may be classified as
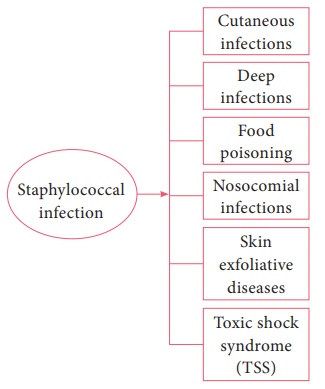
It
includes the following infections, which are as follows:
Cutaneous infections: Wound
(injury), burn infections (tissue
injury caused by heat), pustules (A small elevated skin lesions containing
pus), furuncles (boil forms around a hair follicle and contains pus), styes (a
painful swelling of hair follicle at eyelids), carbuncles (painful cluster of
boils of the skin), Impetigo (skin infection with vesicles, pustules which
ruptures), pemphigus neonatorum (an auto immune diseases that affect skin and
mucous membranes)
Deep infections: It includes Osteomyelitis (inflammation of bones), tonsillitis (inflammation
of tonsils), pharyngitis (inflammation of pharynx) sinusitis (inflammation of
sinuses), periostitis (inflammation of membrane covering bones),
bronchopneumonia (inflammation of lungs), empyema (collection of pus in the
body cavity), septicemia (blood poisoning caused by bacteria and its toxins),
meningitis (inflammation of meninge), endocarditis (inflammation of
endocardium), breast and renal abscess. Food
Poisoning: Staphylococcal food poisoning
may follow 2–6 hours after the ingestion of contaminated food (preformed
enterotoxin). It leads to nausea, vomiting and diarrhea.
Nosocomial infection: S. aureus is a leading cause of
hospital acquired infections. It is the primary cause of lower respiratory
tract (LRT) infections and surgical site infections and the second leading cause
of nosocomial bacteremia,pneumonia, and Cardiovascular infections.
Exfoliative
diseases: These diseases are
produced due to the production of epidermolytic toxin. The toxin separates the
outer layer of epidermis from the underlying tissues leading to blistering
disease. The most dramatic manifestation of this toxin is scalded skin
syndrome. The patient develops painful rash which slough off and skin surface
resembles scalding.
HOTS: Why most infections acquired through the skin are
non-communicable diseases?
Toxic shock syndrome toxin: It is caused by TSST-1 and characterized by high fever, hypotension (low blood pressure), vomiting, diarrhea and erythematous rash. TSS became widely known in association with the use of vaginal tampons by menstruating women but it occurs in other situations also.
Laboratory Diagnosis
Specimens: The clinical specimens are collected according to the nature of Staphylococcal infections,
which is given in the (Table 7.2).
Table 7.2: Clinical specimen collected for Staphylococcal infections
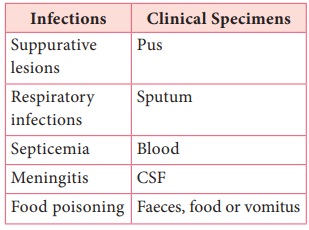
Specimens should be transported immediately to the laboratory and processed.
Direct Microscopy: Gram
stained smears of clinical specimens
is done, where gram positive cocci in clusters were observed.
Culture: The
collected specimen is inoculated on
selective media-MSA and the media incubated at 37°C for 18–24 hours. Next day
culture plates are examined for bacterial colonies, which are identified by
gram staining, colony morphology and biochemical tests such as
a.
Catalase test: The genus Staphylococci are catalase positive. This test distinguishes Staphylococcus from Streptococcus (catalase negative)
b.
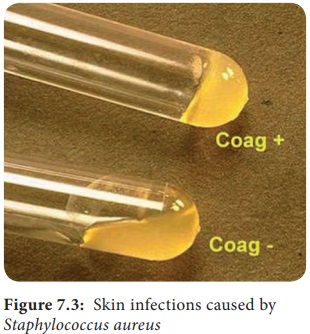
Coagulase
test: This test helps in differentiating a pathogenic strain from
non-pathogenic strain. S. aureus is
coagulasepositive (Figure 7.3).
Treatment
Benzyl
penicillin is the most effective antibiotic. Cloxacillin is used against beta
lactamase. Producing strains (β-lactamase is produced by few strains of S. aureus which cleaves β – lactam ring of
penicillin). Vancomycin is used against MRSA (Methicillin Resistant Staphylococcus aureus) strains.
Topical applications: For mild superficial lesions, topical applications
of bacitracin or chlorhexidine is recommended.
Control measures: Proper sterilization of medical instruments must be done.
Intake of antibiotics must be taken under proper medical advice. The detection
of source & carriers among hospital staff, their isolation and treatment
should be practiced.
Related Topics