Chapter: Medicine and surgery: Endocrine system
Multinodular goitre - Thyroid axis
Goitre
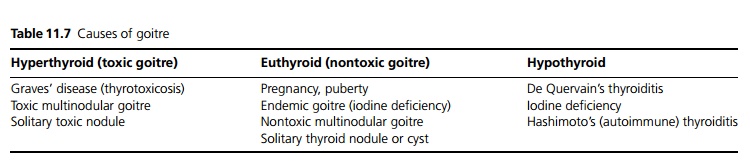
A goitre is a visible or palpable enlarged thyroid. The enlargement may be generalised enlargement or diffuse goitre; or may consist of single or multiple nodules. Further classification is based on whether the patient is hyperthyroid, euthyroid or hypothyroid (see Table 11.7) and below.
Multinodular goitre
Definition
Irregular multinodular enlargement of the thyroid gland, which may be hyperthyroid (toxic) or is commonly euthyroid (nontoxic).
Incidence/prevalence
25% of cases of thyrotoxicosis are due to multinodular goitre.
Age
Increases with age.
Sex
F > M
Aetiology
Unknown. May be due to varying response of the thyroid tissue to TSH over many years.
Clinical features
Patients may present for cosmetic reasons, with thyrotoxic symptoms, or because of complications. Multin-odular goitre can present with a particularly prominent thyroid nodule or a diffusely nodular gland. Most patients are euthyroid with a goitre, occasionally one or more nodules develop, which are TSH-independent and so cause thyrotoxicosis.
Macroscopy/microscopy
The thyroid is enlarged with irregular nodules of varying sizes. Nodules may be cystic, haemorrhagic and fibrosed. Microscopy reveals hyperplastic acini, with varying amounts of colloid.
Complications
Enlargement of the gland can cause tracheal compression leading to shortness of breath and choking. This is more common with retrosternal goitre, when the nodule(s) are in the isthmus. Toxic multinodular goitre has a particularly high incidence of cardiac arrhythmias and other cardiac complications.
Investigations
Thyroid function tests (TSH and thyroid hormone levels) are used to assess thyroid status. A chest X-ray can demonstrate any retrosternal mass or tracheal deviation. Ultrasound scanning of the thyroid may be useful to examine the structure of the thyroid and nature of lesions. Isotope scans are used to demonstrate areas of increased uptake in toxic multinodular goitres. Cysts and nodules may be aspirated by fine needle aspiration for cytology.
Management
Subtotal thyroidectomy may be required for cosmetic reasons or due to compression symptoms or thyrotoxicosis. Patients must be medically treated and euthyroid before surgery.
Related Topics