Chapter: Essentials of Anatomy and Physiology: The Reproductive Systems
Menstrual Cycle in Human
THE MENSTRUAL CYCLE
The menstrual cycle includes the activity of the hor-mones of the ovaries and anterior pituitary gland and the resultant changes in the ovaries (ovarian cycle) and uterus (uterine cycle). These are all incorporated into Fig. 20–9, which may look complicated at first, but refer to it as you read the following.
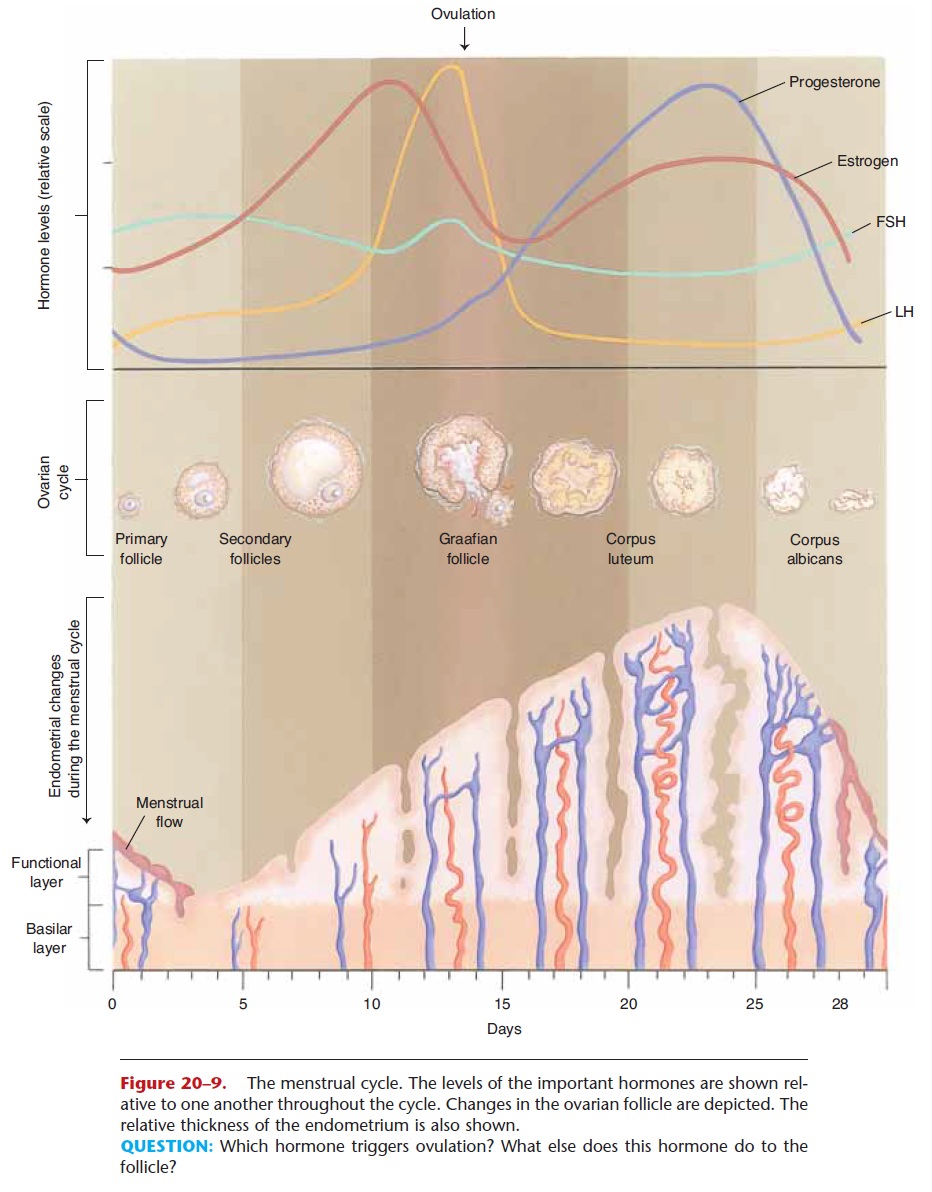
Figure 20–9. The menstrual cycle. The levels of the important hormones are shown rel-ative to one another throughout the cycle. Changes in the ovarian follicle are depicted. The relative thickness of the endometrium is also shown.
QUESTION: Which hormone triggers ovulation? What else does this hormone do to the follicle?
Notice first the four hormones involved: FSH and LH from the anterior pituitary gland, estrogen from the ovarian follicle, andprogesterone from the cor-pus luteum. The fluctuations of these hormones are shown as they would occur in an average 28-day cycle. A cycle may be described in terms of three phases: menstrual phase, follicular phase, and luteal phase.
Menstrual phase—The loss of the functional layer of the endometrium is called menstruation or the menses. Although this is actually the end of a menstrual cycle, the onset of menstruation is eas-ily pinpointed and is, therefore, a useful starting point. Menstruation may last 2 to 8 days, with an average of 3 to 6 days. At this time, secretion of FSH is increasing, and several ovarian follicles begin to develop.
Follicular phase—FSH stimulates growth of ovarian follicles and secretion of estrogen by the follicle cells. The secretion of LH is also in-creasing, but more slowly. FSH and estrogen pro-mote the growth and maturation of the ovum, and estrogen stimulates the growth of blood vessels in the endometrium to regenerate the functional layer.
This phase ends with ovulation, when a sharp increase in LH causes rupture of a mature ovarian follicle.
Luteal phase—Under the influence of LH, the ruptured follicle becomes the corpus luteum and begins to secrete progesterone as well as estrogen. Progesterone stimulates further growth of blood vessels in the functional layer of the endometrium and promotes the storage of nutrients such as glycogen.
As progesterone secretion increases, LH secre-tion decreases, and if the ovum is not fertilized, the secretion of progesterone also begins to decrease. Without progesterone, the endometrium cannot be maintained and begins to slough off in menstrua-tion. FSH secretion begins to increase (as estrogen and progesterone decrease), and the cycle begins again.
Also secreted by the corpus luteum during a cycle are the hormones inhibin and relaxin. Inhibin inhibits the secretion of FSH, and perhaps LH as well, from the anterior pituitary gland. Relaxin is believed to inhibit contractions of the myometrium (as does pro-gesterone), which would help make implantation of the early embryo successful.
The 28-day cycle shown in Fig. 20–9 is average. Women may have cycles of anywhere from 23 to 35 days, the normal range. Women who engage in stren-uous exercise over prolonged periods of time may experience amenorrhea, that is, cessation of menses. This seems to be related to reduction of body fat. Apparently the reproductive cycle ceases if a woman does not have sufficient reserves of energy for herself and a developing fetus. The exact mechanism by which this happens is not completely understood at present. Amenorrhea may also accom-pany states of physical or emotional stress, anorexia nervosa, or various endocrine disorders.
The functions of the hormones of female repro-duction are summarized in Table 20–3.

Related Topics