Chapter: Medicine and surgery: Haematology and clinical Immunology
Non-Hodgkin’s lymphoma
Non-Hodgkin’s lymphoma
Definition
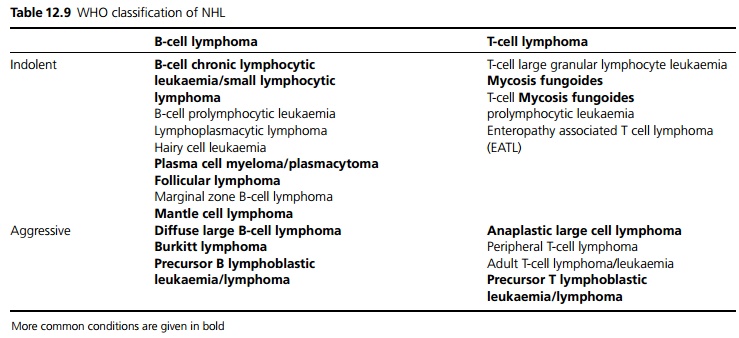
Non-Hodgkin’s lymphoma (NHL) is a tumour originating from lymphoid tissue. NHL includes many subtypes but can be subdivided into indolent and aggressive lymphomas (see Table 12.9).
Incidence
20 per 100,000 per year.
Age
Median age at diagnosis 65 years.
Sex
1.5 M : 1F
Aetiology
Most NHLs are of B-cell origin. Tumours arise due to multiple genetic lesions affecting protooncogenes or tumour suppressor genes. Multiple chromosomal translocations have been identified. Other factors include viruses (Epstein-Barr virus particularly associated with Burkitt lymphoma), enviromental factors, congenital and acquired immunodeficiency and some autoim-mune conditions. Helicobacter pylori is associated with primary gastrointestinal lymphomas.
Clinical features
Indolent: Most patients present with painless slowly progressive lymphadenopathy. Lymph nodes may reduce in size spontaneously making it difficult to distinguish from reactive lymphadenopathy. B symptoms (fever >38◦ C, drenching night sweats, weight loss of more than 10% within 6 months) are not common at presentation. Bone marrow failure leads to anaemia, recurrent infections and bleeding. On examination there is lymphadenopathy and hepatosplenomegaly.
Aggressive lymphomas: Most patients present with lymphadenopathy, extranodal involvement (gastrointestinal tract, skin, genitourinary tract, thyroid and central nervous system) and B symptoms. On examination there is bulky lymphadenopathy and hepatosplenomegaly.
Mycosis fungoides (Sezary’s´ Syndrome) is a rare cutaneous T cell lymphoma. The cells are trophic to the skin particularly the hands and feet, and result in plaques and lumps of associated with generalised lymphadenopathy.
Extranodal lymphomas can occur at any site of lymphoid tissue (gastrointestinal tract, salivary glands, lung, thyroid, skin, gonads, bone and brain). Gas-trointestinal lymphoma is particularly common in the Middle East and is also seen in association with coeliac disease.
The staging of NHL is a measure of its extent and dis-tribution according to the Ann Arbor system, which is suffixed by B if B symptoms are present (see Table 12.8)

Investigations
The diagnosis is made by lymph node biopsy, cytogenetic studies of lymphoma cells may give prognostic informa-tion. Full blood count may show anaemia and throm-bocytopenia suggestive of marrow involvement. Staging involves CT scan of the abdomen and a chest X-ray or CT.
Management
Treatment is dependent on the nature and distribution of the lymphoma. Available options include chemotherapy, radiotherapy and monoclonal antibody treatment. The role of bone marrow transplantation is under investigation.
Prognosis
Indolent lymphomas have a predicted median survival time of 5–10 years. Aggressive lymphomas are more responsive to chemotherapy but have a predicted median survival 2–5 years.
Related Topics