Chapter: Psychiatric Mental Health Nursing : Child and Adolescent Disorders
Related Disorders - Dementia
RELATED DISORDERS
Amnestic disorders are characterized by a
disturbance in memory that results
directly from the physiologic effects of a general medical condition or the
persisting effects of a substance such as alcohol or other drugs (APA, 2000).
The memory disturbance is sufficiently severe to cause marked impairment in
social or occupational functioning and repre-sents a significant decline from
previous functioning. Con-fusion, disorientation, and attentional deficits are
common. Clients with amnestic disorders are similar to those with dementia in
terms of memory deficits, confusion, and prob-lems with attention. They do not,
however, have the multi-ple cognitive deficits seen in dementia, such as
aphasia, apraxia, agnosia, and impaired executive functions.
Several medical conditions can cause brain damage and result in an
amnestic disorder—for example, stroke or other cerebrovascular events, head
injuries, and neuro-toxic exposures, such as carbon monoxide poisoning, chronic
alcohol ingestion, and vitamin B12 or thiamine deficiency.
Alcohol-induced amnestic disorder results from a chronic thiamine or vitamin B
deficiency and is called Korsakoff’s
syndrome.
The main difference between dementia and amnestic disorders is that
once the underlying medical cause is treated or removed, the client’s condition
no longer dete-riorates. Treatment of amnestic disorders focuses on
elimi-nating the underlying cause and rehabilitating the client and includes
preventing further medical problems. Some amnestic disorders improve over time
when the underly-ing cause is stabilized. Other clients have persistent
impair-ment of memory and attention with minimal improvement; this can occur in
cases of chronic alcohol ingestion or mal-nutrition (Grossman, 2005). Nursing
diagnoses and inter-ventions are similar to those used when dealing with the
memory loss, confusion, and impaired attention abilities of clients with
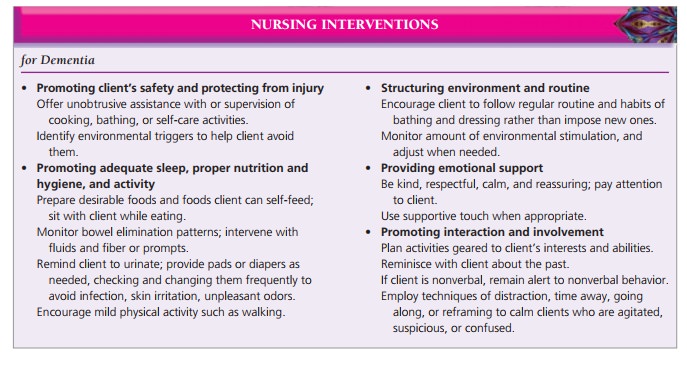
dementia or delirium (see Nursing Interven-tions for Dementia).
Related Topics