Chapter: Biology of Disease: Infectious Diseases and Treatments
Infections of the Gastrointestinal Tract
INFECTIONS OF THE
GASTROINTESTINAL TRACT
All regions of the gastrointestinal tract (GIT) are
subject to infection. Saliva traps and removes many pathogens and these can
also be killed by stomach acid . Unfortunately new ones are constantly
introduced through breathing and eating.
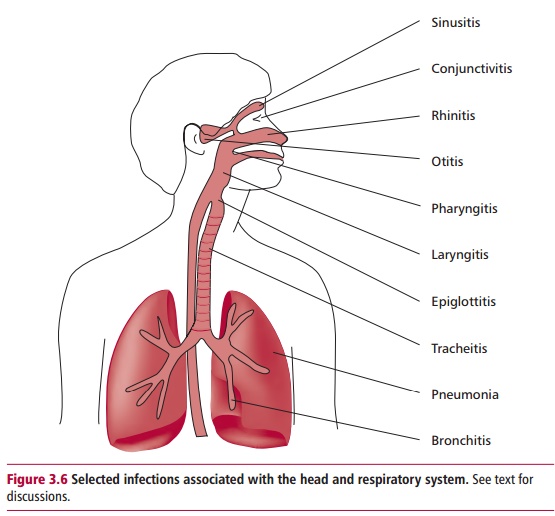
Infections of the oral cavity (Figure 3.6) differ in type and symptoms to those of the stomach and
intestines. Inflammation of oral tissues caused by fungal infection, actinomycosis, often occurs following
injuries, such as an accidental bite to the lining of the mouth or fracture of
the jaw. Immunosuppression resulting from viral infections, AIDS, cancer
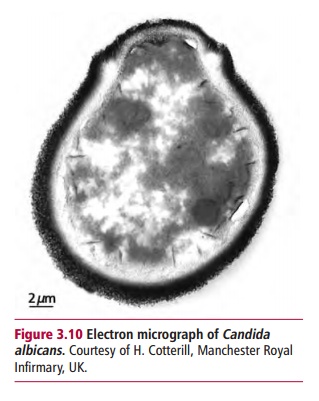
treatment or treatment with broad spectrum antibiotics can all allow the yeast Candida albicans (Figure3.10) to invade and colonize the mucous membrane, eventually
producing athick layer of yeast cells called candidiasis or thrush.
Some bacteria can resist removal by saliva and become
immobilized by binding to surface receptors of cells in the mouth, eventually
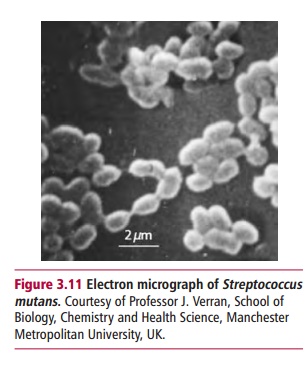
forming biofilms and microcolonies. Oral streptococci, such as Streptococcus sanguis and Streptococcus mutans (Figure 3.11), secrete
glycosyltransferases that mediatetheir adhesion to extracellular carbohydrates
on tooth surfaces leading to the formation of dental plaque, which is a complex
mixture of bacteria and extracellular materials. These bacteria, together with Actinomyces species, can cause caries by
forming plaque on the tooth enamel, where they catabolize sugars to produce acid
that demineralizes enamel and allows the dentine to be eroded. Abscesses of the
roots of teeth can also be caused by mixed bacterial infections.
Periodontal (gum) diseases are inflammatory
conditions that attack the gums, bone, and other supporting structures of the
teeth. The extent of the inflammatory response depends upon the types of
pathogens involved and the effectiveness of the immune response. However, they
are major causes of tooth loss in adults. Gingivitis is the earliest form of
periodontal disease and occurs when plaque accumulates on the teeth near the
gums, which become inflamed and bleed easily. If detected and treated early,
gingival tissues will return to normal without long-lasting damage. Untreated
gingivitis progresses to periodontitis, which is also known as pyorrhea. Plaque
hardens and extends from the gum line to the tooth root causing the gums to
detach from the teeth and form pockets. Periodontal pockets create room for
greater bacterial activity, particularly of facultative and obligate anaerobic
bacteria leading to a progressive cycle of tissue damage until eventually the
bone supporting the teeth is destroyed resulting in their loss.
Stomach and intestinal infections are caused by
viruses, bacteria, protozoa and worms, all of which may be transmitted in food,
contaminated drinking water or by fecal–oral contact. The need for strict
personal hygiene is emphasized because these are the most frequent infections
of children under five years of age. Approximately 40% of cases of diarrhea in
children are caused by rotaviruses (Figure
3.12). In the very young this is potentially lethal and the WHO has
estimated that out of the nearly two billion annual diarrhea diseases
worldwide, three million end fatally.
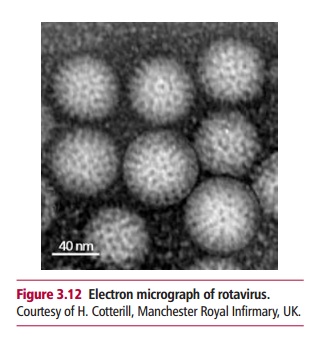
Figure 3.13 indicates a
number of pathogens that can infect the GIT. Theacidic environment and
proteolytic enzymes of the stomach kill most
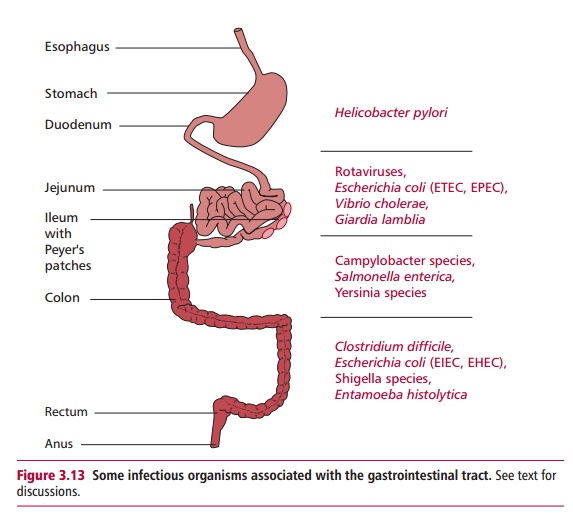
ingested microorganisms. However, the motile
bacterium, Helicobacterpylori has
specific receptors enabling it to bind to the gastricepithelium. It secretes
urease, which catalyzes the hydrolysis of urea releasing ammonia that
neutralizes stomach acid, and cytotoxins that damage the cells. This causes
chronic inflammation of the gastric mucosal membrane and can lead to stomach
and duodenal ulcers . The partially digested food (chyme) in the stomach is
made alkaline in the small intestine by secretions of the gut and pancreas and
by bile salts . In the ileum and jejunum, nonenveloped viruses, such as
rotaviruses and adenoviruses, may infect enterocytes and damage the intestinal
mucous membrane with disruption of water and electrolyte resorption. This can
result in intestinal cramps, vomiting, watery diarrhea and a raised
temperature. Enteropathogens, such as Vibrio
cholerae and forms of Escherichia
coli that are enterotoxic (ETEC) or enteropathogenic (EPEC) all have
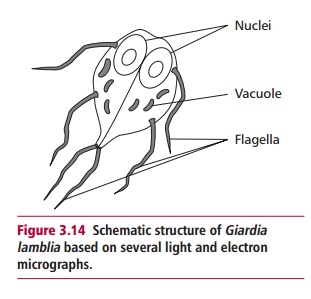
similar effects. The protozoan parasites Giardia
lamblia and Cryptosporidium parvum
are water-borne parasites that can infect the GIT. Giardia lamblia (Figure 3.14)
frequently causes chronic disease, with watery diarrhea and, in some cases, a
subfebrile temperature leading to malnutrition in children as a result of
malabsorption. Cryptosporidium parvum
can adhere to the epithelium of the small intestine and cause a shortening of
the villi, which may be the cause of the diarrhea.
The lower portion of the ileum has areas of lymphoid
tissue called Peyer’s patches (Figure
3.13) composed of so-called M (microfold) cells, rather than the usual
enterocytes and goblet cells . These cells are able to translocate materials
directly to the lymph follicles found beneath the mucosal surface. Invasive
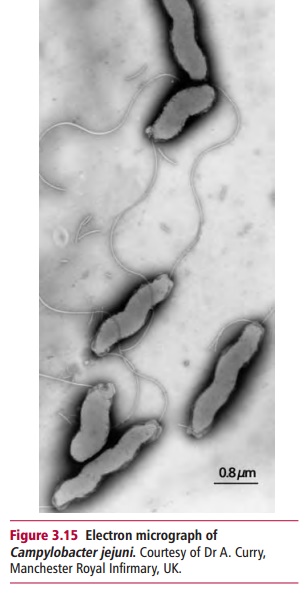
bacteria such as Campylobacter jejuni
(Figure 3.15), Salmonellae and
Yersiniae can use M cells to enter the submucosal area. Here they can multiply
and destroy the adjacent epithelium, form abscesses and spread through the
lymph and blood systems into the mesenteric lymph nodes, spleen and liver. The
infection can also spread into the colon, causing inflammation of the colon or colitis. The ileum and colon can also
be attacked by the bacteria Yersinia
enterocolitica, Salmonella enterica
and Campylobacterjejuni resulting in
abdominal cramps, vomiting, watery, occasionally bloody,diarrhea and fever. Shigella dysenteriae and Escherichia coli pathotypes, EHEC
(enterohemorrhagic) and EIEC (enteroinvasive) can cause a hemorrhagic colitis
with bloody stools and subfebrile to febrile temperatures. The pathogenic
protozoan Entamoeba histolytica is
thought to infect 50 million people and kill about 100 000 per year worldwide
due to amebic liver abscesses. Lastly, Clostridium
difficile, a normal inhabitant of the gut, is an opportunistic pathogen. It
is especially common in older people in hospitals and nursing homes and has
been implicated in iatrogenic infections following medical interventions, such
as antibiotic therapy. Infection with Clostridium
difficile is now recognized as the major causative agent of colitis and
diarrhea, which may occur following antibiotic intake and can be fatal in older
patients.
Related Topics