Chapter: Paediatrics: Infectious diseases
Paediatrics: Immunizations
Immunizations
•
Immunizations
are an important part of child health in the community.
•
Immunization
should be delayed in the acutely ill child.
•
In
those where there is a family history of febrile convulsion, advice should be
given about control of fever with antipyretics, and when to seek medical
assistance.
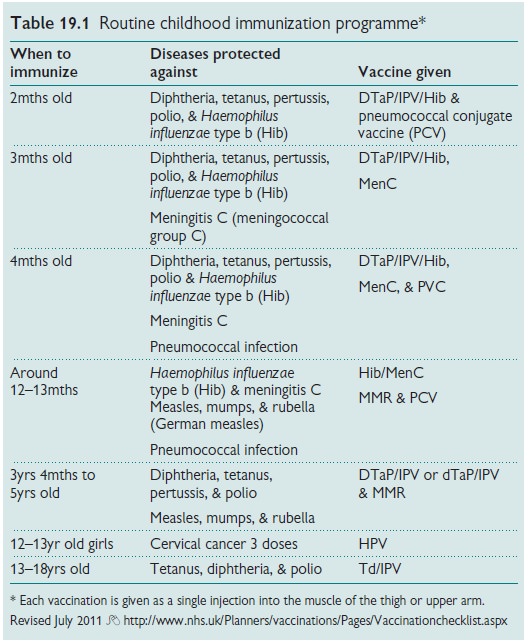
Schedule
The schedule for vaccinations to
be given to an infant growing up in the
UK is as follows:
•
BCG: birth in at-risk groups (e.g.
those living in areas of high rate of TB,
or those whose parents/grandparents were born in a TB high-prevalence country).
· Hepatitis
B:
•
birth,
1mth, 2mths in at risk groups;
•
12,
15, and 18mths in at risk groups.
•
Diphtheria, pertussis, tetanus (DPT):
•
2, 3,
and 4mths in all infants;
•
booster
at 3yrs 4mths to 5yrs old;
•
booster
for only diphtheria and tetanus at 13–18-yr-olds.
•
Inactivated polio virus:
•
2, 3,
and 4mths in all infants.
•
boosters
at 3yrs 4mths to 5yrs, and 13–18yrs
•
Haemophilus influenzae type b: 2, 3, 4, and 12–13mths in all infants.
•
Neiserria meningitidis
(meningococcus) C: 3, 4
and 12–13mths in all infants.
•
Pneumococcal conjugate vaccine: 2, 4, and 12–13mths in all
infants.
•
Measles, mumps, rubella (MMR):
•
12–13mths
in all infants;
•
booster
at 3yrs 4mths to 5yrs.
•
Human papilloma virus (HPV,
against cervical cancer): 3
doses within 6mths in girls
12–13-yr-old.
Live vaccines are contraindicated
in children with immunodeficiency. Pertussis immunization is contraindicated in
infants who have had a severe local or general reaction to a previous
injection. MMR is contraindicated in children allergic to excipients such as
gelatin and neomycin.
Related Topics